AI in Revenue Cycle Management: Streamlining Billing to Cash

Did you know hospitals make an annual loss of $5 million due to unresolved claims denials?
The revenue cycle of most hospitals is nothing short of a mess. From reimbursement time of 45-60 days, the money is often late or simply accounts for loss if not addressed. However, claim denials are not the only reason for the hospital’s revenue cycle mess; in fact, some studies suggest that around $250+ billion is lost due to administrative complexities or inefficiencies.
While many healthcare practices are adopting Revenue Cycle Management (RCM) software solutions to streamline their finances, they simply fall short due to many complexities. And those who have tried in-house solutions have finally admitted to the complexities that go around in claims submission and inefficiencies, etc.
However, some of the practices have taken a leap of faith and adopted an AI RCM automation solution, and surprisingly, have seen a steady increase in clean claim rates by a staggering 95%.
Sounds surprising to you, too?
Well, it is indeed true that billing automation AI solutions can literally simplify billing processes for you, and with a claims submission agent in place, it can even do what you want, just like you would do it.
Now, you have all the reasons to believe that this is all a little too far-featured, and it is now up to me to convince you of AI RCM automation solutions and, streamline your revenue cycle and improve the financial health of your practice.
On that note, let’s see how!
AI-Ready RCM Stages: Identifying Automation Opportunities
Every healthcare practice is different, and their requirements for claims submission and reimbursement requirements also vary from that of a generic healthcare practice. Now, AI is a wide concept, and for automation, you need to identify the opportunities that might be explored with AI RCM automation solutions.
1. Patient Registration & Eligibility Verification: Manually verifying a patient’s insurance and eligibility can be a time-consuming process, and the chances of error are also high. Here, billing automation AI can automate the insurance verification process, collect the necessary demographic data, and also set the system for the prior authorization process as well.
2. Charge Capture & Coding: Coding and charge entry automation can improve coding accuracy and ensure that the documentation required for coding and charges is complete. This automation can be used for revenue leak prevention with AI.
3. Claims Management & Submission: Managing claims and their submission is a process that has a lot of processes in it, like claims scrubbing, error detection, and optimal submission timing, depending on the requirement. This presents you with a perfect opportunity to deploy a claims submission agent that can fast-track claims management and submission with accuracy.
4. Denial Management & Appeals: If stats are to be believed, the chances of a healthcare claim being rejected is somewhere between 5% and 10%. This is where RCM denial tracking powered by AI can come into the picture. With an AI-powered denial pattern analysis, these claims can be easily managed, and revenue leak prevention AI can automate the appeal generation by eliminating the root cause of denial.
RCM Automation Readiness Checklist
Assess My SystemComprehensive AI Strategy: Pre-Claim, Claim & Post-Claim Automation
Claim submission is quite a lengthy process. At first, there is the pre-claim process that you need to streamline, then actually file the claim, and once they are filed, post-claim processes kick in, such as follow-ups, analysis, etc.
Now, here, a customized AI RCM automation solution gives you enough opportunities to instill itself in the claims submission process. Let’s see how you can leverage the extensive capabilities of a claims submission agent:
1. Pre-Claim Intelligence: The processes that come with pre-claim submission are patient eligibility verification, validating patient’s insurance coverage, and ensuring that they have prior authorization in place before the service is actually delivered. Here, a claims submission agent can easily verify, validate, and ensure everything before claims submission.
2. Claims Optimization: One of the aspects that has a huge margin of human error is claim filing. Just like in the prior process, an AI-powered claims submission agent can automate claim creation, validate and automate the coding of CPT and ICD based on the documents, and submit the claim in time to avoid any denials.
3. Post-Claim Management: Once the claims are submitted, the post-claim management process involves tracking and analyzing the claim in case of denial and automating follow-up for outstanding claims. Seems like a tiring process, right? Well, it is, and that is why RCM denial tracking with claims submission agents can assist you in each and every process.
Complete RCM AI Strategy Guide – Phase-by-Phase Implementation Plan
Free DownloadSpeed & Accuracy Revolution: Faster Reimbursement Through AI
If you have been following this article, then you must know that billing for healthcare in this age is quite a lengthy and time-consuming process. Moreover, you are somewhere at war with time, so ensuring accuracy and timing is essential. And speed and accuracy being some of the core competencies of an AI RCM automation solution, here are some ways in which it can bring speed and accuracy to your billing process:
1. Clean Claim Rate Optimization: While scratching the surface of the internet about AI systems submitting claims, some case studies suggested that 95% acceptance can be achieved. Though it seems a little far-featured, it can be done through intelligent error detection and correction.
2. Accelerated Payment Processing: For accelerating the payment process, automated payment posting is not enough; you also need to reconcile EOB (explanation of benefits). For this, along with a claims submission agent, you would need an EOB GenAI parser so that payment processing can be accelerated.
3. Predictive Analytics for Cash Flow: Analysis is another core competency of AI models. Bringing this into your AI RCM automation solutions, you can easily forecast payment timelines, identify payment collection risks beforehand, and optimize finances accordingly.
4. Payer-Specific Intelligence: As an individual payer, there are certain payer requirements and processing patterns that you are used to. Now, by deploying a machine learning system, payer-specific needs can also be met, further streamlining your billing processes.
Cash Flow Acceleration Calculator: Measure AI RCM Impact
CalculateSeamless Integration: Connecting AI RCM with EHR & Billing Systems
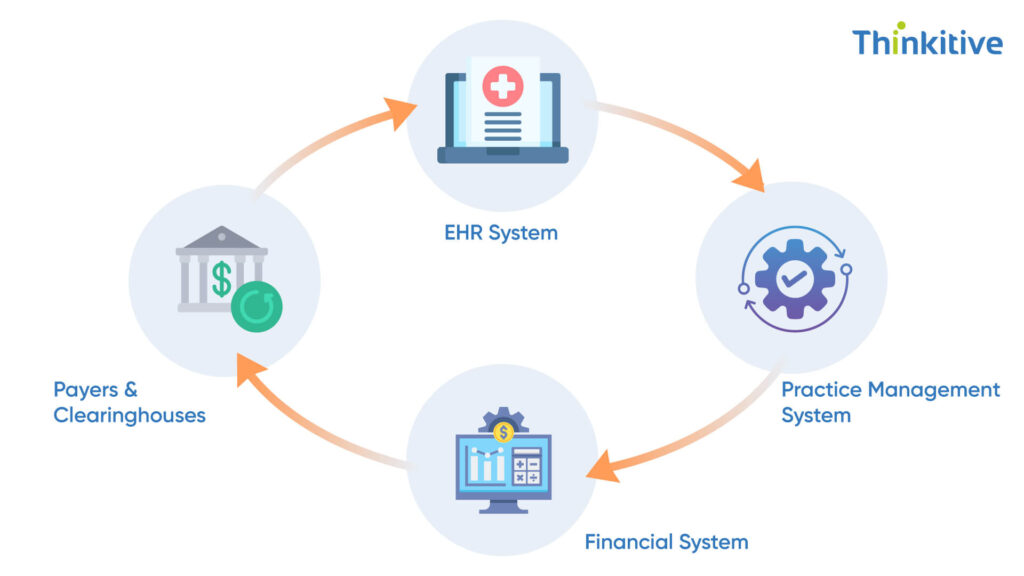
Data is the foundation of your billing practice. It can literally streamline your practice’s billing process and even set in motion the ideal workflow that suits your practice the best. That is why seamless integration of your EHR system, billing system, and AI RCM automation solutions is necessary.
Let’s see why it is necessary and why you should consider this:
1. EHR Integration Excellence: EHR is the epicenter of data for any healthcare practice, and it might be for your practice as well. Integrating your billing automation AI with an EHR system would enable bidirectional data flow. This is crucial to maintain seamless workflow continuity and bring everyone on the same page.
2. Practice Management System Connectivity: Another reason why you should integrate your AI RCM automation solution with a practice management system is because it enables real-time synchronization. Let me explain, you see, from scheduling to registration and care planning, everything is stored in your system. Now, integration with this system can enable real-time synchronization, further fast-tracking the billing process while ensuring accuracy.
3. Financial System Integration: With a 40 to 60-day period of reimbursement, getting an idea about your practice’s financial performance can be a little overwhelming. This is why connecting your AI RCM automation solution with accounting, banking, and financial reporting systems can provide you with comprehensive revenue visibility to plan things better.
4. Third-party Payer Integration: Integration with major insurance payers and clearing houses can be of extreme use as it enables real-time eligibility verification and gives you real-time updates on claim status.
Cost Recovery & Revenue Optimization: AI-Powered Financial Intelligence
Claim denials often lead to losses, which can negatively impact your practice’s financial performance. However, other than automation and speeding up your healthcare billing process, AI-powered financial intelligence can be utilized for cost recovery and optimizing your revenue as well. Let’s see how:
1. Revenue Leak Detection: When you have an AI instilled in your system, then use it effectively. For instance, with the revenue leak prevention AI module, the system can easily identify underpayments and missed charges and make contractual adjustments after reviewing.
2. Denial Pattern Analysis: Claim denials always have patterns, and it is usually seen in patients whose claims are often denied. In such cases, you can deploy machine learning algorithms to identify the root cause of denials and recommend preventive measures.
3. Contract Optimization: While you’re at it, use AI-powered analysis to analyze payer contracts so that you are reimbursed accurately.
4. Bad Debt Prevention: Bad debt is another indicator that can count your losses. Here, instilling a predictive model to identify collection risks can be of extreme use. Other than that, taking suggestions from it can also help you in implementing proactive intervention strategies.
Conclusion
If you’ve made it here, then I guess you must give an AI RCM automation solution a shot. You see, it can not only give you an opportunity to identify gaps in your billing process but also give you enough space to make improvements.
Along with that, the automation, speed, and accuracy it brings to the table, in this case system, is simply unmatched. On that note, let’s take a leap of faith and rely on advanced technologies to advance your practice. Click here to get started with the first process of system readiness and your requirements.
Frequently Asked Questions
AI RCM automation solutions significantly boost efficiency by streamlining processes. Billing automation with an AI claims submission agent and charge entry automation minimizes errors and speeds up submissions. An EOB GenAI parser accelerates payment posting. Furthermore, revenue leak prevention AI and RCM denial tracking proactively identify and resolve issues, leading to improved cash flow and reduced administrative burden.
AI RCM automation solutions significantly benefit stages like claims submission (using a claims submission agent), charge entry automation, and denial management. An EOB GenAI parser improves payment posting. AI also excels in RCM denial tracking and revenue leak prevention AI, proactively identifying and correcting issues to optimize billing automation.
AI RCM automation solutions significantly improve clean claim rates and reduce billing denials. AI-powered billing automation, like claims submission agents and charge entry automation, ensures accuracy. EOB GenAI parsers and revenue leak prevention AI further refine processes. RCM denial tracking leverages AI to identify trends and automate appeals, enhancing revenue and efficiency.
Implementing AI RCM automation solutions, like billing automation, claims submission agent, charge entry automation, EOB GenAI parser, revenue leak prevention AI, and RCM denial tracking, typically yields ROI within 6-18 months. Benefits include significant reductions in manual work, faster reimbursements, and decreased denial rates, leading to improved financial performance. Some organizations report results within the first quarter.
AI RCM automation solutions integrate with existing EHR and billing systems to streamline workflows. Key features include billing automation AI, a claims submission agent, and charge entry automation. An EOB GenAI parser interprets remittance data. This all works to enhance RCM denial tracking and enable revenue leak prevention AI, optimizing the entire revenue cycle.
AI RCM automation solutions significantly boost revenue recovery by addressing billing inefficiencies. Key capabilities include claims submission intelligence, charge entry automation, and EOB GenAI parser for swift processing. Revenue leak prevention AI and RCM denial tracking proactively identify and resolve issues, maximizing collections and minimizing lost revenue.
Key performance metrics for AI RCM success include:
- Clean Claim Rate: Measures the percentage of claims submitted without errors, indicating successful billing automation.
- Denial Rate & RCM denial tracking: Crucial for identifying and reducing claim rejections, highlighting the effectiveness of revenue leak prevention AI.
- Days in Accounts Receivable (A/R): Reflects the speed of payment collection, showcasing efficiency of AI RCM automation solutions and claims submission agent.
- Net Collection Rate: Percentage of collectible revenue actually collected.
- Charge Entry Accuracy/Automation Rate: Tracks precision and efficiency of charge entry automation.
- EOB GenAI parser accuracy: Measures how accurately the AI extracts and processes data from Explanation of Benefits, crucial for efficient payment posting.
GenAI EOB parsers significantly enhance payment posting accuracy by automating the extraction of key data, which is a core part of AI RCM automation solutions. This billing automation reduces manual errors common in traditional processes, improving charge entry automation and aiding the claims submission agent. The precision provided by the EOB GenAI parser is crucial for revenue leak prevention AI and effective RCM denial tracking.
AI-powered healthcare billing, using AI RCM automation solutions, must ensure HIPAA compliance and data security. Compliance is crucial for billing automation, claims submission agent, and charge entry automation. EOB GenAI parser, revenue leak prevention AI, and RCM denial tracking require robust controls to prevent fraud and maintain regulatory adherence.
Implementing AI RCM automation solutions, like billing automation and claims submission agent, can take as little as 40 days for core functions, but comprehensive deployment varies. Factors like integrating with existing systems, data quality for EOB GenAI parsers, and staff training for revenue leak prevention AI and RCM denial tracking influence the timeline, potentially extending it to several months.




