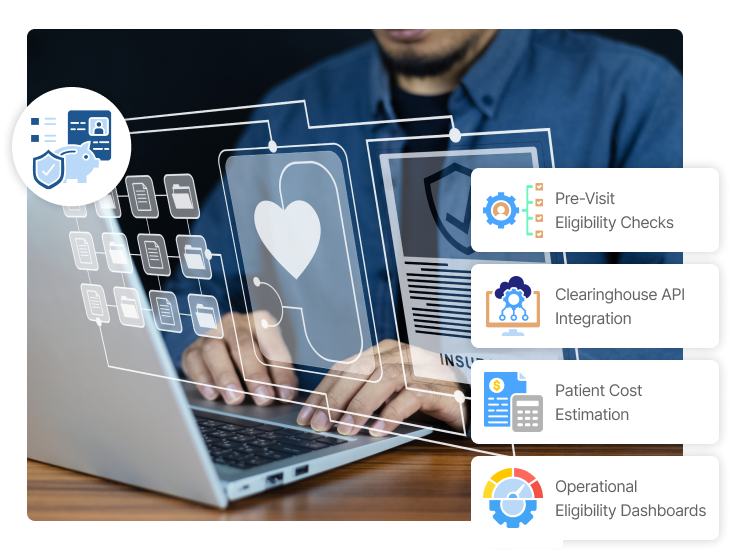
Real-Time Eligibility Verification to Eliminate Errors & Stop Revenue Loss
Embedded directly into your EHR, our AI verifies eligibility and benefits instantly, eliminating manual checks and stopping denial-related revenue loss at the source.
WHO IT’S FOR & WHAT IT SOLVES
Revenue Protection Starts at the Front Desk with AI-Powered Real-Time Verification
Eligibility verification mistakes, inactive coverage, and missed payer requirements quietly drive claim denials and revenue leakage across your front desk and revenue cycle.

Stop Revenue Leakage Before the Patient Is Seen
Discover how AI-powered insurance verification helps you stop denials and revenue loss.
CLIENTS TESTIMONIALS
Real Results in Eligibility Accuracy & Denial Reduction
Healthcare organizations are using automated eligibility verification to eliminate manual errors, prevent inactive coverage issues, and improve reimbursement accuracy before claims are submitted.
Cost & Timelines
Real-Time AI Insurance Verification On Time and Within Budget
We build real-time AI insurance verification solutions tailored to your timelines and cost expectations—without compromising compliance, data security, or accuracy.
Complexity
Software complexity (its functionality scope)
Type
Software type (e.g. web, mobile, desktop)
No. of Users
The expected number of users
Integrations
The required integrations as per regulations
Compliance
Regulatory compliance requirements
Security
Performance, security, usability and accessibility requirements
Deployment
The chosen deployment model (e.g. on-premise, cloud)
Sourcing
The sourcing model (in-house, outsourcing) & team composition
We deliver healthcare software in the following timeframes
1 Week
Medical software project starts within 1 week
2-4 Months
MVP release
Every 2-4 Weeks
New healthcare software versions

How Much Revenue Is Slipping Through Eligibility Gaps?
Automate real-time insurance verification to eliminate manual errors and reduce preventable claim denials.
Case studies
Read the Success Stories of Our Clients with Real-Time AI Insurance Verification
Empowering Healthcare Technology Innovation
250+
Healthcare Projects
400+
Healthcare Experts
98%
Client Retention Rate
150+
Healthcare Customers
50%
Cost Saving on Development

Engagement models
Affordable & Flexible: Engagement Models for Every Need
Our flexible engagement models allow us to customize our healthcare AI development services to meet your unique needs. Whether you're looking for a dedicated team, project-based work, or ongoing support, we have the right solution for you.
I have a requirement and want
to pay a fixed price
Share your project requirements, and our team will conduct a discovery call to understand your needs in detail. We'll provide a clear project estimate and deliver high-quality work. Pay only upon project completion and your satisfaction, ensuring you're never overcharged.
I want to hire a healthcare AI software developers
on an hourly basis
Hire dedicated developers with 160 hours of focused attention each month. Enjoy peace of mind with transparent billing, daily timesheets, and our unwavering commitment to your success. Benefit from the expert guidance of our complimentary Delivery Manager.
SAVE
EXTRA 20%
Specialties
Real-Time AI Insurance Verification Tailored to Your Specialty
We design and build real-time AI insurance verification for hospitals and healthcare practices based on your unique clinical workflows and operational needs.
Let’s Explore How We Can Develop AI Agents for Your Practice
Making your healthcare practice AI-ready with excellent custom healthcare AI solutions in just a Click!

Custom Real-Time AI Insurance Verification Development
Domain-specific Accelerators & Frameworks
End-to-End Healthcare Digital Transformation
Interoperable Data Systems
Assured Compliance & Security
Proficiency in Healthcare Standards
AI & Analytics Powered App Insights
Pre-Built Components
Accelerate Real-Time AI Insurance Verification Development with Healthcare-Ready Components
Use pre-built, compliant AI frameworks to shorten time-to-market and control development costs.
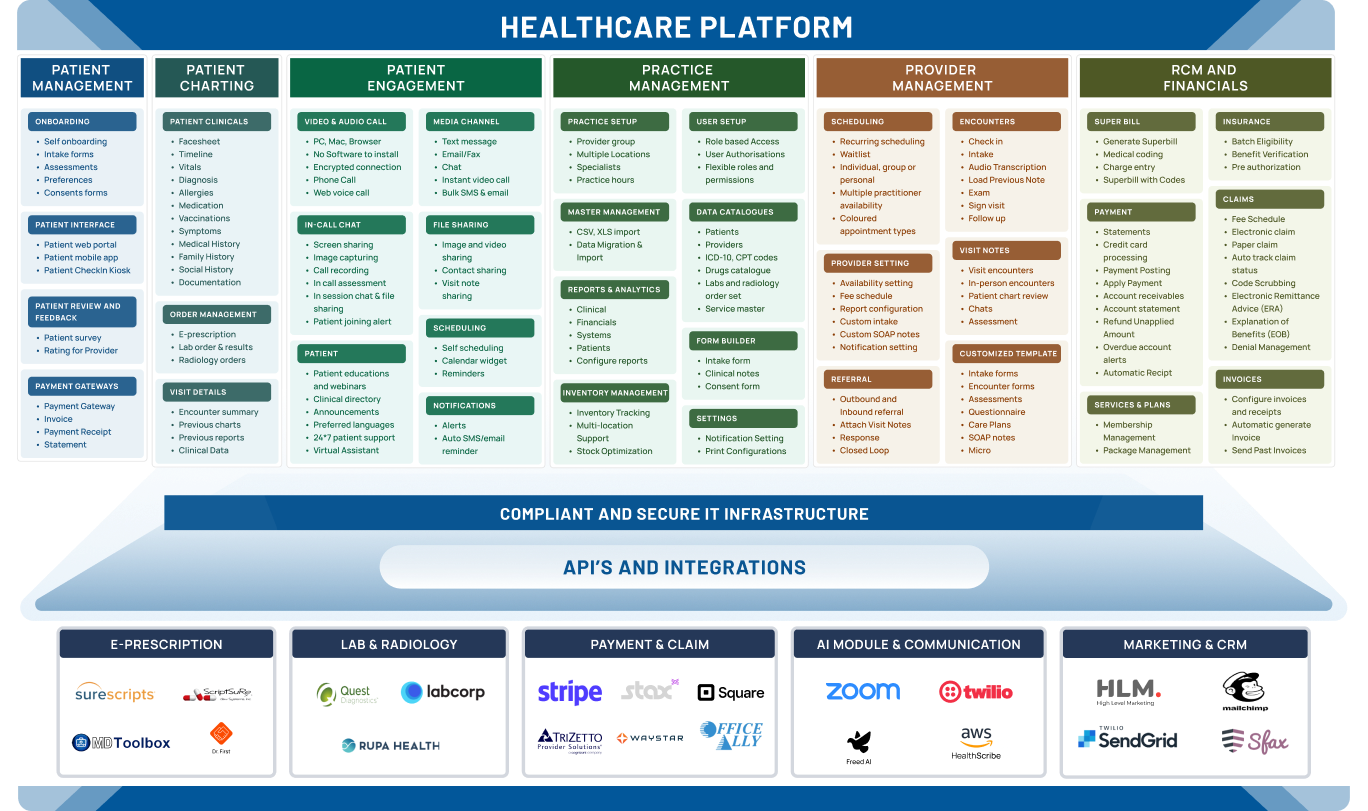
Integration
Make Your Practice Smarter and Quicker with Robust Integrations
Integrate your healthcare systems with ePrescribing, labs, billing, and patient engagement systems.
ePrescription & Labs Integration
We provide ePrescriptions and Labs integration with your AI ... agents to enable you to send orders directly from your healthcare system. These integrations offer multiple benefits, from minimizing errors to improving clinical efficiency and reducing the overall cost of care for both patients and providers.

Surescripts
Surescripts is the leading ePrescription network that helps improve medication ... safety and convenience for patients, providers, pharmacies, and safety and convenience for patients, providers, pharmacies, and payers. Integrate Surescripts into your AI healthcare solutions to enable secure electronic e-prescribing and real-time access to patient medication history.
Billing & Payment
Safe, secure, and seamless healthcare transactions with our billing, ... payment, and point-of-sale integrations for your AI agents. Give your virtual care practice a comprehensive real-life healthcare ecosystem.

Waystar
Waystar provides healthcare revenue cycle management solutions. Streamline claims processing, reduce denials, and optimize revenue capture through automation and AI, improving financial efficiency for healthcare organizations with Waystar.
Communication
Facilitate real-time communication with custom AI agents and ... stay connected with your patients at all times. Give your virtual care practice a comprehensive real-life healthcare ecosystem.

Sfax
Sfax is a secure faxing solution designed for healthcare. Integrating it with AI healthcare innovations enables secure exchange of patient information like faxes within the system, ensuring patient data privacy and compliance with HIPAA regulations. This streamlines communication and protects sensitive medical information.

Automate eligibility and benefit verification
Get real-time coverage checks and fewer billing surprises.








Framework & Technology Expertise
Our Healthcare Software Developer’s Framework & Technology Expertise
Our AI development team has broad experience in all AI technologies, frameworks, and expertise in multiple databases, real-time data processing, and cloud technologies.
Back-end Programming Languages
Front-end Programming Languages
Languages
Javascript Frameworks
Mobile
Cloud
Databases/Data Storages
SQL
NOSQL
Platforms

Need to Design, Develop, or Improve
Your Healthcare Software System?








Frequently Asked Questions
Get answers to all your questions
Still have questions ?
Everything About Healthcare Software Development
Healthcare AI Development Blogs

How AI Voice Scribes Can Slash Physician Burnout

Automating Medical Coding: How AI Improves Accuracy & Speed
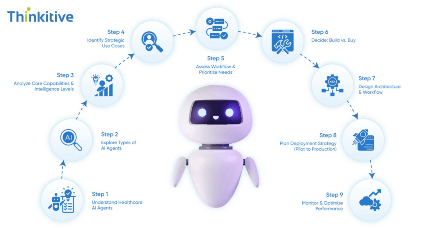
Step-by-Step Guide to Building Your First Healthcare AI Agent