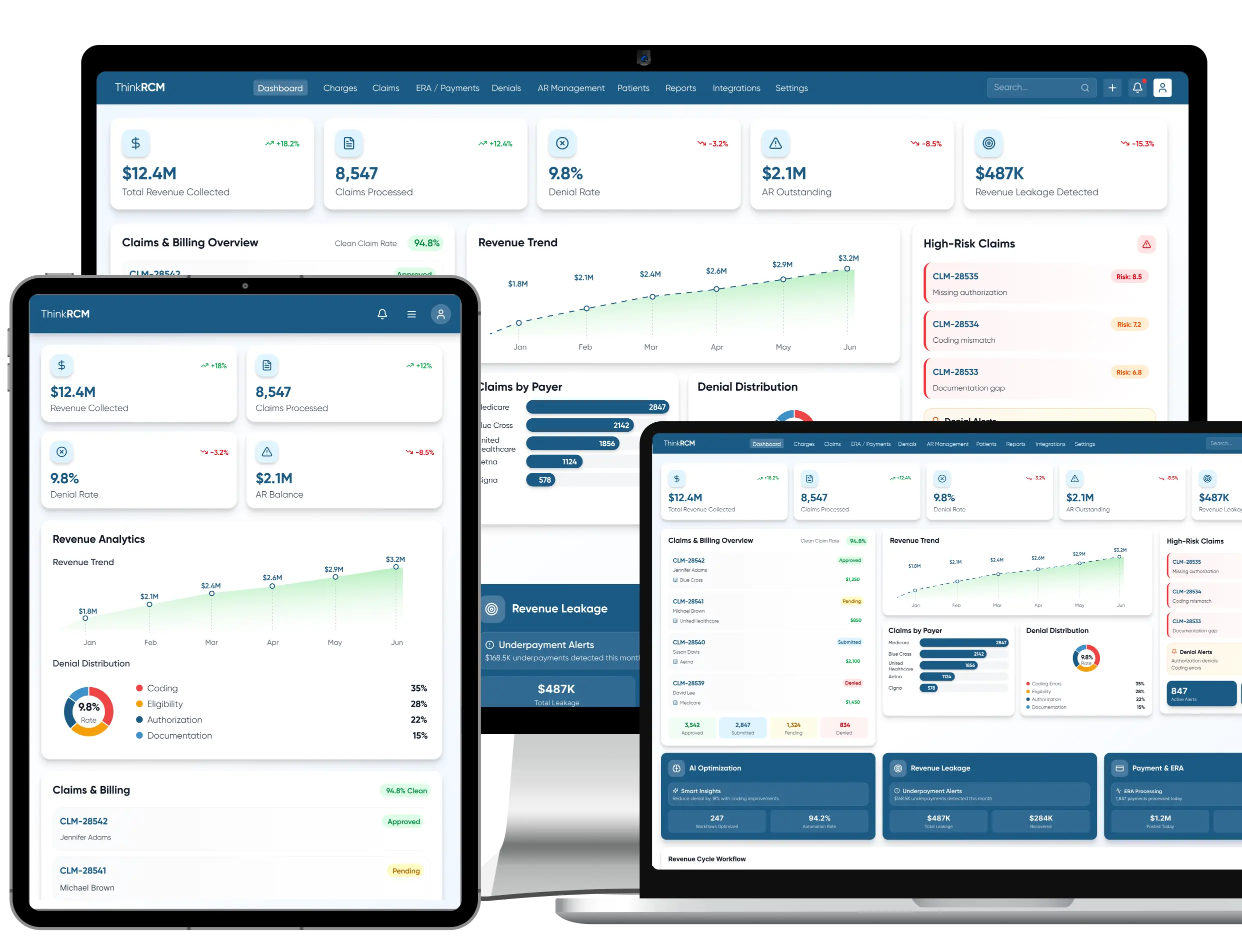
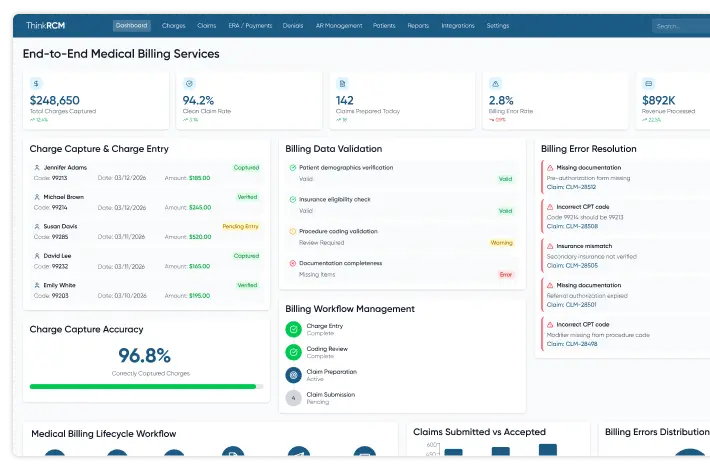
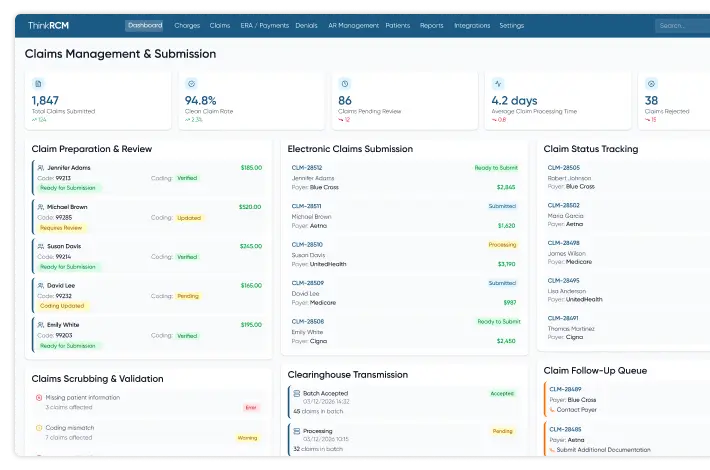
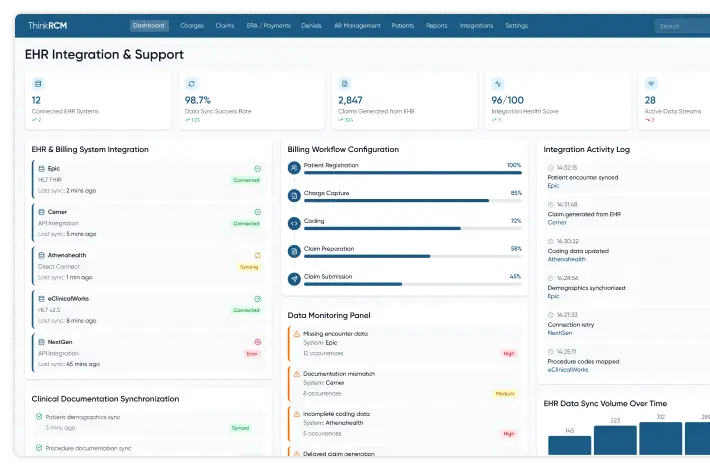
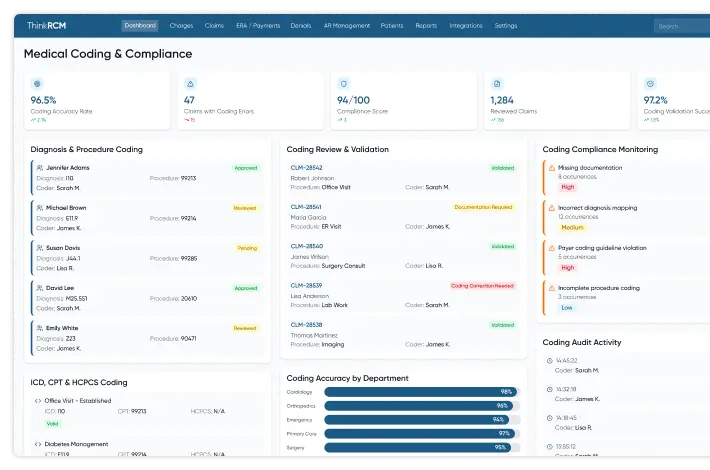
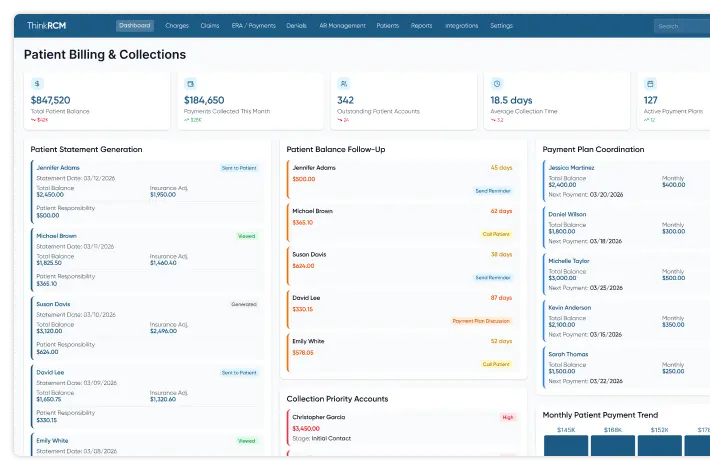
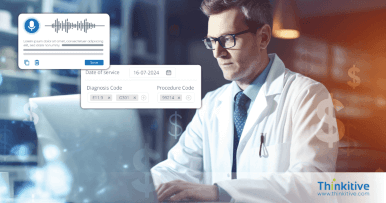
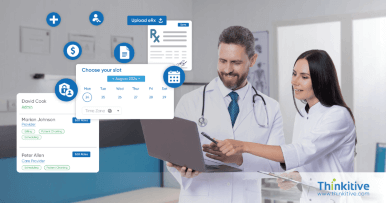
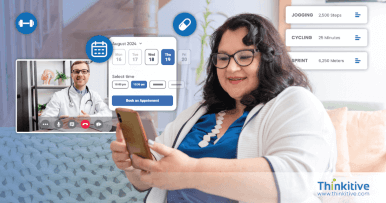
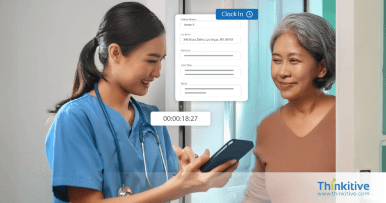
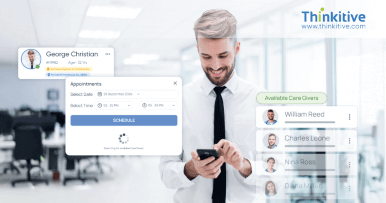
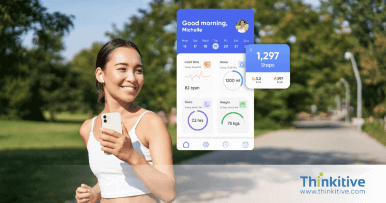
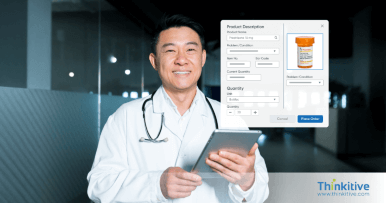
Comprehensive RCM Services That Streamline Billing & Accelerate Reimbursements
Structured RCM processes that help reduce claim denials, improve clean claim rates, and accelerate reimbursements across the healthcare billing lifecycle.

All-in-one RCM services to improve cash flow
Streamline billing operations and accelerate healthcare reimbursements.








Clients Testimonials
What Healthcare Providers Say About Our RCM Services
Real experiences from healthcare providers using our RCM services.
Cost & Timelines
Key Factors That Determine the Success of Your Revenue Cycle
Mastering these factors optimizes workflows, reduces denials, and boosts revenue.
Practice Size & Patient Volume
Provider count and patient volume shape billing workflows and ensure efficient claim processing.
Healthcare Specialty
Specialty-specific billing requirements help improve coding accuracy and reimbursement outcomes.
Claim Volume
Managing claim volume efficiently ensures faster submissions and more consistent reimbursement cycles.
EHR & Billing System Integration
Seamless integration with EHR and billing systems improves claim accuracy and reduces administrative work.
HIPAA & Payer Compliance
Compliance with HIPAA and payer guidelines helps reduce claim rejections and billing risks.
Data Security & Patient Information Protection
Strong security practices safeguard patient data and support compliant billing operations.
RCM Service Scope
Defining the right RCM scope ensures comprehensive billing support and maximized reimbursement opportunities.
Current Billing Workflow
Evaluating existing workflows helps identify inefficiencies and improve overall revenue cycle performance.
We deliver healthcare software in the following timeframes
1 Week
Medical software project starts within 1 week
2-4 Months
MVP release
Every 2-4 Weeks
New healthcare software versions

Engagement models
Choose the Right Engagement Model for Your RCM Needs
Flexible engagement models designed to support your revenue cycle operations, billing workflows, and reimbursement goals.
Full-Service RCM Management
End-to-end revenue cycle management support covering billing, coding, claims processing, payment posting, denial management, and accounts receivable follow-ups to streamline the entire billing lifecycle.
Dedicated Revenue Cycle Team
A dedicated team of RCM specialists working as an extension of your organization to manage billing operations, monitor claim performance, resolve denials, and support ongoing revenue cycle optimization.
SAVE
EXTRA 20%
Case studies
Revenue Cycle Management Services Case Studies & Success Stories
Why Healthcare Organizations Trust Us
98%
Clean Claim
Rate
30%
Average Revenue
Increase
100%
HIPAA-Compliant
& Secure
100%
Certified
Coders
24/7
Support
No
Long Term
Contracts

Ready to Strengthen Your Healthcare Revenue Cycle?
Strengthen billing operations and accelerate reimbursements with expert RCM support.
Frequently Asked Questions
Get answers to all your questions
Still have questions?
Comprehensive RCM services refer to the end-to-end management of financial and administrative processes involved in healthcare reimbursement. These services support the entire revenue cycle, from patient registration and insurance eligibility verification services to medical coding, claims submission, payment posting, and collections.
Through comprehensive revenue cycle management, healthcare organizations can streamline billing workflows, improve reimbursement accuracy, and reduce administrative burden. Full service revenue cycle management ensures that every stage of the billing lifecycle is managed efficiently to support consistent revenue flow and operational stability.
Comprehensive revenue cycle management services typically include a wide range of billing and financial operations that support healthcare reimbursement. These services may involve insurance eligibility verification services, end-to-end medical billing services, healthcare claims management services, and ICD-10 medical coding services.
Additional components often include payment posting and reconciliation services, denial management and appeals services, medical AR management services, and patient billing and collections services. Together, these processes ensure that healthcare providers can maintain accurate billing operations and improve revenue cycle performance.
End-to-end medical billing services help healthcare providers manage the complete billing lifecycle, ensuring claims are prepared, submitted, and followed up accurately. These services include claim preparation, claim scrubbing services, coding validation, and payer communication to improve the likelihood of successful reimbursements.
When integrated within comprehensive revenue cycle management services, these processes support clean claim rate optimization, reduce claim rejections, and accelerate payment timelines. This structured billing workflow helps healthcare providers improve revenue collection and maintain consistent financial performance.
Effective healthcare claims management services play a critical role in ensuring claims are submitted accurately and processed efficiently by insurance payers. Proper claims management involves verifying claim details, performing claim scrubbing services, and submitting claims in accordance with payer requirements.
When supported by comprehensive RCM services, claims management helps improve first-pass claim acceptance rates and supports clean claim rate optimization. Accurate claims submission reduces rework, prevents delays, and ultimately contributes to higher reimbursement rates for healthcare providers.
EHR billing integration services enable seamless communication between electronic health record systems and billing platforms. This integration ensures that clinical documentation, diagnosis codes, and treatment details are automatically aligned with billing workflows.
Within comprehensive revenue cycle management, EHR integration improves data accuracy, reduces manual data entry, and ensures billing processes remain consistent with clinical documentation. This streamlined workflow helps healthcare organizations maintain efficient revenue cycle operations and reduce administrative errors.
Medical coding is essential for translating clinical documentation into standardized billing codes used for claim submission. Accurate coding through ICD-10 medical coding services ensures diagnoses and procedures are correctly represented for insurance reimbursement.
As part of comprehensive revenue cycle management services, coding also supports medical coding compliance services and healthcare billing compliance services, helping providers maintain regulatory compliance while improving claim accuracy and reimbursement outcomes.
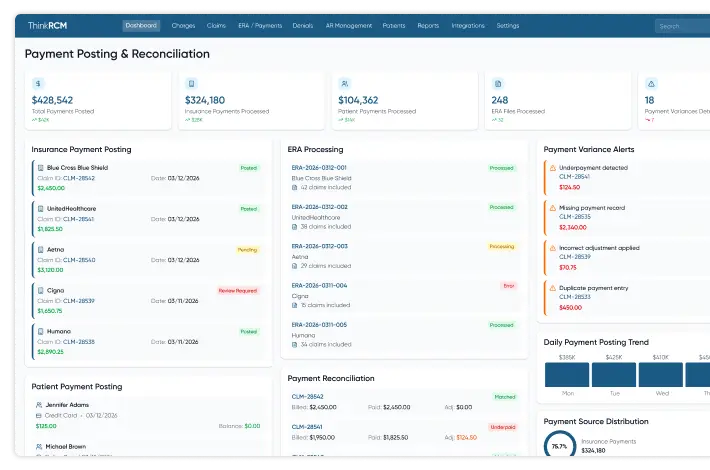
Payment posting and reconciliation services ensure that payments received from insurance companies and patients are accurately recorded within the billing system. These services involve reviewing remittance details, posting payments to appropriate accounts, and identifying discrepancies.
Through medical payment posting services, healthcare providers gain better visibility into payment status and financial performance. Within comprehensive revenue cycle management, this process helps maintain accurate financial records and ensures billing data reflects actual reimbursements received.
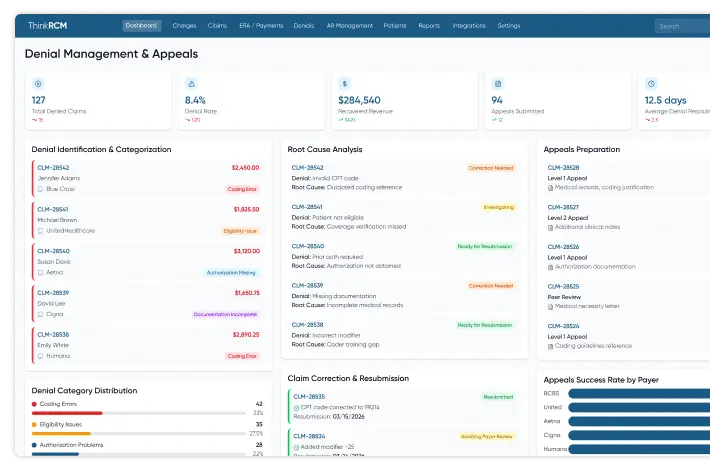
Denial management involves identifying, analyzing, and resolving claims that have been rejected or denied by insurance payers. Denial management and appeals services help healthcare organizations review denial reasons, correct claim errors, and resubmit claims with the necessary documentation.
With structured medical billing denial appeals services, providers can recover revenue that may otherwise be lost due to claim rejections. Within comprehensive RCM services, denial management also helps identify recurring billing issues and improve future claim acceptance rates.
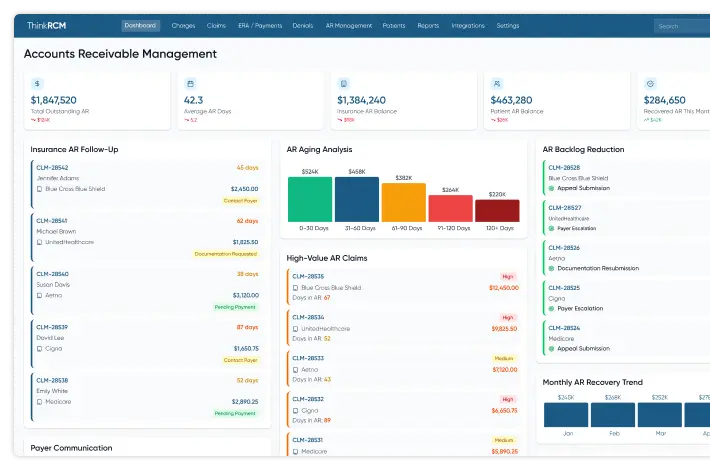
Medical AR management services focus on tracking outstanding claims and ensuring timely follow-up with insurance payers. By reviewing aging reports and resolving unpaid claims, healthcare organizations can improve revenue recovery and reduce delays in reimbursement.
As part of comprehensive revenue cycle management, effective AR processes help support accounts receivable days reduction healthcare, allowing providers to maintain healthier cash flow and better financial stability.
Claim denials in medical billing often occur due to incomplete patient information, coding inaccuracies, missing documentation, or insurance eligibility issues. Errors in claim preparation or failure to meet payer requirements can also lead to rejections.
Through comprehensive revenue cycle management services, processes such as insurance eligibility verification services, claim scrubbing services, and coding validation help minimize these issues and improve overall claim acceptance rates.
Patient billing and collections services play an important role in ensuring patient financial responsibility is managed effectively. These services involve generating patient statements, processing payments, and following up on outstanding balances.
Within comprehensive revenue cycle management, effective patient billing helps healthcare providers recover outstanding balances while maintaining clear communication with patients regarding their financial obligations.
Administrative tasks related to billing, coding, and claims management can be time-consuming for healthcare organizations. Comprehensive RCM services help manage these processes through specialized teams and structured workflows.
By handling billing operations, coding, AR follow-ups, and denial management, comprehensive revenue cycle management services allow healthcare staff to focus more on patient care rather than administrative billing tasks.
End-to-end comprehensive revenue cycle management provides healthcare organizations with detailed insights into billing performance, claim status, and payment trends. Structured reporting and monitoring allow providers to track financial metrics more effectively.
By integrating services such as payment posting and reconciliation services, medical AR management services, and claims tracking, healthcare organizations can maintain greater financial transparency and make informed revenue cycle decisions.
Yes, comprehensive revenue cycle management services are designed to support a wide range of healthcare organizations, including multi-specialty clinics and physician groups. Different specialties often have unique billing workflows and payer requirements.
Through structured medical billing for physician groups, specialized coding processes, and payer-specific claims management, comprehensive RCM services can adapt to the operational needs of multi-specialty healthcare practices.
Healthcare providers often outsource comprehensive revenue cycle management services to improve billing efficiency, reduce claim denials, and optimize revenue performance. Managing the full revenue cycle internally can require significant administrative resources and specialized expertise.
Outsourcing full service revenue cycle management allows providers to access experienced billing professionals, advanced billing tools, and structured workflows that support improved reimbursement timelines and stronger financial performance.
Everything About Healthcare Software Development
Healthcare Software Development Blogs

Custom Healthcare Software for Population Health Management

The Role of Healthcare Software Developers in Digital Transformation
Benefits of Custom Healthcare Software for Small Practices & Clinics