EHR Interoperability: The Definitive Guide to Connected Healthcare Systems
The talks of the connected healthcare ecosystem has reached every hospital, clinic and digital healthcare practices. In fact, back in 2021, Office of the National Coordinator of Health for Health Information Technology, reported that 70% of the healthcare systems are interoperable in nature.
However, the need for medical data exchange is always a need for practice. That is why, the demand for EHR interoperability amongst healthcare practices is usually seen higher. But why has this reason become one of the growing concerns for healthcare organizations?
Well, have a look at it this way!
After a deeper analysis of the healthcare system and patient behaviors, according to this report, 89% of patients who switched providers reported ease of navigation and interoperability as their primary reason. In fact the same report also suggested that 44% of the patients report poor clinical experience and 13% reported network issues as their primary concerns for switching.
This shows that while most of the systems are connected, they are not able to share information seamlessly and for many systems, the data stored in other systems simply doesn’t make sense.
You see, many practices focus on integration, while their requirement is usually for interoperability. Here you need to understand that your system can truly achieve EHR integration when it truly achieves EHR interoperability.
But as someone from a non-technical background, understanding why this makes so much sense is important, right?
On that note, let this blog be your definitive EHR interoperability guide for building a connected healthcare system.
So without further ado, let’s get started!
What is EHR Interoperability in Healthcare?
To define EHR interoperability in simple words, it can be termed as the ability of different EHR systems to connect with disparate healthcare applications to that exchange, update and make sense of the data to be used for clinical and administrative purposes.
Many confuse it with simply transferring for data, whereas it is beyond that, as accurate, standardized and meaningful data is involved. Furthermore, there are four levels of EHR interoperability. Here is a brief table for you to understand all four EHR interoperability levels:
| Level | Definition | Key Focus | Technologies / Standards | Example | Limitations |
| Foundational Interoperability | Basic ability of systems to send and receive data | Data exchange (connectivity) | Basic interfaces, file transfer protocols | A hospital sends patient data to another system | Data may not be understood or usable by the receiving system |
| Structural Interoperability | Data is exchanged in a standardized format with preserved structure | Data format and organization | HL7, FHIR | Lab results shared with predefined fields (e.g., test name, value, unit) | Systems can read data but may not fully understand its meaning |
| Semantic Interoperability | Systems interpret and use data with shared meaning | Data meaning and clinical context | SNOMED CT, LOINC, FHIR | Diagnosis recorded in one system is interpreted correctly in another | Requires complex standardization and mapping across systems |
| Organizational Interoperability | Alignment of workflows, policies, and governance for seamless data exchange | Processes, compliance, and collaboration | HIPAA frameworks, data governance models, HIEs | Hospitals, labs, and insurers sharing patient data securely under defined protocols | Requires coordination across multiple stakeholders and regulatory compliance |
Why Has Interoperability Become So Important?
As a healthcare provider you know that for normal data exchange in your practice, your system has to depend on many systems, right from labs to payers and what not. And since all these healthcare service providers act independently, they have their data stored in their system.
Due to this data silos are created in their systems. This creates interruptions in care delivery and other administrative aspects, as the entire process of care delivery has become data oriented. Meaning, for reimbursement or care delivery, your practice depends on other healthcare systems.
Moreover, this shift to digital practices have also been brought forth by 21st Century Cures Act, ONC rules and even CMS conditions. This has made it essential for healthcare practices to achieve healthcare interoperability.
How EHR Interoperability Works in Connected Healthcare Systems
Now that we have covered most of the intricacies about EHR interoperability, let’s now understand how this works in connected healthcare systems. And one of the best ways to understand this is by understanding the flow of data and let’s take an example to understand this better:
So, the data usually or typically flows from one healthcare provider, let’s call it A to another healthcare provider, let’s call it B. Now, the core components involved in this process of exchanging data from one system to another in a healthcare setting is through:
- EHR system: where data is stored
- APIs and Middleware: The mediators that connected system A with system B
- Healthcare Information Exchanges: Systems that allow disparate healthcare providers to securely connect and share information electronically
Now, let’s understand the actual flow. So, for System A to retrieve data from System B, the EHR in system A triggers a call through an API gateway. Here, the middleware acts as a secure bridge between the two systems—a part of the HIE network—to identify the correct patient information that is to be extracted into your local record.
Now that you have known the components and the flow of data from one system to another, let’s move forward about the intricacies of healthcare data interoperability.
Medical Data Exchange: Standards, Protocols, & Best Practices
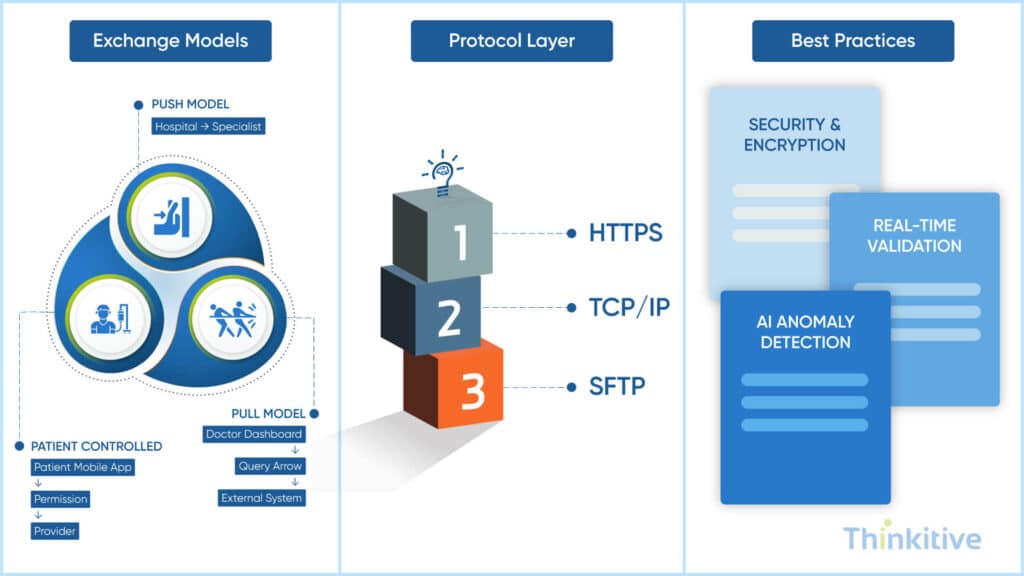
In healthcare interoperability, medical data exchange forms the foundation. In simple terms, there are certain standards, protocols and best practices that enable secure communication between systems. On that note, let’s explore that one by one:
The Three Layers of Exchange
- Direct Exchange: This is also called the ‘Push’ model where healthcare providers send patient information directly to another system. These types of exchanges are typically secure and point-to-point in nature, furthermore, the initiation is usually done by the sender.
- Query-Based Exchange: While the other model is called ‘Push’, this model is called ‘Pull’ based model where the provider searches for and retrieves on demand, whenever the provider of the external system is needed. Here, the data is fetched in real-time and required patient matching and access permissions.
- Consumer-Mediated Exchange: Unlike the previous model, this model is controlled by patients and they decide how to share their data with providers. In short the permission about data retrieval is given to my patient and it is typically API based.
Now, true interoperability is something where three exchange models—push, pull and patient-mediated—work together to create a connected healthcare ecosystem. Only when these layers work in union, can you ensure that the right data is available at the right time and that too in the right context.
Other than these layers of exchange, here are some of the essential protocols that you need to know:
- HTTPS: This stats for Hypertext Transfer Protocol Secure, it is basically a primary protocol used for secure web-based communication. All modern API-driven healthcare systems use this protocol for secure sharing. Data in this is encrypted using SSL/TLS and widely uses RESTful APIs.
- TCP/IP: It stands for Transmission Control Protocol or Internet Protocol. It acts as a core communication framework of the internet where it enables reliable data transmission between systems. This protocol breaks data into packets and reassembles them. Its role in healthcare is that it supports all EHR data exchange over networks and ensures data integrity during transmission.
- SFTP (Secure File Transfer Protocol): This type of protocol is used for secure file-based data transfer, it is typically seen in legacy or batch-processing healthcare systems. Furthermore, it encrypts both commands and data and supports uploads and downloads.
Some of the best practices that you can use for medical data exchanges is by using AI. You see, the AI embedded into the system will monitor traffic patterns that are being transferred from one system to another. In this process, the system can detect anomalies in real-time, giving you an edge by strengthening your interoperability.
EHR Data Mapping: Solving Complexity in Multi-System Environments
One of the most commonly used terms in interoperable electronic health records is data mapping. This data mapping forms the bedrock of your interoperability. Let’s understand EHR data mapping before uncovering the role it plays is medical data exchange:
So, EHR data mapping is nothing but the process of matching data fields between different system—typically information systems like EHR systems—to ensure that the health information that is being transferred is exchanged accurately and consistently.
To understand this in simple words, have a look at this example, there are two systems which use distinct terminologies, formats, or proprietary codes for storing data. Now, data mapping here acts as a translator that pairs the data element from a source system to the target system.
Now, for a system, the biggest challenge that it faces is that it finds it difficult to correct data from the different systems with each other. Or else, you might request one information and get something else, imagine how irritating that would be, right?
This is where EHR data mapping comes into the picture, and if you are a practice that depends on multi-system connected healthcare environments, then EHR data mapping can become a live saver for you.
You see, with the data mapping process, your system gets the ability to translate the data into a format that is structured and meaningful.
And the first barrier that you’ll face is the semantic barrier, where your system have to navigate through different coding system, such as:
- LIONC – typically used for lab tests and observations
- SNOMED CT – Used for diagnoses and clinical concepts
Data mapping becomes important here because without that the chances of misinterpretation of clinical data increases, along with incomplete patient records ultimately leading to poor clinical decisions.
AI-Powered Crosswalks
While overcoming the semantic barrier, the gap between data exchange and data understanding, your system becomes smarter. However, with the use of AI it can lead to smarter data mapping, where you move from manual rule-based mapping to AI-driven mapping, which will make your barrier faster, error prone and hard to scale. This can be done with the use of machine learning models to create intelligent crosswalks between disparate datasets.
Here the system can learn from the patterns used in different coding systems and smartly predict correct field mapping. This way, adapting to new data formats becomes much easier and interoperability is scaled.
Data Integrity: Structuring Unstructured Clinical Data
It is not a secret anymore that most of the part of healthcare data is unstructured, some of the most prominent examples of this are physician notes, discharge summaries or clinical narratives.
The challenges in this unstructured data are often related to exchanges, mapping and analyzing. This is why ensuring data integrity is clinically important, and the best solution to this is NLP – natural language processing.
With this you can extract key clinical entities and convert free text into structured data fields which ensure consistency in data across your systems.
Healthcare Data Migration: Moving Patient Records Between Systems Safely
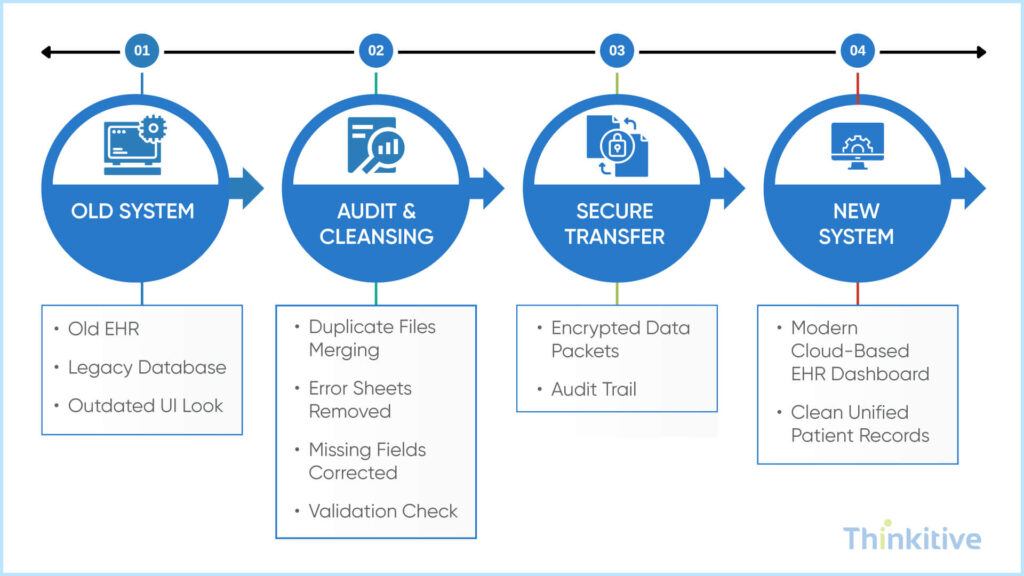
Along with data mapping, data migration is also something that you should be aware of, when it comes to EHR interoperability. You see, EHR interoperability is not just about connecting systems, in the process, it often requires moving large volumes of patient data from one system to another. And this process is called healthcare data migration.
It is critical for system transitions so that you can ensure data accuracy, security and continuity of care. But you do not require to move patient records every time right?
On that note:
When is Data Migration Required?
There are typically three instances when a healthcare practice requires data migration. Here are those scenarios:
- EHR system replacement (switching vendors or platforms)
- Mergers and acquisitions (consolidating multiple systems)
- System upgrades or modernization (moving to cloud or new architecture)
There might be some other factors that might require you for data migration. But if you are going ahead with the data migration process, then here are a few things that you need to know:
Pre-Migration Auditing: Fixing ‘Dirty Data’ Before it Moves
Before migrating data, you must organize a comprehensive data audit to cleanse your data. Some of the major processes that are involved in this are:
- Identifying duplicate patient records
- Detecting missing or inconsistent data fields
- Standardizing formats such as dates, units, and codes
- Validating clinical accuracy
You need to fix this dirty data because if the same quality data is transferred into a newer system, the problems will still remain the same. Furthermore, for this process, you can use AI to eliminate deduplication and patient identity resolution. For instance, it can help you in matching patient records across datasets, identify duplicates with high accuracy and merge records into a single file. This reduces clinical risk and leads to better coordination.
Maintaining Data Lineage & Auditability
One of core concepts of interoperable electronic health records is that it not only allows you to exchange data but also helps in tracking where that data came from and how it has been changed. This is called data lineage, where it gives your system the ability to trace the origin of data, track the transformation applied during migration and how the data has moved across systems.
It is important because it aligns with HIPAA compliance’s regulatory requirements, supports audit and legal requirements and stands as a core factor that helps in building trust and ensuring data accuracy.
EHR Interoperability Standards: From HL7 to FHIR & Beyond
Too much technical information till now, right?
Even for a technical person, processing and making sense of this much information can be overwhelming. Well, a similar situation happens with the systems, as they are not able to understand the language that we speak. You see, every healthcare system talks in binary.
Having said that, for allowing your system to understand and speak the same language, using certain EHR interoperability standards are required. This table will give you a brief idea about them:
| Component | Definition | How It Works | Key Benefits | Limitations |
| HL7 v2 | A legacy messaging standard for healthcare data exchange | Uses structured messages (e.g., ADT, ORU) sent between systems | Widely adopted, reliable for existing integrations | Complex, hard to scale, limited flexibility |
| FHIR (Fast Healthcare Interoperability Resources) | A modern standard for exchanging healthcare data using APIs | Uses RESTful APIs and modular resources (Patient, Observation, etc.) | Real-time data access, flexible, developer-friendly | Requires modernization of legacy systems |
| SMART on FHIR | A framework for building apps that integrate with EHRs using FHIR | Uses FHIR APIs + OAuth 2.0 for secure app access | Enables app ecosystems, plug-and-play integrations | Dependent on FHIR adoption and EHR support |
The use of AI here also can be extremely useful. You see, while standards like HL7 and FIR define how data is being exchanged, the problem comes in bridging the gap between legacy and modern systems. This is where AI-driven transformation is playing a critical role in this.
Major Benefits of Interoperable Electronic Health Records
Having an interoperable EHR system has benefits that can be across the system and almost all the aspects of your practice. Here are some of the benefits:
- Clinical: For the clinical aspects of care delivery, the chances of errors are eliminated, as data is readily available and consistency is maintained bringing the entire care team on the same page. Due to these aspects decision-making process is improved massively, leading to accurate and enhanced care delivery.
- Financial: The financial aspects of practices are also improved with EHR interoperability. For instance, it streamlines workflows, simplifying data flow and evidence at every instance. This reduces administrative burden massively, improving the overall financial health of the practice.
- Strategic: It also involves some strategic benefits as it enables population health management and allows you to imbibe value-based care models, giving you an edge in care delivery and administration.
- Patient-Centric Care: With interoperability, you keep data at the epicenter of your practice’s every aspect right from care delivery to claims submission. This makes your practice adopt a patient-centric care approach, improving patient access, engagement and care coordination.
Overcoming Interoperability Implementation Challenges
EHR integration is necessary as it allows your system to connect with other systems and exchange information. However, to achieve true EHR integration, you need to achieve true interoperability as it helps in solving complexities that arise in real-time exchange and semantic consistency.
However, achieving interoperability is easier said than done. The process is filled with challenges that you have to overcome. On that note, here are some of the most common challenges that you’re likely to encounter with EHR interoperability and here is how you can overcome them:
| Challenge | Description | How to Overcome |
| Legacy Systems & Vendor Lock-in | Older EHR systems use outdated architectures and proprietary formats, making integration difficult | Adopt API-first strategies (FHIR), use middleware/integration engines, and gradually modernize legacy systems instead of full replacement |
| Data Silos Across Fragmented Ecosystems | Patient data is scattered across hospitals, labs, and clinics, limiting visibility and care coordination | Implement Health Information Exchanges (HIEs), centralized data platforms, and interoperable APIs to unify data access |
| Semantic Inconsistencies Across Systems | Different coding systems and formats lead to misinterpretation of clinical data | Use standardized terminologies (SNOMED CT, LOINC), implement data mapping frameworks, and leverage AI for semantic normalization |
| Security, Privacy & HIPAA Compliance | Sensitive patient data must be protected during exchange and storage | Enforce encryption (HTTPS, TLS), role-based access control, audit trails, and compliance frameworks (HIPAA, GDPR where applicable) |
| Cost vs Long-Term ROI | High upfront investment in interoperability infrastructure can deter organizations | Focus on phased implementation, prioritize high-impact use cases, and highlight long-term savings (reduced duplication, improved efficiency) |
| Scalability in Real-Time Data Exchange | Increasing data volume and real-time demands strain system performance | Use cloud-based infrastructure, scalable APIs, microservices architecture, and event-driven data exchange models |
The Future of Healthcare Interoperability
The landscape of healthcare interoperability is rapidly evolving. Right from the standards to the regulatory requirements, the process of evolution seems to be never stopping. This can be even reflected in the nature of interoperability as it has moved from basic data exchange to intelligent, real-time and more patient-centric ecosystems.
With respect to the advancements in EHR interoperability, here are few aspects about EHR interoperability that you should know:
- API-First & FHIR-First Architecture: Modern healthcare systems are adopting API-first and FHIR-first architecture as it builds interoperability into the system. Due to this data becomes accessible in real-time and integration becomes faster and reliable. Moreover, it reduces dependency on complex and custom integrations.
- Rise of AI as Interoperability Layer: AI has already made its space as a critical layer on top of interoperability framework. This has helped healthcare practices solve traditional challenges like data mapping and normalization, patient identity resolution, automation of workflows, etc.
- SMART on FHIR: SMART on FHIR frameworks is driving a shift that is making healthcare a platform-based ecosystem. With this the EHRs are no longer closed systems, due to which third-party apps can plug into core systems and drive innovation. This has proven to be crucial for clinical decision support, remote monitoring and driving engagement.
Furthermore, one of the latest anticipations in interoperability is said to be driven by continuous and real-time data streams. This is a hint for practices to prepare for IoT, remote monitoring and real-time care delivery. For this you need to integrate your system with wearable devices or IoT sensors, along with RPM systems. This will fuel the shift from reactive care delivery to proactive care delivery.
Conclusion: The Road to Truly Connected Healthcare Systems
If you have made it till here, then you must know that interoperability is the strategic foundation for modern healthcare practices. In simple words, it gives your system the ability to make sense of the data so that you can use it effectively.
Moreover, with modern practices you can move beyond simple data exchange mechanisms to an intelligent connected ecosystem that bridges all the gaps between disparate systems that you want to connect with.
On that note, ready to bridge the gap between your system and other disparate systems? Learn how interoperability can benefit your practice, get your first consultation.
Frequently Asked Questions
EHR interoperability refers to the ability of different systems to exchange, interpret, and use patient data seamlessly across platforms and organizations. In simple terms, it ensures that interoperable electronic health records can move across providers while remaining accurate and meaningful.
In this EHR interoperability guide, it’s important to understand that interoperability goes beyond basic data sharing—it enables connected healthcare systems where information is accessible, standardized, and actionable.
The four levels of healthcare interoperability include:
- Foundational – Basic data exchange between systems
- Structural – Standardized data formats (e.g., HL7, FHIR)
- Semantic – Shared understanding of data meaning
- Organizational – Aligned workflows, policies, and governance
These levels collectively enable effective healthcare data interoperability across systems.
Understanding how EHR interoperability works in healthcare systems involves multiple layers:
- Data exchange through APIs and standards like HL7 and FHIR
- Secure transmission using protocols like HTTPS
- Data mapping and normalization for consistency
- Integration across providers, labs, and applications
This enables connected healthcare systems where patient data flows seamlessly across the care continuum.
Medical data exchange refers to the ability to send and receive data between systems, while healthcare data interoperability ensures that the data is also understood and used correctly.
In other words:
- Data exchange = transfer of information
- Interoperability = meaningful use of that information
HL7 and FHIR standards differ primarily in their approach:
- HL7 v2 uses message-based communication and is widely used in legacy systems
- FHIR uses API-based communication for real-time, flexible data exchange
FHIR is more modern, scalable, and better suited for connected healthcare systems.
FHIR is considered the future because it enables:
- Real-time data access through APIs
- Easier integration with modern applications
- Scalable and flexible architectures
These capabilities make FHIR essential for building interoperable electronic health records and advancing healthcare interoperability.
APIs act as the bridge between systems, enabling secure and real-time medical data exchange.
In modern healthcare interoperability, APIs:
- Allow systems to communicate instantly
- Support FHIR-based integrations
- Enable third-party app ecosystems
They are foundational to how EHR interoperability works in healthcare systems today.
EHR data mapping ensures that data from different systems is aligned, standardized, and interpreted correctly.
It helps:
- Resolve differences in coding systems (e.g., SNOMED, LOINC)
- Normalize data formats
- Enable accurate healthcare data interoperability
Without proper mapping, even connected systems cannot achieve meaningful interoperability.
The key benefits of interoperable electronic health records include:
- Improved care coordination
- Reduced duplicate tests and errors
- Faster clinical decision-making
- Enhanced operational efficiency
- Better patient outcomes
These benefits make interoperability essential for modern connected healthcare systems.
AI enhances healthcare data interoperability by:
- Automating data mapping and normalization
- Identifying duplicate patient records
- Structuring unstructured clinical data using NLP
- Improving data accuracy and consistency
This significantly strengthens medical data exchange across systems.
Key barriers to effective medical data exchange include:
- Legacy systems and vendor lock-in
- Data silos across organizations
- Semantic inconsistencies
- Security and compliance challenges
- High implementation costs
Overcoming these is critical to achieving true healthcare interoperability.
Secure healthcare data migration requires:
- Encryption protocols (HTTPS, TLS)
- Access controls and authentication
- Data validation and auditing
- Compliance with regulations like HIPAA
These measures ensure safe and compliant transfer of sensitive patient data.
Interoperable electronic health records reduce manual data entry and streamline workflows.
This leads to:
- Less time spent searching for patient data
- Reduced duplication of work
- Faster access to complete records
As a result, healthcare interoperability plays a key role in reducing clinician burnout and improving efficiency.




