AI-Powered EHR Software: A Roadmap for Clinics
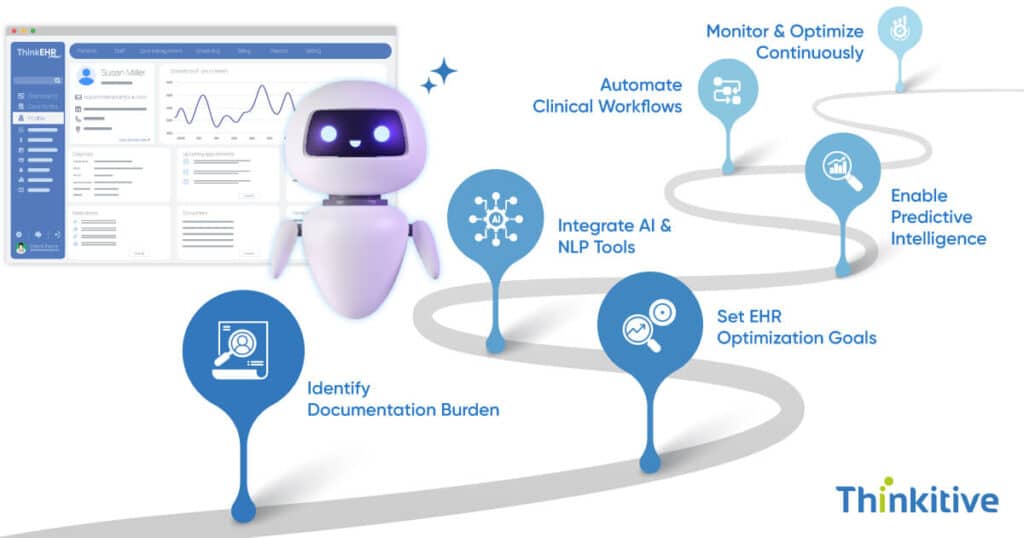
The EHR systems today have become the epicenter of any healthcare practice. Every information you need to deliver care can be found in your EHR. While it has revolutionized the healthcare industry, it has also brought some of the problems of its own.
For instance, the introduction of EHR systems has made documentation much easier, but also necessary. Due to this, healthcare providers have been spending most of their time filling out EHRs. In fact, if you’re a healthcare provider, then you must be familiar with the ‘Pyjama Time,’ right?
The time you spend out of your practice, filling up EHRs, is called Pyjama Time. And over the past few years, that has become a growing concern for everyone. So, what can be done?
Well, the answer to this lies in the very thing we use to solve our earlier problems – Technology.
Now, the introduction of advanced technologies like AI, machine learning, NLP, etc., has been evolutionary for many industries. Furthermore, its introduction of AI-powered EHR software in the healthcare industry is somewhere highly anticipated.
So, why not power your EHR system with an AI EHR solution? How does it change your practice, or what change will it bring?
Well, let’s uncover that in this blog today and also try to find a roadmap for AI-powered EHR software development.
So, without further ado, let’s get started!
Understanding AI-Powered EHR Software: Beyond Traditional Systems
The problem with traditional EHR systems is that they are largely reactive and static in nature. Although efficient at storing patient data, they lack the ability to analyze the data they collect and store or make sense of it. This is where AI-powered EHR software can be used to enhance patient care practices.
These intelligent EHR systems leverage technologies like machine learning, natural language processing (NLP), and predictive analytics to proactively assist healthcare providers in decision-making. Additionally, manual work is also reduced as you can use smart EHR platform features to interact with systems that understand context, suggest diagnoses, and even draft clinical notes.
Moreover, NLP-powered documentation makes note-taking efficient and stress-free as you can convert voice or free-text inputs into structured notes in real-time. And when you combine this with predictive analytics, you get an intelligent healthcare system that uses real-time data trends to identify high-risk patients and suggest the best possible treatment pathway.
Patient health management and care coordination also benefit from AI-powered EHRs. They analyze vast patient datasets, identifying trends, forecasting outbreaks, and optimizing resource allocation. Along with all of this, the EHR system’s adaptive nature sets this apart from traditional EHRs.
In short, this evolution not only promises to reduce administrative burden but also elevates care quality and precision across the board.
Strategic Use Cases: Where AI-Powered EHR Software Transforms Clinical Practice
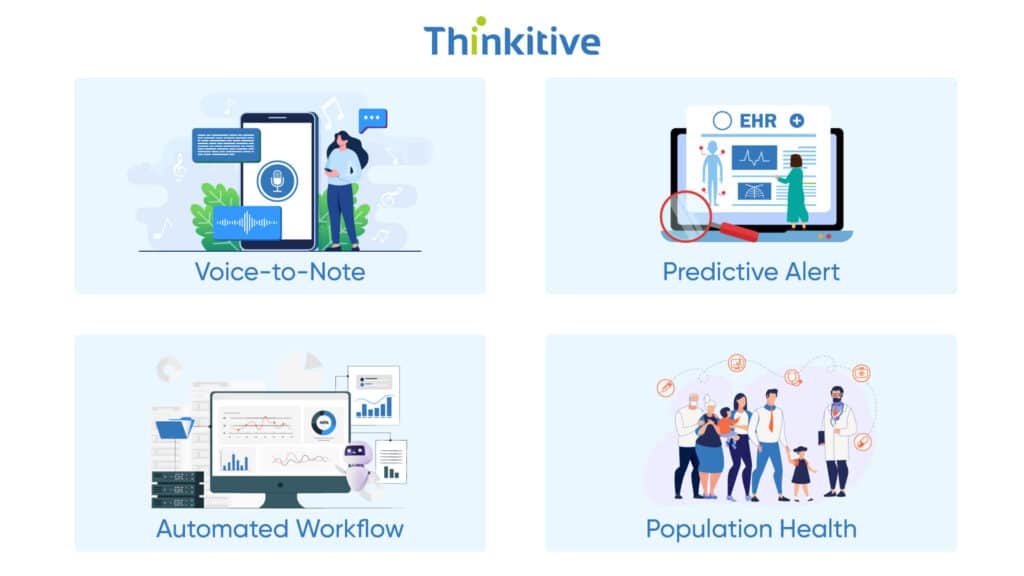
When you shift to AI-powered EHR software, you don’t just upgrade a single system; you entirely change how your clinical workflows and decision-making work. The first thing that changes is the way to take notes, shifting from a traditional, time-consuming way to a more efficient AI-powered way. AI-powered voice recognition tools turn patient-provider conversations into structured notes in real-time. Additionally, all this happens while maintaining the accuracy of the data and not damaging its context.
The next change is that you get predictive clinical insights with intelligent EHR systems. You are able to identify hidden patterns that a human eye misses with AI models that analyze historical and real-time data. This makes early intervention possible, boosting patient safety and improving outcomes.
But benefits don’t stop here, as automated workflow management powered by AI makes sure that the right tasks reach the right people at the right time. These clinical AI workflows can drastically reduce delays and friction in care delivery by managing everything smoothly.
The population health intelligence tools help you identify public health trends, manage the chronic disease population, and shape care protocols. The result of all this is a streamlined, smarter clinical practice that allows providers to focus on patients and not be entangled in systems.
Clinical AI-Powered EHR Use Case Library to Better Understand the Benefits
DownloadPlatform Selection: Leading AI-Powered EHR Software Solutions
Making the right choice for your AI-powered EHR software is important, and it can make or break your clinic’s digital transformation journey. You have multiple options open to you from enterprise-grade systems like Epic and Cerner Oracle, to agile cloud-native platforms like Athenahealth and NextGen.
This wide range can be confusing, so here is a simple table that gives you a comparison between these systems in an easy way:
| Platform | AI Capabilities | Cloud-Native | Specialty Support | AI Maturity Level | Notes |
| Epic | NLP, predictive analytics, ML-based CDS | Partial | Broad | Advanced | Strong enterprise adoption |
| Cerner Oracle | AI-driven diagnostics, pop health AI | Yes | General | Intermediate | Strong in hospital networks |
| Athenahealth | Smart scheduling, clinical note AI | Yes | Moderate | Growing | Agile for midsize practices |
| NextGen | Risk scoring, AI alerts, cloud-based | Yes | Yes | Moderate | Ideal for outpatient and specialty care |
| Elation/Canvas/Other AI-Native | Built-in AI from the ground up | Yes | High | Emerging | AI-native, great for nimble practices |
While Epic AI features and Cerner Oracle AI EHR solutions are the first choice in enterprise-grade intelligence, Athenahealth AI and NextGen are more popular in agile, cloud-based platforms. Whereas AI-native EHR platforms built from the ground up for machine learning offer promising flexibility but require careful vetting due to varying levels of maturity.
Data Intelligence & Clinical AI: Maximizing EHR Software Capabilities
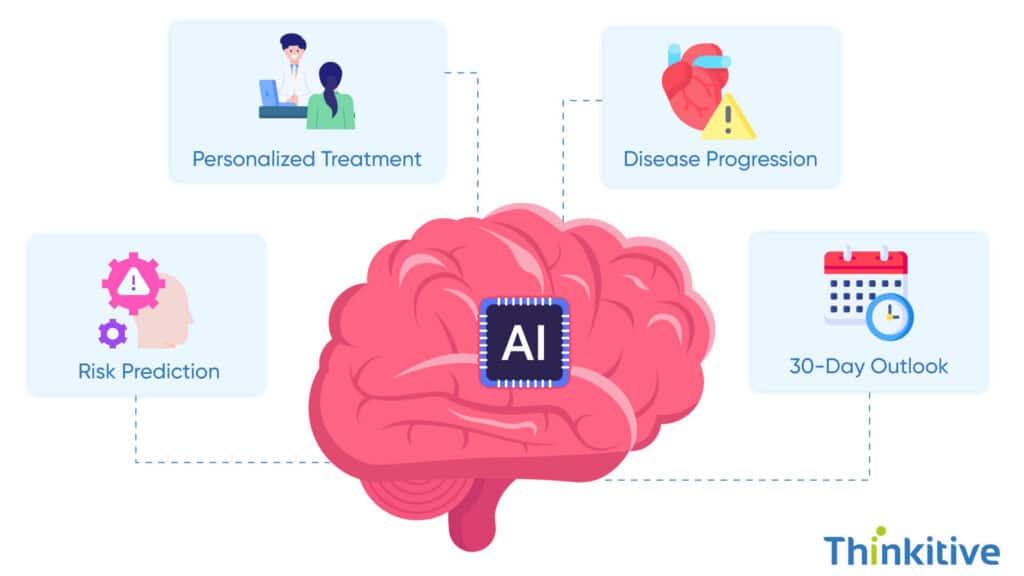
You must have noticed how the EHRs are overflowing with data; however, using that to make medical decisions is quite difficult. This is where clinical AI analytics shows its importance, by turning the raw data into actionable insights in real-time.
With smart EHR data intelligence platforms, you can go beyond charting and record-keeping. Every lab result, diagnosis code, and clinical note becomes a clue to diagnosing the patient’s condition with increased accuracy.
Take predictive modeling, for example, with its AI-powered algorithms, it can predict patient health deterioration, flag readmission risks, and personalize care plans. For instance, you can know which diabetic patient will experience complications based on their lifestyle or past reports before they show any symptoms.
Natural Language Processing (NLP) changes the whole game of note-taking. With this tool at your bay, you can easily convert voice-recorded insights into structured documents automatically. Real-time decision support is also a powerful benefit. With this, you can process and analyze the health data as it is generated, improving decision quality and speed.
You get intelligent recommendations based on patient records and health patterns, and not just alerts. This helps providers make faster, more informed decisions without facing information overload. In short, what seemed futuristic is now foundational support for patient care.
Implementing Strategy & Testing: Deploying AI-Powered EHR Software
When it comes to rolling out the AI-powered EHR software, you need to be careful and adopt a phased approach to ensure it goes smoothly. This is where a phased implementation strategy can be useful for deploying AI features department by department and not all at once, with diagnostic and decision-support tools.
After that comes AI model training and validation, because clinical AI is only as good as the data it is trained on. But you need to use de-identified data to keep patient data privacy, and also remember to use specialty-specific datasets to align the algorithms with your patient population. Running a validation test after this is necessary, as you need to confirm it has been trained as you intended.
Next comes workflow integration testing. Test how AI tools will behave in real-world scenarios, and check if the NLP tool understands clinical terms clearly. Additionally, make sure that predictive alerts show at the right time. These tests ensure the tech works fine and will not stop functioning at a critical point in care.
Finally, managing the adoption process and the changes these new systems will bring efficiently, especially for your workforce, is essential. Tell them the why behind the change and provide training while creating feedback loops to improve stability.
Interoperability & Standards: Connecting AI-Powered EHR Software
No matter how capable your AI healthcare software and AI EHR solution are, it needs to be well-connected to perform at its full potential. That’s where healthcare interoperability AI steps in, and in the era where healthcare moves fast, this is a must-have, not just a nice-to-have.
Moreover, you need to follow healthcare standards like FHIR R4 and Smart-on-FHIR AI to enable intelligent EHR systems to talk to one another and devices. Here’s a quick breakdown of how today’s interoperability standards power AI-enhanced EHR connectivity:
| Standard / Tool | Purpose | AI Relevance |
|---|---|---|
| FHIR R4 | Structured data sharing via RESTful APIs | Enables real-time data feeds for AI models |
| Smart-on-FHIR | App framework built on FHIR for plug-and-play tools | Embeds AI apps into EHR workflows |
| API Integration | Custom system/device connectivity | Links EHRs with AI devices, wearables, etc. |
| Future Standards | ONC TEFCA, HL7 AI models (in development) | Ensures long-term compatibility and upgrades |
What makes AI EHR connectivity truly transformative is context-aware interoperability; it not only transfers data, but it also understands it.
Conclusion
In a nutshell, Electronic Health Records AI is completely revolutionizing EHR systems. AI EHR solutions, along with AI medical records software, are changing workflows, especially medical documentation, from the ground up.
So, if you are interested in transforming your healthcare and making EHR systems proactive rather than reactive, using Artificial Intelligence EHR is the best option. Click here to start your journey towards faster and smarter healthcare with AI EHR solutions and systems.
Frequently Asked Questions
AI-powered EHR software supports smarter and more proactive decision-making than traditional EHRs with advanced technologies like AI and machine learning. It enhances traditional systems by automating tasks, enhancing analytical abilities, reducing manual work, and enabling intelligent alerts, which improve patient outcomes and provide personalized care recommendations.
Implementing AI-powered EHR software typically costs between $50,000 $250,00 or more. The final price depends on customization, data migration, integration complexity, and vendor support. Moreover, sometimes there are additional costs associated with training, maintenance, and compliance upgrades. If you use cloud-based models, it may reduce upfront costs but may add subscription fees.
Implementing AI-powered EHR software typically takes 6 to 12 months, depending on the system’s complexity, customization needs, data migration requirements, and staff training. Smaller practices may move faster, while larger healthcare networks often require phased rollouts and rigorous compliance testing before full deployment.
When you are selecting EHR software, first prioritize AI features like predictive analytics for patient risk scoring, NLP for documentation, and intelligent alerts and AI-powered decision support. Also, look for AI-driven workflow automation and real-time interoperability tools to enhance provider efficiency and patient outcomes.
To keep data secure and follow HIPAA rules in AI-powered electronic health record (EHR) software, use strong encryption, limit access, conduct regular checks, and employ AI to spot unusual activity. Make sure all AI models that handle personal health information (PHI) are trained and used in secure settings that comply with HIPAA’s Privacy and Security guidelines.
Staff needs practical training on using AI features, understanding predictive insights, and keeping data accurate. Ongoing technical support should be available, along with tutorials for specific roles and guidance for managing changes. This will help ensure the smooth adoption of AI-powered EHR systems and build trust among clinical and administrative teams.
Yes, AI-powered electronic health record (EHR) software can work with current healthcare systems and devices. It does this by using common standards like FHIR and HL7. Through application programming interfaces (APIs) and smart connections, it connects easily with labs, imaging systems, and wearables. This allows for smooth data sharing, better workflows, and improved clinical decision-making, all without needing to change the existing infrastructure.
AI-powered electronic health record (EHR) software can provide significant returns on investment (ROI). It does this by reducing administrative costs, speeding up clinical decision-making, improving patient outcomes, and decreasing billing errors. Clinics often see returns of 3 to 5 times their investment over time due to better efficiency, smarter use of resources, and improved revenue management, thanks to automation.
When choosing AI-powered EHR vendors, focus on a few key areas. First, check if the vendors support interoperability standards like FHIR and Smart-on-FHIR. Next, look at their AI features, such as predictive analytics and automation. Make sure they comply with regulations like HIPAA and HITECH, and see what customization options they offer. User experience and how easily you can integrate the system are also important. Also, review the chosen vendor carefully to make sure that they will deliver compliant and scalable software that will improve your ROI.
AI-powered electronic health record (EHR) software must follow privacy laws like HIPAA, HITECH, and GDPR. It also needs to address specific risks related to AI, such as algorithm bias and the need for clear explanations of its decisions. If the AI affects clinical choices, it may come under FDA oversight. It is essential to ensure that data handling is secure and that all processes can be audited for regulatory compliance.



