Prior Authorization Failures in Mental Health: The Missing Workflow Problem
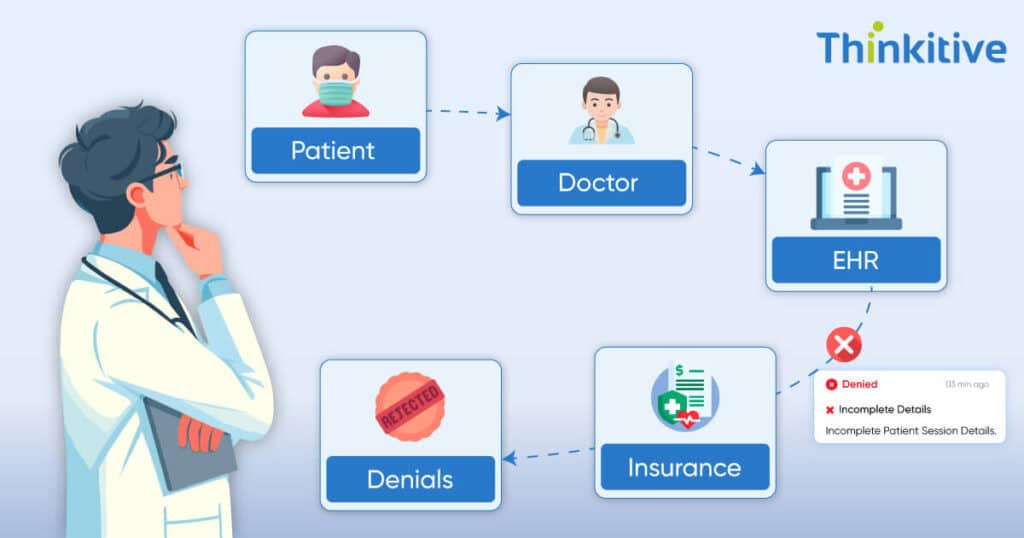
Navigating mental health care is never easy, but prior authorization (PA) makes it even more complicated. While it’s a necessity, even an essential step for ensuring that patients get the right treatment, and it is medically needed, for providers, it’s an added administrative load.
Almost all of the insurance companies demand approvals for every treatment, from therapies to psychiatric evaluations. These approvals not only bring extra paperwork but also delay patient care, and most importantly, lead to clinician burnout.
Furthermore, this already lengthy and tiring process is made even more complicated by the generic EHRs. These systems are tailored for the PA in physical health and not designed for the mental health prior authorization process.
Without these streamlined workflows, most of the work needs to be done manually, leading to repetitive administrative work or increased risk of claim denials. That’s why, in behavioral health, prior authorization automation and smart EHR integration, backed by professional behavioral health EHR implementation services, are essential tools for reducing delays and errors.
So, in this blog, we will focus on decoding why mental health prior authorization requests get denied and how to streamline prior authorization in behavioral health with custom mental health EHR solutions.
Let’s get started without further ado!
Understanding Prior Authorization in Behavioral Health
Now, prior authorization is a requirement set by providers to get approval for certain mental health services. This includes therapy sessions, psychiatric evaluations, and medication management before the treatment is started.
Although this is intended to ensure that the patient receives appropriate care, it adds extra work for clinicians. Moreover, being a long process, it can delay treatment and frustrate both patients and providers.
Insurers require prior authorization for several reasons. One of those reasons is fraud prevention, ensuring services are medically necessary and billed correctly. Another reason is that cost control helps manage healthcare spending, while confirming medical necessity guarantees the treatment aligns with the patient’s clinical needs.
The prior authorization process involves three steps. First is submission, where the clinician or staff sends a request. The second is a review in which the insurer evaluates medical documentation and compliance. The final step is approval or denial, which determines whether care can proceed.
Behavioral health often faces unique bottlenecks compared to other specialties. Therapy authorizations may require detailed clinical notes, while medication management can demand lab results or psychiatric documentation. Generic EHRs frequently lack integrated PA workflows, forcing staff to track approvals manually, increasing the risk of delayed care, rejected claims, and clinician burnout.
Streamlining these steps with behavioral health EHR workflow improvements and prior authorization automation can save time, reduce insurance approval delays in mental health, and enhance patient outcomes. For providers navigating the growing PA burden, leveraging technology is no longer optional; it’s essential.
The Missing Workflow Problem

Despite their central role in patient care, most EHRs fall short when it comes to mental health prior authorization workflows. Generic systems often lack built-in, specialty-specific processes, leaving clinicians and administrative staff to handle approvals manually.
Manual workflows are time-consuming and error-prone. Teams rely on faxing forms, making repeated phone calls, and uploading documents, often across multiple platforms. Without centralized tracking, it’s easy for requests to slip through the cracks, leading to delayed care and denied claims.
Poor visibility is another major issue. Many EHRs do not provide real-time dashboards for pending authorizations, making it difficult to know which requests are waiting for review, which are approaching expiration, or which have been denied. This lack of oversight not only frustrates staff but can directly impact revenue.
Consider a mid-sized behavioral health clinic that handles dozens of therapy authorizations weekly. Without automated tracking, renewal requests are missed, approvals expire, and reimbursement is delayed. Over time, these gaps accumulate into significant financial losses and increased clinician burnout.
Addressing this missing workflow and common prior authorization challenges for behavioral health providers is critical. By implementing prior authorization automation and integrating PA-specific processes into behavioral health EHR workflows, clinics can gain real-time visibility, reduce insurance approval delays in mental health, and reclaim both time and revenue.
How Workflow Automation Solves Prior Authorization Failures
Behavioral health clinics can overcome prior authorization challenges by implementing workflow automation within their EHR. Key benefits include:
1. Centralized Dashboards
- View all pending, approved, and denied PA requests in one place.
- Automated submission and tracking ensure no request is overlooked.
2. Real-Time Alerts
- Notifications for expiring approvals or incomplete documentation.
- Enables timely follow-ups, reducing the risk of claim denials.
3. Integration with Payer Portals
- Connect directly via APIs or portal integrations.
- Requests and updates are automatically synced with the EHR, minimizing manual effort.
4. Reduced Staff Time and Errors
- Automation frees clinicians and administrative teams from repetitive tasks.
- Results in faster insurance approvals, fewer mistakes, and improved patient care.
By combining these features, behavioral health providers can streamline prior authorization workflows, reduce insurance approval delays in mental health, and reclaim both time and revenue. Automation transforms prior authorization from a bottleneck into a smooth, predictable process.
Building an Effective Prior Authorization Workflow in Your EHR
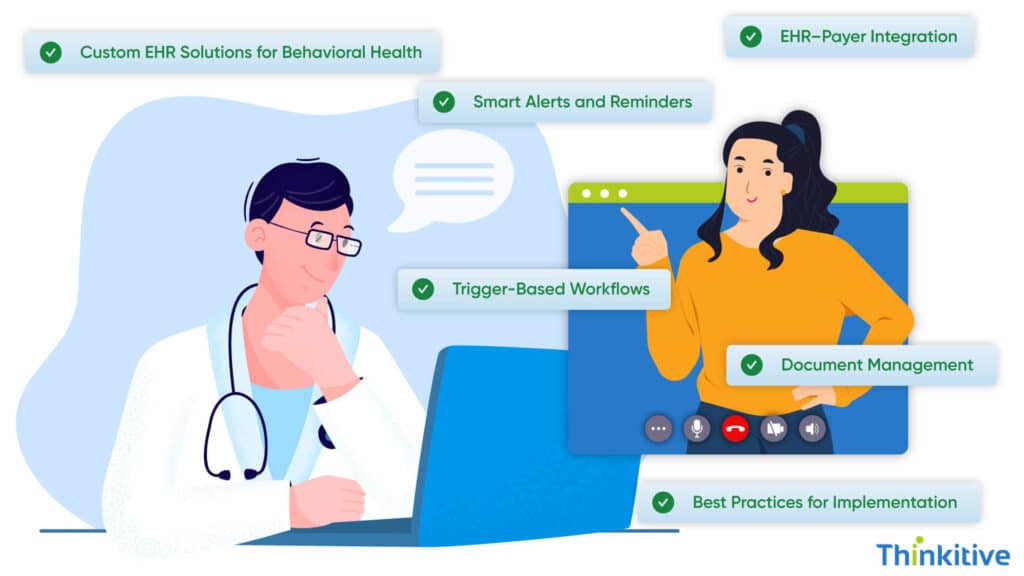
When it comes to automating prior authorization workflow in EHR, it needs some key features to reduce delays, denials, and staff burnout. Here’s what to prioritize:
1. Trigger-Based Workflows
Automatically initiate PA requests when a new treatment plan, therapy session, or medication is added. This ensures no request is missed and minimizes manual tracking.
2. Document Management
Auto-attach clinical notes, lab results, and supporting documentation to each PA request. Complete submissions increase approval rates and speed up insurer review.
3. Smart Alerts and Reminders
Receive notifications for expiring approvals, incomplete documentation, or pending submissions. Timely alerts help prevent claim denials and reduce administrative stress.
4. EHR–Payer Integration
Connect directly with insurance portals or APIs. Requests are submitted and updated in real-time, giving staff full visibility into authorization status without extra phone calls or faxes.
5. Custom EHR Solutions for Behavioral Health
Tailored workflows built for therapy, psychiatry, and medication management reduce errors and save time. Automation ensures faster insurance approvals and improved patient care.
6. Best Practices for Implementation
Map existing PA processes before automation, train staff on new dashboards and workflows, and regularly audit results. Continuous optimization ensures compliance, efficiency, and revenue protection.
By integrating these components, behavioral health providers can transform prior authorization from a bottleneck into a streamlined, predictable process. Automated EHR workflows for prior authorization reduce insurance approval delays in mental health while improving operational efficiency and clinician satisfaction.
Financial Impact: Lost Revenue & Delayed Reimbursements
Prior authorization challenges don’t just affect patient care; they hit the bottom line. Delayed or missed approvals can lead to denied claims, slower reimbursements, and lost revenue. For behavioral health clinics, even a few missed authorizations per week can accumulate into significant financial losses.
One mid-sized behavioral health clinic tracked PAs manually across multiple systems. A series of missed renewals and expired approvals resulted in $25,000 in lost revenue over just a few months. The administrative burden also increased staff stress and clinician burnout, highlighting how inefficient PA workflows have real-world costs.
Integrating prior authorization automation into a behavioral health EHR can dramatically reduce these financial risks and improve mental health claims management. Automated submission, smart alerts, and EHR–payer integration cut down on human error and speed up approval timelines. Clinics report fewer denials, faster reimbursement cycles, and measurable ROI, often recouping their technology investment within months.
By streamlining PA workflows, behavioral health providers not only improve care delivery but also safeguard revenue and operational efficiency. In today’s insurance environment, workflow automation in behavioral health EHRs isn’t just a convenience; it’s a critical business strategy that turns a costly bottleneck into a predictable, revenue-positive process.
The Future: AI & Predictive Authorization Workflows

The future of mental health prior authorization lies in AI-driven, predictive workflows that anticipate authorization needs before submission. By analyzing historical claims, treatment patterns, and payer behavior, AI can identify which cases are likely to require PA, allowing clinics to act proactively rather than reactively.
Advanced EHRs use AI to automatically populate PA forms with the right clinical notes, diagnosis codes, and supporting documentation. This reduces manual entry, accelerates submission, and lowers the risk of errors that lead to denials.
Modern behavioral health EHR vendors are evolving to support predictive PA workflows, integrating AI with dashboards, smart alerts, and payer portal connections. These systems notify staff of upcoming approvals, automatically update requests, and even suggest the optimal documentation for faster insurer review.
By leveraging AI and predictive analytics, clinics can reduce insurance approval delays in mental health, improve reimbursement timelines, and minimize staff burnout. Predictive PA workflows are not just about efficiency; they enable a more strategic approach to care management, ensuring patients receive timely treatment while clinics protect both revenue and operational efficiency.
As behavioral health providers embrace these innovations, workflow automation combined with AI will transform prior authorization from a reactive administrative burden into a proactive, intelligent process, positioning clinics for a more efficient, revenue-secure future.
Conclusion
Prior authorization challenges in behavioral health are more than administrative hurdles; they impact patient care, staff efficiency, and clinic revenue. From missed approvals to delayed reimbursements, the workflow problem is at the heart of these inefficiencies. Implementing automated, specialty-specific EHR workflows with real-time tracking, smart alerts, and payer integration can transform prior authorization into a smooth, predictable process.
For clinics ready to reclaim time, reduce denials, and improve reimbursement cycles, Thinkitive’s Behavioral Health EHR offers a streamlined solution that handles prior authorizations efficiently, empowering your team to focus on what matters most: delivering quality care.
Ready to see how Thinkitive’s Behavioral Health EHR streamlines prior authorization for your team? Book a demo right away.
Frequently Asked Questions
Denials often occur due to incomplete clinical documentation, missing treatment plan details, incorrect CPT or diagnosis codes, expired authorizations, or submission to the wrong payer. Lack of timely follow-ups and manual tracking errors also contribute to rejected mental health claims.
EHR automation ensures complete, accurate, and timely PA submissions by auto-populating forms, attaching clinical notes, and sending smart alerts. Real-time tracking reduces missed deadlines and errors, increasing approval rates while minimizing staff workload and improving overall revenue cycle efficiency.
Yes, modern behavioral health EHRs allow payer-specific workflow configurations, including custom templates, required documentation, and submission rules. This ensures each insurer’s criteria are met, reducing denials and streamlining approvals across multiple payers without extra manual effort.
Implementation timelines vary by clinic size and EHR complexity. Smaller practices may deploy basic workflows in a few weeks, while larger organizations integrating multiple payer systems may take 8–12 weeks. Proper mapping, staff training, and testing ensure smooth adoption.
Key metrics include PA approval rates, denial frequency, average submission-to-approval time, staff time spent on authorizations, and revenue recovered. Tracking these KPIs helps identify bottlenecks, optimize workflows, and demonstrate the ROI of prior authorization automation in behavioral health.



