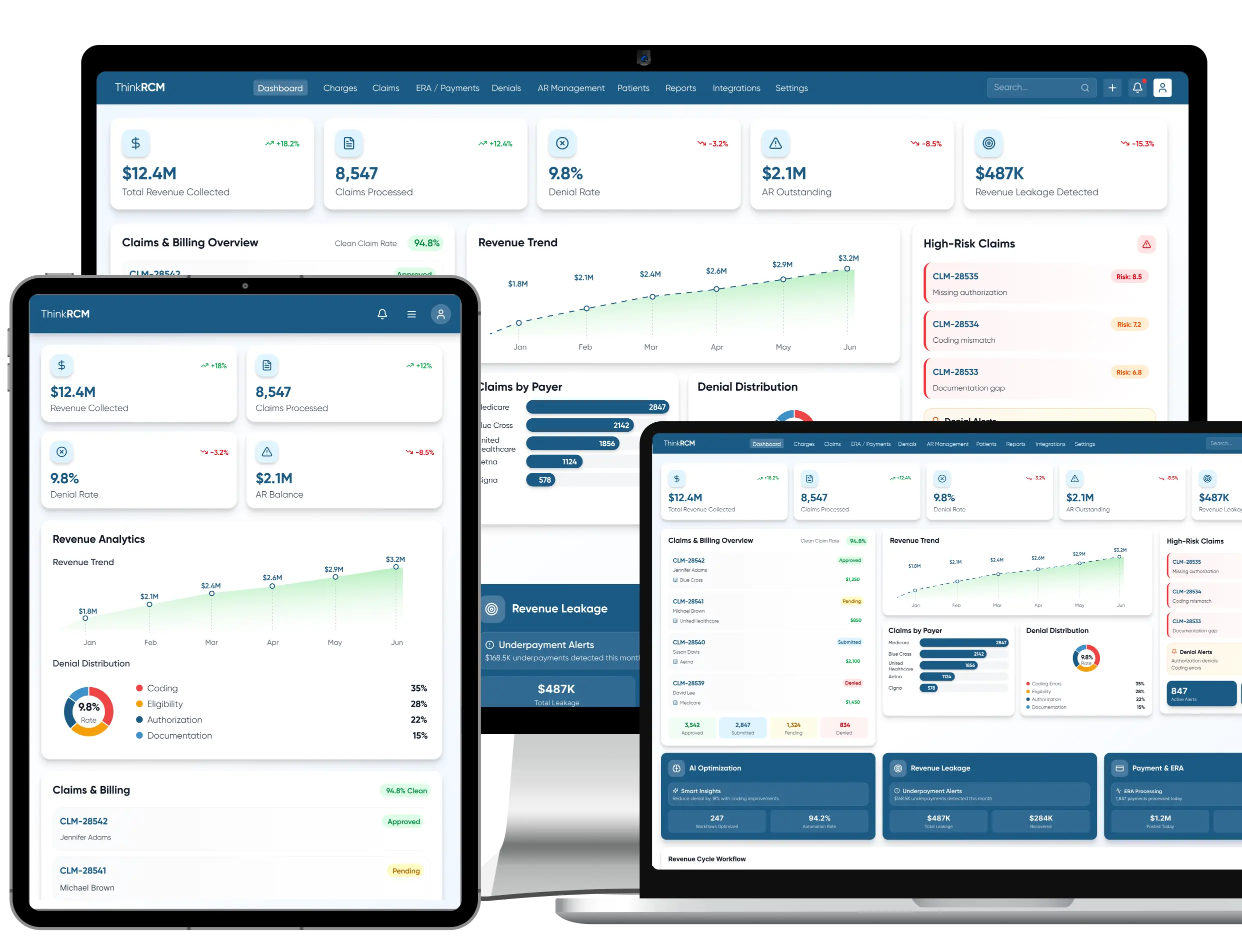
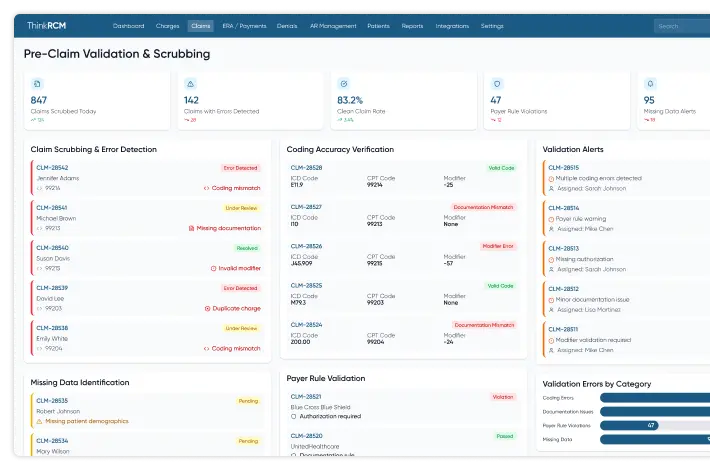
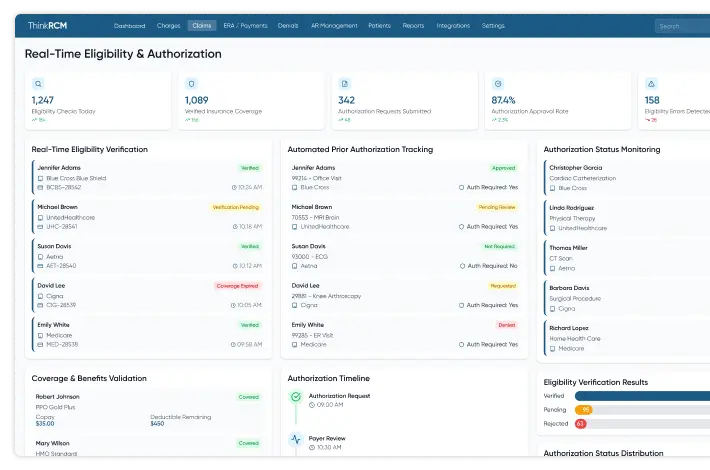
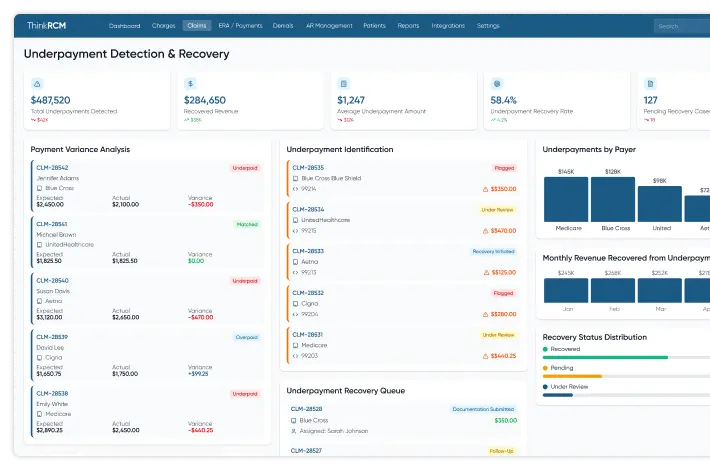
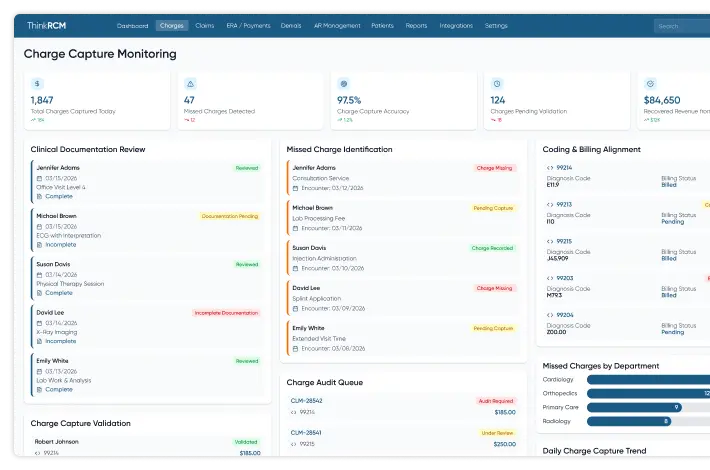
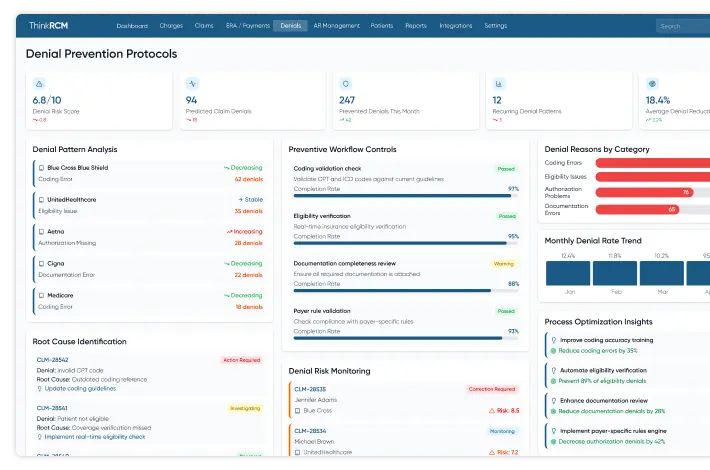
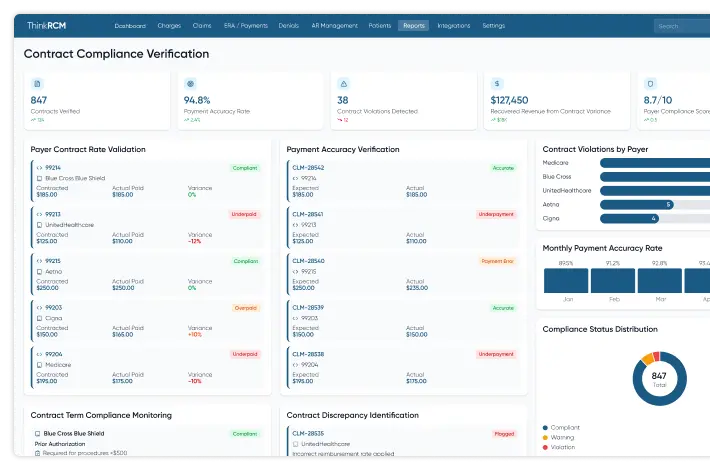
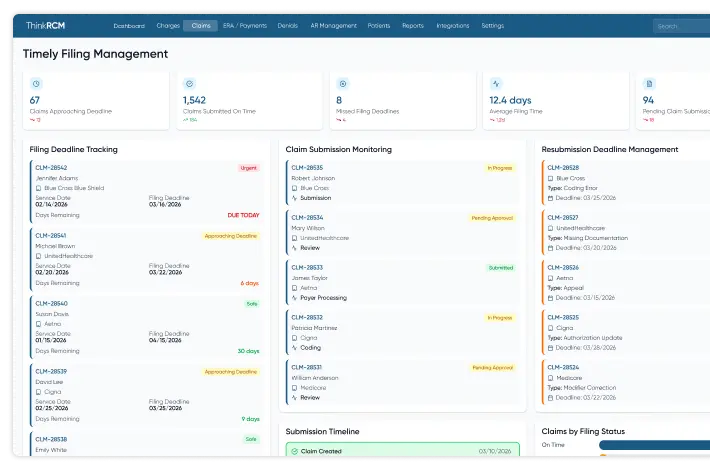
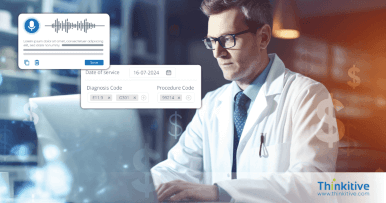
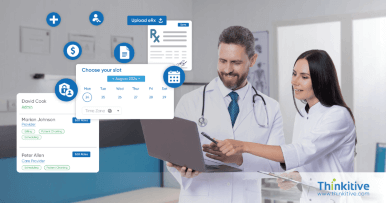
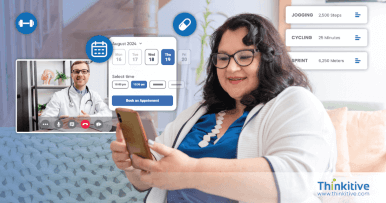
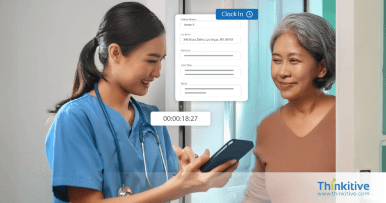
Strengthen Revenue Integrity & Prevent Revenue Leakage with Denial Management Services Healthcare
From pre-claim validation to underpayment recovery, proactive revenue leakage prevention services help healthcare providers identify revenue gaps, reduce claim denials, and improve reimbursement accuracy.

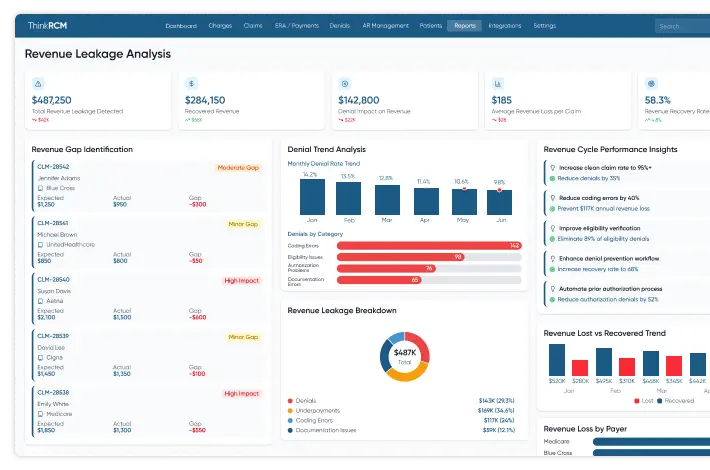
Find and fix revenue leakage points
Did you know, around 90% of the revenue leakage in healthcare can be prevented? Get your analysis and prevent loss.








Clients Testimonials
Why Healthcare Providers Trust Our Revenue Leakage Prevention Service
Healthcare organizations rely on our expertise to identify revenue gaps, reduce claim denials, and improve reimbursement accuracy across their revenue cycle operations.
Cost & Timelines
Key Factors That Impact Revenue Integrity and Reimbursement Performance
Evaluating these factors helps strengthen revenue integrity and billing efficiency.
Practice Size & Patient Volume
Provider count and patient volume shape billing workflows and ensure efficient claim processing.
Healthcare Specialty
Specialty-specific billing requirements help improve coding accuracy and reimbursement outcomes.
Claim Processing Efficiency
Efficient claim processing ensures timely submissions, reduces errors, and minimizes denials that contribute to revenue leakage.
EHR & Billing System Integration
Seamless integration with EHR and billing systems improves claim accuracy and reduces administrative work.
HIPAA & Payer Compliance
Compliance with HIPAA and payer guidelines helps reduce claim rejections and billing risks.
Accurate Patient Data & Documentation
Accurate patient information and documentation help prevent billing errors, reduce claim rejections, and support compliant reimbursements.
RCM Service Scope
Defining the right RCM scope ensures comprehensive billing support and maximized reimbursement opportunities.
Current Billing Workflow
Evaluating existing workflows helps identify inefficiencies and improve overall revenue cycle performance.
We deliver healthcare software in the following timeframes
1 Week
Medical software project starts within 1 week
2-4 Months
MVP release
Every 2-4 Weeks
New healthcare software versions

Engagement models
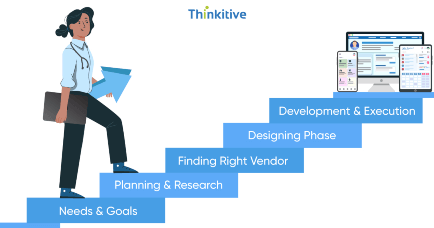
Choose the Right Engagement Model for Revenue Leakage Prevention & Denial Management
Flexible engagement models designed to support denial management, prevent revenue leakage, and improve reimbursement outcomes.
Full-Service RCM Management
End-to-end revenue cycle support including denial management, revenue leakage prevention, claim processing, and reimbursement optimization to strengthen revenue integrity across your billing lifecycle.
Dedicated Revenue Cycle Team
A specialized team of RCM experts working alongside your organization to monitor claim performance, prevent denials, identify revenue leakage, and optimize reimbursement outcomes.
SAVE
EXTRA 20%
Case studies
Revenue Cycle Management Services Case Studies & Success Stories
Why Healthcare Organizations Trust Us
98%
Clean Claim
Rate
30%
Average Revenue
Increase
100%
HIPAA-Compliant
& Secure
100%
Certified
Coders
24/7
Support
No
Long Term
Contracts

Ready to Recover & Prevent the Losses from Revenue Leakage?
With denial management and revenue recovery services, improve your practice’s financial health.
Frequently Asked Questions
Get answers to all your questions
Still have questions?
Everything About Healthcare Software Development
Healthcare Software Development Blogs

Custom Healthcare Software for Population Health Management

The Role of Healthcare Software Developers in Digital Transformation
Benefits of Custom Healthcare Software for Small Practices & Clinics