Client Requirements
The client was a prominent healthcare solutions provider in Texas, U.S. They had an extensive network of primary care providers, specialized care providers, and home care agencies.
The client desired a solution to improve communication between patients and providers. This would help enhance patient outcomes, decrease readmissions, and reduce service costs. These changes were made considering the effect chronic conditions have on patients, their families, and healthcare providers.
The client wanted to create an app for Chronic Care Management. This app should have telehealth capability and target people at high risk of hospitalization. This includes people with COPD, Asthma, hypertension, and other conditions such as diabetes.
Thinkitive Solution
Thinkitive's business analysts and subject matter experts initiated the requirement analysis phase. During this phase, the team worked on requirement gathering and competitive research. They suggested a solution that best fit the client's business needs.
The BA team takes a call with clients on multiple occasions while creating detailed functional requirement documents. After this, we designed low-fidelity prototypes and took timely approvals from the client.
Thinkitive assembled a team of experts in both frontend and backend development. The innovative team developed a microservices-based architecture and created separate microservices for each module.
Our team started from scratch while developing the chronic care management platform. This platform enables the providers to understand better patient needs and medication compliance, educate patients on specific diseases, and have faster, better patient-clinical communication.
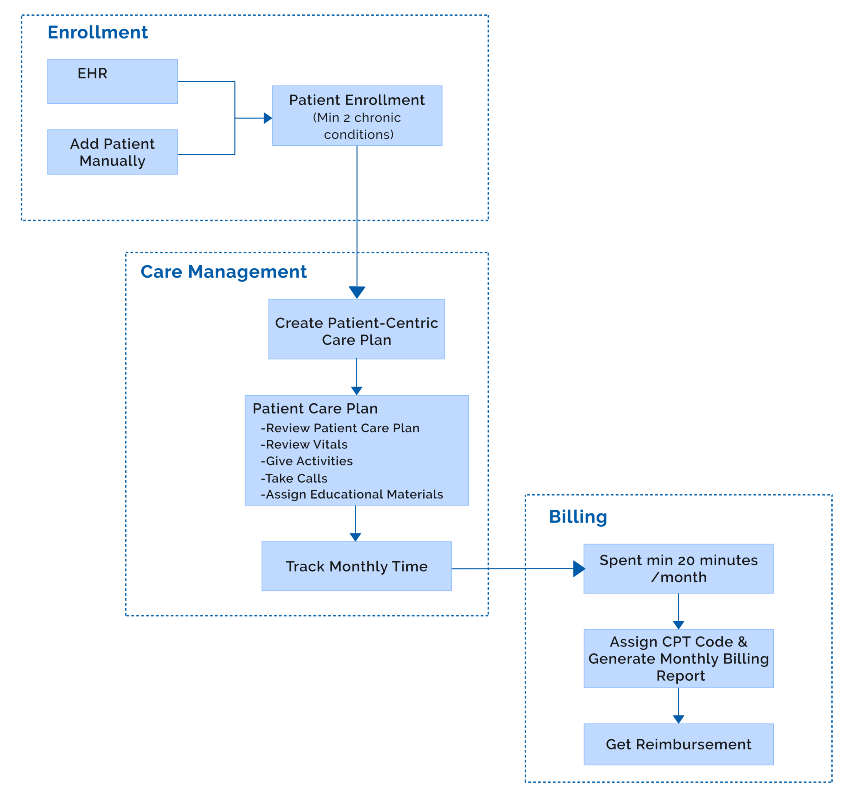
Solution Highlights
-
Patients Enrollment
Thinkitive has implemented a patient enrollment process. This process ensures eligibility for the CCM program, patient consent and documentation, and collection of patient clinical information. This can help providers to treat patients more effectively.
-
Care Management
Our team has developed a Care Plan module. This module enables providers to create a new patient-centric care plan. Alternatively, providers can create a care plan library for each disease.
Review Care Plan with Automated Time Tracking - Providers can review a patient's health information, care plan progress, and the goals outlined in the plan. They can assess the patient's progress based on this review. If necessary, they can also update the care plan. While reviewing the patient data, the system can record the provider's time spent on each patient.
Patient Screening and Assessment - The provider can do patient screening virtually. This includes conducting a health assessment, which may consist of questions and exercises for the patient to complete. From these screenings, the provider can mark the patient's health progress.
-
Track Time & Reimbursements
Time Tracking - During the non-face-to-face interaction by a provider with the Patient, the automated timer will run to record the time spent calling a patient, reviewing the care plan, and tracking progress.
CPT Code Assigning - Automated CPT code assigned based on time spent by the provider along with add-on code.
Report - CCM platform tracks and records everything from calls and interactions to bills and generates simple billing reports. Create a customized report based on CMS guidelines for guaranteed reimbursement.
Timely Reimbursement - Once the report is generated, the provider can review and download it from the CCM platform and send it to the payer.
Value Delivered
-
Quicker onboarding workflow.
-
Boost productivity so that the team can accomplish more in less time.
-
Workflow for documentation is significantly more streamlined and error-free.
-
A simple workflow can handle the entire episode of CCM.
-
Changes made by CMS can be implemented & configure easily.
