Remote Patient Monitoring CMS Guidelines & Reimbursement

The Centers for Medicare & Medicaid Services (CMS) is part of the United States Department of Health and Human Services (HHS). It is responsible for administering Medicaid, Medicare, the Health Insurance Marketplace, and the Children’s Health Insurance Program (CHIP).
CMS has introduced Current Procedural Terminology (CPT) codes. This ensures providers can provide the correct services for the correct diagnosis. Moreover, these services are reimbursable for Medicare and Medicaid beneficiaries by submitting the correct claim, including the appropriate CPT codes.
CMS has recently implemented guidelines and reimbursement policies to support Remote Patient Monitoring (RPM). This has made RPM more accessible to both patients and healthcare providers.
Firstly as an RPM service provider, you must understand the CPT codes used for RPM services. Furthermore, you must be familiar with CMS guidelines for claiming these services. This will eventually help reduce denials and maximize reimbursement. This blog post will discuss the CMS guidelines and reimbursement policies for Remote Patient Monitoring in detail.
CMS Guidelines for Remote Patient Monitoring Software
The CMS has developed guidelines that healthcare providers must follow when using the RPM system to treat patients. These guidelines ensure the quality of care provided through RPM is high. They also ensure the technology used is safe and effective. Following are some of the CMS guidelines for RPM:
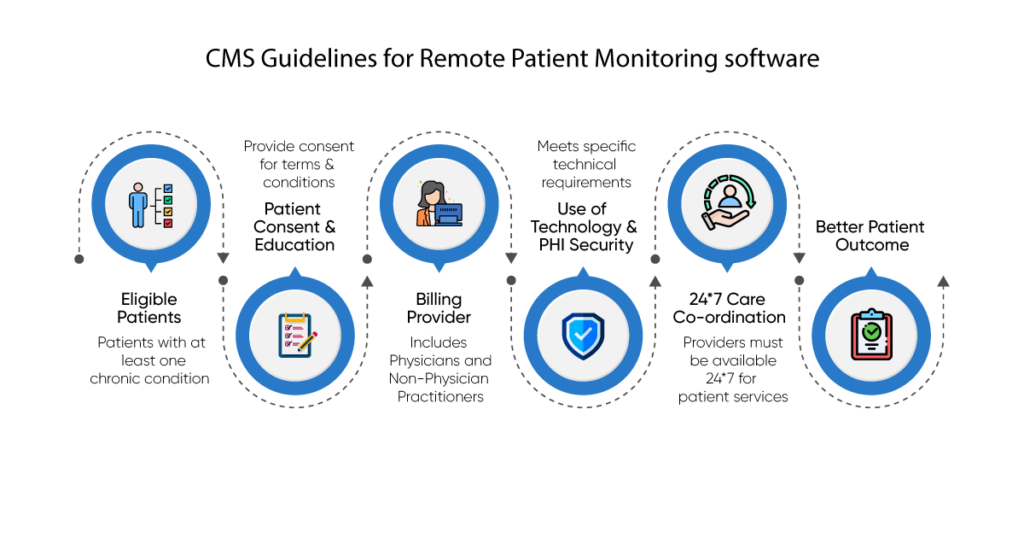
Eligible Patients:
Patients with at least one chronic condition over the past six months are at risk of serious harm to their health. In this situation, healthcare providers must identify these patients and determine their eligibility for remote patient monitoring (RPM). The following are examples of chronic conditions: Diabetes, Heart failure, and Chronic Obstructive Pulmonary Disease (COPD).
Patient Consent and Education:
Before providing Remote Patient Monitoring (RPM) services to a patient, they must understand how the system works. They must also provide consent for the following terms and conditions.
- Only one Provider can provide RPM services for a single patient for the same month
- Provider can share patient medical information with other providers for better care access
- Patients can stop RPM services at any point after completing the current month’s billing
- The patient must have to pay a co-pay if required
Billing Provider:
Qualified healthcare providers can bill RPM services. That includes both Physicians and Non-Physician Practitioners.
Below are some examples of RPM service providers other than Physician
- Certified Nurse Midwives
- Clinical Nurse Specialists
- Nurse Practitioners
- Physician Assistants
Use of Technology and PHI Security:
Healthcare providers must use remote monitoring technology that meets specific technical requirements. In addition, the data collected by the RPM system must be compatible and secure, complying with HIPAA rules.
24*7 Care Coordination:
Healthcare providers must coordinate care for patients. Moreover, providers must be available 24*7 for patient services. This also includes providing feedback and collaborating with other healthcare professionals. This is to ensure that the patient’s care is handled correctly.
Better Patient Outcome:
Firstly, healthcare providers must decide the right frequency for monitoring each patient. This must take into consideration their health condition and personal needs.
What are CPT Codes and Reimbursement For Remote Patient Monitoring?
Generally, CPT codes are a set of codes healthcare providers use to bill for patient services. With the introduction of remote patient monitoring, new CPT codes have been developed to allow providers to bill for RPM services. Furthermore, healthcare providers use these codes to report and bill for RPM services provided to patients.
CMS introduced the amendment in CPT codes in Dec 2021, and those updated codes will be effective from Jan 2022.
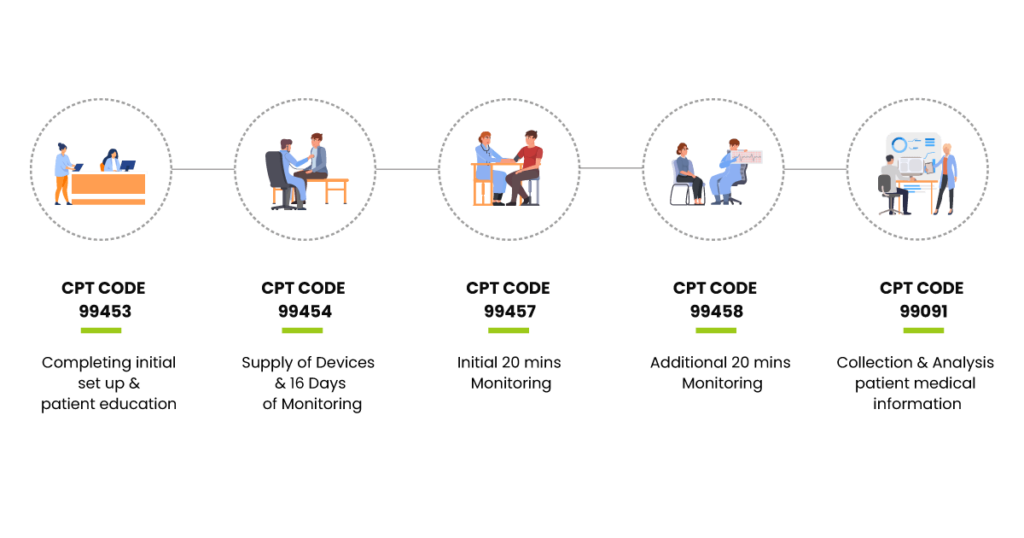
Below are the updated codes and their details:
1. CPT code 99453-Completing initial set-up and patient education
After successful enrollment, providers set up the care program and assign devices to patients. Providers can either rent out these devices or patients can also own such devices.
Providers educate patients about RPM services and device handling. This service can be billed under CPT code 99453. The most important thing to remember is that this code can be billable only once per episode.
The average reimbursement for CPT code 99453 is approximately $21 for each patient.
2. CPT code 99454-Supply of Devices and 16 Days of Monitoring
The Provider must supply the home health medical devices and a suitable care program to bill this service. The patient must have at least 16 days of readings over 30 days. Providers can bill this CPT code once within 30 days.
It cannot be repeated in the same 30-day period.
The average reimbursement for CPT code 99453 is approximately $50 Per month for each patient.
3. CPT code 99457-Initial 20 mins monitoring
The Provider must complete 20 minutes of monitoring to bill this CPT code. This includes checking the patient’s vitals, non-face-to-face consultation through messaging,audio-video calls, and providing other remote care.
Analyzing and interpreting patient physiologic data and vitals collection can be done remotely. Providers can bill this CPT code every 30 days.
The average reimbursement for CPT code 99453 is approximately $49 Per month for each patient.
4. CPT code 99458-Additional 20 mins monitoring
The Provider must spend an additional 20 minutes to the initial 20 minutes of remote monitoring to bill this code. CPT code 99457 can be billed multiple times per calendar month for each additional 20 minutes.
The average reimbursement for CPT code 99453 is approximately $38 Per month for each patient.
5. CPT code 99091-Collection and Analysis patient medical information
A qualified healthcare provider collects patient vital and other clinical information. They then analyze and interpret this data.
This service is typically used when patients discover abnormalities in their medical records
However, to qualify for this code, the Provider must spend a minimum of 30 minutes for each patient for each calendar month.
Complete Guide to RPM CPT Codes to Maximize Revenue
Free Guide DownloadHow Do RPM CPT Codes and Billing Work
Healthcare providers use CPT codes to bill for services rendered to patients. With the advent of remote patient monitoring, new CPT codes have been developed to allow providers to bill for RPM services. This blog post will discuss in detail how remote patient monitoring CPT codes and billing work.
How does billing for remote patient monitoring work?
Healthcare providers must meet specific requirements to bill for remote patient monitoring services. These requirements include:
- The patient must be an established patient of the Provider.
- The patient must have consented to receive remote patient monitoring services.
- The patient must be given an RPM device or use their own device.
- The Provider must be actively involved in the remote patient monitoring process and review and interpret the collected data.
- The Provider must document the services provided and the data collected.
Once the requirements are met, the Provider can bill for remote patient monitoring services using the appropriate CPT codes. The billing process involves submitting a claim to the patient’s insurance company, which includes the CPT code for the service provided and the amount charged.
It is essential for healthcare providers to properly document the remote patient monitoring services provided to ensure accurate billing. Providers should contact the patient’s insurance company. This is to confirm that the services are covered and to learn the reimbursement amount.
How to Optimize Revenue by RPM
Nowadays, it is easy to make money by providing Remote Patient Monitoring (RPM) services. It is keen to comply with Centers for Medicare and Medicaid Services (CMS) rules and guidelines. Doing so can help practitioners get maximum reimbursement for RPM services.
Providers can ensure their RPM services compliance with CMS in the following ways:
1. Choose the Appropriate RPM software
Choosing the right RPM software with the necessary features enables healthcare providers to comply with CMS guidelines. This provides comprehensive patient care.
User-friendly software with efficient communication features ensures better patient outcomes and makes reporting more straightforward. This helps to submit RPM reports and claims.
2. Choose the suitable RPM devices
Using the right medical devices to track patient physiologic data is vital in remote patient monitoring services.
Devices must ensure that patients have a smoother experience of handling medical devices and can also be able to transmit physiologic data seamlessly.
FDA-approved devices are clinically tested, increasing trust and reducing the amount of rejected claims.
3. Target right patient
Patients with six months or more of chronic illnesses may be eligible for Remote Patient Monitoring (RPM) services. This illness has had a significant impact on their health.
Those patients may have diabetes, asthma, blood pressure, hypertension, obesity, and other diseases.
4. Outsourced the task if required
Remote care providers can outsource tasks.
They form a care team for each patient. This team provides remote care to the patient. The team can work under the guidance of QHP.
This team can complete a range of tasks. These include the following:
– Documenting patient data.
– Obtaining patient consent.
– Setting up and onboarding patients and staff on a remote health monitoring system.
– Supplying RPM devices to patients.
Conclusion
In conclusion, the Centers for Medicare & Medicaid Services (CMS) has played a pivotal role in making Remote Patient Monitoring (RPM) more accessible and financially viable for healthcare providers. Their introduction of specific CPT codes and comprehensive guidelines has paved the way for RPM to enhance patient care while ensuring fair reimbursement. By adhering to these guidelines, healthcare providers can not only optimize revenue, and deliver better patient outcomes but also contribute to the future of remote healthcare. When executed with precision and compliance, RPM services offer a win-win solution for both patients and healthcare providers in the ever-evolving landscape of modern medicine.




