A Deep Dive into Custom EHR Software Architecture, Compliance & Scalability

There is a shift in the healthcare industry that is forcing providers to move from off-the-shelf software systems to custom software systems. This shift has been brought into the healthcare ecosystems due to the inefficiencies of the generic software systems.
You see, every healthcare practice has unique workflows and administrative and clinical needs. And most of the time, healthcare providers struggle with aligning these software systems with their practice. However, with very limited room for customization and scaling, they are forced to align their practice with the requirements of the software.
This disrupts their entire practice’s workflow, and many healthcare providers are shifting to custom solutions, specifically with the EHR software systems. And in their quest to align their software systems with that of the practice, many providers have chosen custom EHR software development approaches.
However, when interacting with some of the providers in recent times, I have realized that most of these custom EHR software development ventures fail because of poor or incapable architecture. And these providers are not to be blamed, given their limited understanding of a custom software architecture.
But when you develop a custom EHR software, it is important to understand the custom EHR software architecture. Since it is a high-level structure that acts as a blueprint that defines the core components, their relationships, and how they interact with each other, it defines the performance of the software and also helps in scalability and maintenance.
That is why, since we entered this space of custom EHR software development, we have focused on having a robust architecture that can be easily adaptable.
On that note, let this blog be your guide to custom, secure, and compliant EHR architecture while building your own EHR. In this blog, we will discuss the intricacies of custom EHR system architecture and everything that you need to know.
So, without further ado, let’s get started!
Assess Your System Architecture Readiness for Custom EHR
Get Free ConsultationFoundation of Custom EHR Software Architecture
To understand the architecture of any software, you need to understand the foundation of that particular architecture, right? Well, let’s understand the architecture on the basis of that here.
So, typically, the legacy systems follow a monolithic architecture that is made up of tightly coupled data, logic, and User Interface. Whereas, with custom EHR, you can adopt a modern architecture that is built on cloud-native with an API-first approach. This forms the major foundation of your EHR system, which makes it easy to update, integrate, and adapt to your ever-changing clinical and regulatory needs.
Furthermore, when you choose to develop a custom EHR, you usually follow a modular design, where your clinical workflows, billing workflows, integration capabilities, analytics, and UI operate as independent components, but are connected with each other. Due to this keen separation, updating and replacing individual modules becomes easy. For instance, if you want to add AI or RPM features to your EHR system, then it can be easily done, and you don’t have to rewrite the programming of the entire system.
One of the major parts of architecture also includes data storage, its accessibility, and sharing capabilities. Now, with a custom EHR following a modular approach, complying with HIPAA regulations, and implementing role-based access control becomes much easier. Furthermore, with FHIR HL7-based APIs, interoperability can be easily achieved, supporting scalability.
And this becomes the foundation of your custom EHR system architecture.
Core Architectural Patterns in Custom EHR Development
If you have read the earlier section, then you must have got an idea about the core architectural patterns that are typically used in custom EHR software architecture – monolithic and microservices architecture.
Refer to the table below for a better understanding:
| Aspect | Monolithic Architecture | Microservices Architecture |
| System Structure | All EHR functionalities (clinical, billing, scheduling, reporting) are tightly bundled into a single codebase | EHR features are broken into independent services (clinical, billing, integrations, analytics, etc.) |
| Scalability | Scales the entire system together, even if only one module needs more resources | Each service scales independently based on workload (ideal for high-volume clinics) |
| Development Speed | Faster to build initially but harder to modify as complexity grows | Slightly higher initial effort, but faster long-term development and iteration |
| Maintenance & Updates | Small changes can require full system redeployment | Individual services can be updated without impacting the entire EHR |
| Fault Isolation | A failure in one module can affect the entire system | Issues are isolated to specific services, improving system reliability |
| Interoperability | Limited and harder to extend integrations over time | API-first design enables seamless FHIR/HL7 and third-party integrations |
| Compliance Management | Compliance controls are applied system-wide, making changes risky | Security, audit logs, and access controls can be enforced per service |
| Customization Flexibility | Customizations increase system complexity and technical debt | Specialty-specific workflows can be customized as separate services |
| Performance Under Load | Performance degrades as user volume and data grow | Designed to handle high concurrency and large data volumes efficiently |
| Best Fit For | Small practices with simple workflows and limited growth plans | Growing practices, multi-location providers, and compliance-heavy environments |
For a better deep dive into monolithic and microservice architecture, click here to read the detailed blog – Microservices vs Monolithic Architecture for EHR Development.
Interoperability in Custom EHR Systems
Interoperability in custom EHR systems is one of the core aspects that you need to keep in mind when designing the architecture of your software. This is necessary because you need your system to effectively communicate with other healthcare systems, so that they can exchange data effectively and efficiently.
To break the possibility of data silos across providers, labs, pharmacies, and payers, you need to achieve interoperability. For this, one of the best ways to do that is to standardize interoperability standards such as HL7 and FHIR. Since these standards make it easier for your system to exchange data, it becomes easier for you to maintain continuity of care and enhance not only data flow but also the quality of care that is being provided to your patients.
Read our latest blog about – The role of interoperability in custom EHR systems for better understanding and in-depth understanding.
Custom EHR Integration Architecture & Ecosystem Collaboration
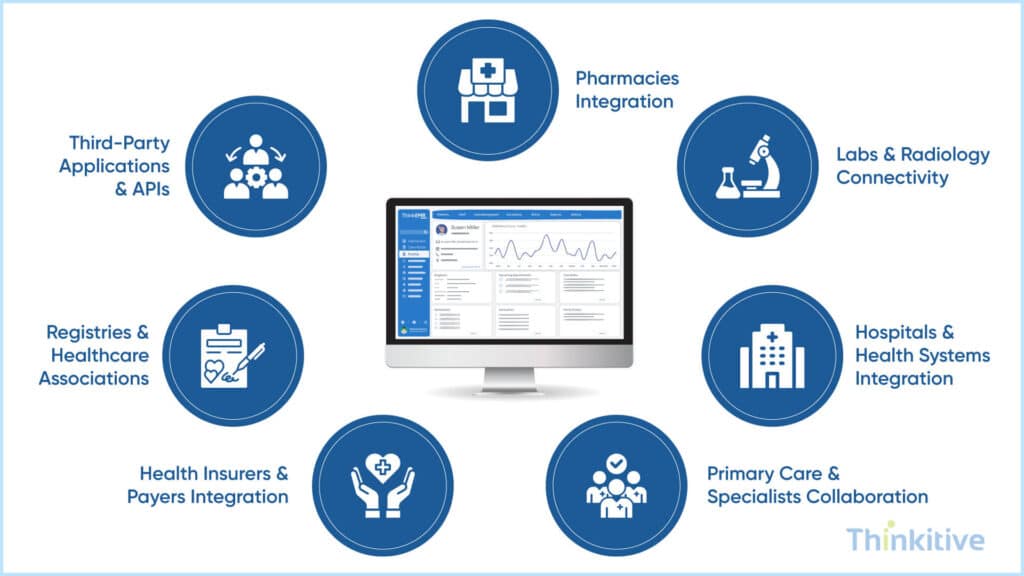
After interoperability, the next thing that you need to emphasise in your custom EHR system architecture is integration. You see, only when your system is able to communicate and exchange data with other healthcare software systems can you provide the right care to your patients.
For this, one of the best practices that is used in custom EHR integration architecture is API-first design. In recent development ventures, API-first design of EHR software has become the backbone of modern EHRs. Since they allow much faster data transfer and directly establish a connection with the system you want to share data with.
On top of that, it makes it easier for your system to establish integration with third-party systems like labs, radiology, billing, and even RPM devices and platforms.
Following the best practices in integration support ecosystem-level healthcare collaboration allows your systems to seamlessly exchange data with other systems. Read an in-depth blog – Custom EHR Integration and Ecosystem Collaboration.
Secure & Compliant EHR Architecture by Design
Your EHR software system will deal mainly with the data that is quite sensitive in nature. That is why the security of that data is one of the most important aspects that you need to cover in your custom EHR software architecture.
On top of that, since you deal with the private and personal data of your patients, data theft in your system can lead to breaches of their fundamental rights. That is why the government has established some regulatory bodies that you need to be compliant with. Let’s have a look at each aspect one by one.
Secure & Compliant EHR Development Guide
Free DownloadSecurity as an Architectural Requirement
Some of the features or core components for a secure and compliant EHR architecture that you need to include are data encryption, access control, and auditability. These core elements allow your system to be more secure. You see, with data encryption, your data becomes hard to read for unknown systems with the right key. Furthermore, with access control, only authorised personnel can access the data in your system, and auditability allows you to review all the activities that are happening in your system.
If you want to know about security and compliance, then read our detailed blog – Custom EHR Development: interoperability, Security & Compliance.
Navigating Regulatory Compliance in Custom EHR Systems
There are certain rules and regulations established by the government to ensure the safety and privacy of patient data that is used by healthcare software systems. While designing the architecture of your custom EHR software, some of the architectural implications that you need to follow are HIPAA, ONC, and CMS.
Each of these compliances and regulatory bodies has different requirements, and adhering to those will help you navigate the landscape easily. And with compliance with these regulations, you can avoid hefty fines, penalties, and reputation damage.
Furthermore, these regulations are constantly changing, so designing the system architecture accordingly is very important. If you want to know in detail about the regulatory landscape, then read our in-depth blog, Custom EHR Regulatory Landscape.
EMR vs EHR Compliance Scope in Custom Systems

The compliance of your system also differs depending on the type of record-keeping system you are developing. For instance, if you are developing an EMR system, the compliance scope is quite limited as there are only a limited number of systems that you need to connect with. On top of that, you only collect the data that is limited to your clinic, and that makes all the difference.
In an EMR system, some of the main compliance areas that are under focus are data security, access control, and basic HIPAA requirements.
However, if you are developing an EHR system, the compliance scope is quite broad. This is because your system needs to be integrated with many systems, both inside and outside of your ecosystem. Furthermore, since your system will contain the entire medical history of your patients, the scope of security and compliance increases and is quite strict in nature.
Some of the expectations in an EHR system are based around interoperability, standardized data formats with FHIR HL7 formats, auditability, separate consent management, and adherence to information blocking rules.
For more details, read our blog – Navigating EMR Regulatory Compliance.
Architectural Considerations When Transitioning from EMR-Centric Systems to Interoperable EHRs
Moving from an EMR to an EHR system requires a shift from a closed, database-centric architecture to a module that is API-driven and follows a modular architecture. For this, your system must support standardized data models, allow real-time data exchange, have role-based access control, and have the capability to provide comprehensive audit logs.
This means you need to decouple core clinical data from presentation layers and introduce integration services by designing them for scalability. This way, you can ensure they can fully support HIEs, third-party apps, and multi-location workflows without compromising performance and compliance.
You can read in detail about how to navigate regulatory compliance in the blog, Navigating EMR Regulatory Compliance.
Scalability Considerations for Custom EHR Solutions
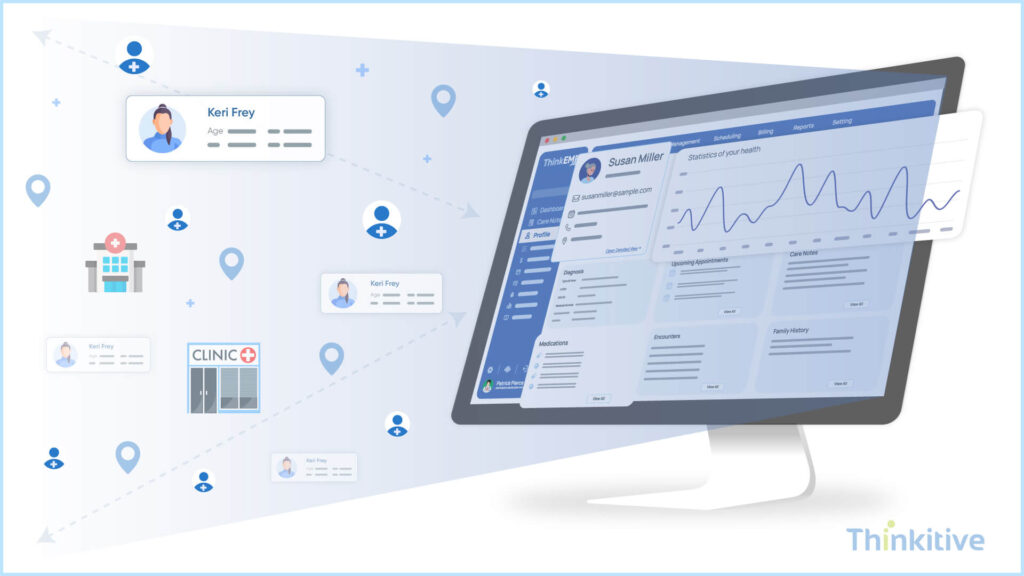
With time, your practice is bound to grow and to accommodate your growing needs; your custom EHR needs to scale accordingly. Some of the things that you need to keep in mind with respect to this are a growing number of users, growing patient data, and expanding clinical operations.
Some of the scalability considerations for custom EHR are finding the right balance between horizontal scaling and vertical scaling. For instance, vertical scaling increases the system capacity by adding more resources synchronously, such as CPU and memory, to a single service. On the other hand, with horizontal scaling, you can distribute workloads across multiple servers or services, allowing your EHR system to handle growth more reliably and cost-effectively.
However, if you are looking to open multiple practices at different locations with respect to enterprise growth, then your EHR architecture must be cloud-ready, modular in nature, and driven by APUs. This includes curation of centralized patient records with location-specific workflows and shared identity and access management, load balancing, and standardized integrations.
This is one of the best ways to prepare your system for future growth and scalability. Furthermore, we have created a detailed blog about scalability, read – Scalability Considerations for Custom EHR Solutions.
Step-by-Step Guide to Build Scalable EHR
Free DownloadHow to Design a Scalable & Compliant Custom EHR Architecture
If you have been patient and made it till here, then you must have covered all the aspects of understanding custom EHR architecture, compliance, and scalability. But the question that you might be getting here is, ‘How to design a scalable and compliant custom EHR architecture?’
Well, let’s break this down. First things first, you need to have an architecture-first planning and plan your development phase accordingly. In simple terms, what I mean by this is to align your business goals with compliance needs and try to fit that with technical scalability requirements.
And you need to plan this early, because when you make architecture-based decisions, long-term ROI can be easily defined, and when the time comes to make drastic changes, it can be done easily and effectively without much worry.
Future-Ready Custom EHR Architecture
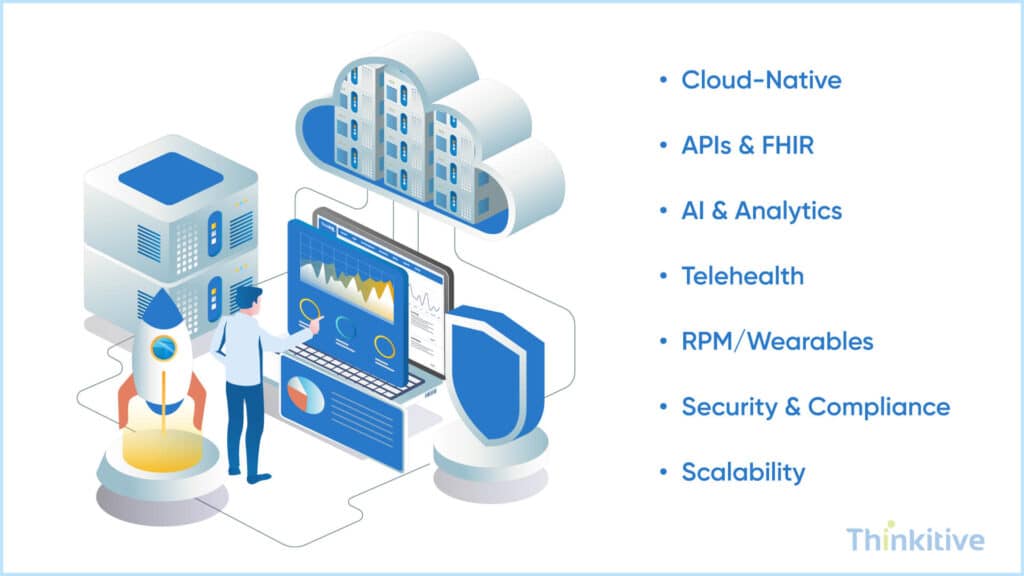
Furthermore, the healthcare industry and the technological landscape are constantly changing. What is trending today may not be trending tomorrow or might even be scrapped out, right? In such cases, you need to have a future-ready custom EHR system architecture. Some of the considerations in this are:
- Enabling AI-Driven Decision Support & Analytics: Since AI is the talk of the town, integrating it into your system can help you in making better decisions and even give your system exceptional analytical skills unmatched by any other system.
- Support Telehealth, RPM, and Value-Based Care Models: The winds in the healthcare industry are indicating virtual care delivery models. That is why we developed a custom EHR software architecture that supports telehealth platforms for virtual consultations, RPM for remote patient monitoring, and value-based care models to give patients value for what they seek.
And as mentioned earlier, prepare for the future with interoperability and other regulatory options.
Conclusion
If you have made it this far, then you have been extremely patient and serious about building a custom EHR software. And architecture being an integral component of it, I hope this blog has covered all the necessary things from microservices vs monolithic EHR architecture to the scalability and interoperability needs for your custom EHR.
On that note, let this blog be your guide to understanding custom EHR architecture, compliance, and scalability. And if you are looking for a reliable and trusted partner to develop your custom EHR, then Click here to assess your system and get started.
Frequently Asked Questions
Custom EHR software architecture defines how clinical, administrative, and data components are structured, connected, and secured within an EHR system. It is critical because modern healthcare demands interoperability, regulatory compliance, scalability, and performance—all of which are directly influenced by architectural decisions. A well-designed custom EHR architecture ensures long-term flexibility, safer data handling, and smoother clinical workflows.
Off-the-shelf EHR platforms typically use rigid, one-size-fits-all architectures with limited extensibility. In contrast, custom EHR system architecture is designed around specific clinical workflows, specialty needs, and growth plans. Custom architectures allow modular enhancements, deeper integrations, better performance tuning, and easier compliance updates over time.
Architecture choices directly affect how data is secured, shared, audited, and scaled. Designing these elements in isolation often leads to compliance gaps, performance bottlenecks, or costly redesigns. A secure and compliant EHR architecture ensures that regulatory requirements (HIPAA, ONC, HITECH) are met while supporting future growth without disrupting care delivery.
EHR architecture determines how well systems communicate with external entities like labs, pharmacies, HIEs, payers, and patient apps. Architectures built around FHIR APIs, HL7 standards, and service-based integration enable seamless data exchange, reduce vendor lock-in, and support value-based care models—making interoperability in custom EHR systems achievable and sustainable.
Security is foundational—not an add-on. Custom EHR architecture embeds security at every layer through role-based access control (RBAC), encryption, audit logs, MFA, and secure APIs. Architectural security ensures protected health information (PHI) remains confidential, tamper-proof, and traceable across all workflows and integrations.
Custom EHR architecture supports regulatory compliance by enforcing data access controls, auditability, encryption standards, breach monitoring, and data retention policies at the system level. This proactive design approach simplifies HIPAA compliance, supports ONC certification needs, and adapts more easily to evolving regulatory frameworks.
Legacy EHR systems often struggle with:
- Performance degradation as data volumes grow
- Limited support for multi-location expansion
- Inflexible infrastructure scaling
- High upgrade and maintenance costs
These issues stem from monolithic designs that were never built for modern scalability demands.
In microservices vs monolithic EHR architecture, microservices offer clear advantages. Each function (billing, scheduling, clinical documentation, analytics) operates independently, allowing healthcare organizations to scale features selectively, deploy updates faster, and improve system resilience—making it ideal for scalable EHR software architecture.
Effective custom EHR integration architecture requires:
- API-first design
- Standardized data models (FHIR/HL7)
- Secure authentication and authorization layers
- Fault-tolerant integration services
These considerations ensure smooth interoperability without compromising security or system performance.
Modern custom EHR architectures separate data, application logic, and analytics layers—making it easier to introduce AI-driven clinical decision support, predictive analytics, population health tools, and real-time insights without disrupting core operations.
Poor architectural decisions can lead to:
- Compliance violations and audit failures
- Increased security vulnerabilities
- High technical debt
- Slow innovation and costly upgrades
Over time, these risks can significantly impact operational efficiency and patient trust.
Organizations should start by aligning architecture with:
- Clinical workflows and specialty needs
- Regulatory requirements
- Interoperability goals
- Long-term growth plans
Partnering with experienced healthcare IT teams helps organizations design a scalable and compliant custom EHR architecture that balances performance, security, and future readiness.




