Healthcare Data Migration: Moving Patient Records Between Systems Safely

Healthcare is becoming more personalized, and so is healthcare delivery!
This transition has been on the rise as many healthcare practices are actively adopting value-based care practices. And in this quest, many healthcare practices are actively choosing to build their own healthcare systems.
The inefficiencies that are being caused by the healthcare system have forced many practices to move away from traditional off-the-shelf healthcare systems. In this quest to upgrade their healthcare systems, many practices are taking the risk of EHR data migration.
You see, if you go by definition, healthcare data migration is nothing but the process of moving files from one system to another. Sounds simple, right?.
Well, it’s actually not that simple. If it had been, then it wouldn’t have been the riskiest phase in healthcare system upgrades.
Having said that, most practices are adopting EHR data migration because, as they shift to newer systems, they want to maintain a single source of truth for the practice.
On that note, in this blog, let’s uncover the intricacies of healthcare data migration and also discuss some of the EHR migration risks and best practices to overcome them.
So, without further ado, let’s get started!
What is Healthcare Data Migration?
Before getting into the details of the healthcare data migration process, let’s first get the basics cleared, starting with the definition.
So, data migration in healthcare can be defined as the process of securely and structurally transferring sensitive patient and clinical information from one system, format, and storage location to another.
While the definition sounds simple, the devil that hides in the details is ensuring clinical continuity in the process of transferring. That is why this is referred to as the riskiest phase in healthcare IT upgrades.
Furthermore, when understanding healthcare data migration, knowing the difference between migration, mapping, and data exchange is also important. On that note, refer to the table for clarity:
| Aspect | Data Migration | Data Mapping | Data Exchange |
| Definition | Transferring healthcare data from one system to another | Aligning data fields between source and target systems | Sharing data between systems in real time or on demand |
| Purpose | Move complete patient records during system changes | Ensure data accuracy and consistency | Enable seamless access to patient information across systems |
| Nature | One-time or phased process | Supporting step within migration/integration | Continuous and ongoing process |
| Scope | Entire datasets (EHRs, billing, clinical data) | Individual data elements (fields, formats, codes) | Selected data (labs, prescriptions, summaries) |
| Example | Moving data from a legacy EHR to a new system | Mapping “BP” to “Blood Pressure” field | Sending lab results from lab system to EHR |
- Role in EHR Replacement, System Upgrades, & Consolidation
If you are already running a practice and looking to replace or upgrade your EHR system, then you need patient data migration to bring your old data into your new system. Data migration plays a foundational role that helps you restructure your IT systems more effectively.
During EHR replacement, you need to ensure complete patient histories are transferred without loss. Moreover, the clinical workflows must continue and align with your practice without disrupting other processes.
However, for upgrades, you need data migration to maintain data integrity across the new architecture and improve performance. It basically allows practice upgrades without losing legacy data value.
Achieving true interoperability has become crucial for care coordination and continuity of care. With accurate medical data migration, data can be structured, standardized, and consistent across care settings, allowing for seamless exchange.
Furthermore, with data migration complete, accurate patient records can be accessed. This way, you won’t lose data and improve care delivery while ensuring patient safety and desired outcomes.
The Healthcare Data Migration Process: A Structured Framework
Now that you have a brief idea about healthcare data migration, let’s try to learn about the healthcare data migration process and the intricacies in it, so that you can safely move the data from one system to another.
The migration process can be divided into four phases. Let’s have a look at what those phases are and what happens in each phase. Refer to the table below for a better understanding:
| Phase | Key Activities | Objective | Key Considerations |
| Phase 1: Pre-Migration Discovery | Data audit, identify dark data, detect orphan records, assess data quality | Understand the current data landscape and risks | Data completeness, duplication, compliance gaps |
| Phase 2: Extraction & Scoping | Extract data from source systems, define what to migrate vs archive | Reduce migration load and focus on relevant data | Business requirements, regulatory retention policies |
| Phase 3: Transformation Bridge | Data mapping, standardization, format conversion, validation rules | Ensure data is usable and compatible in the target system | Terminology standards (ICD, SNOMED, LOINC), data consistency |
| Phase 4: Execution & Cutover | Data transfer, system switch (Big Bang or phased), go-live support | Move data safely and transition operations smoothly | Downtime planning, rollback strategy, user readiness |
These four phases are basically the blueprint of an end-to-end healthcare data migration process. However, data migration can only be considered a success when data integration is intact with no loss or corruption. Along with that, the data is secure and compliant with the necessary regulations and compliances.
The data migrated from other systems should not disrupt the patient care activities and ensure clinical continuity. Last but not least, the data should be structured for future exchange.
Migration Strategies for Safe Data Transition
You might follow all four phases of data migration by the book, but the real-world setting is often different than what it appears. That is why there are strategies that allow you to ensure the safety of your data and fill the gaps that might be left during the process.
On top of that, choosing the right migration strategy is also important. That way, data safety would not be compromised, and clinical continuity would be ensured with minimal disruption.
- Big Bang Vs Phased Migration
You might be aware of these terminologies. Here is a table to help you choose the right strategy for your practice:
| Approach | Description | Advantages | Risks / Limitations |
| Big Bang Migration | All data is migrated at once, followed by immediate system switch | Faster transition, no need to maintain two systems | High risk of downtime, difficult rollback, potential clinical disruption |
| Phased Migration | Data is migrated in stages (by department, location, or data type) | Lower risk, easier validation, minimal disruption | Longer timelines, requires coordination across phases |
TIP: While most practices prefer phased migration to reduce clinical and operational risks. You can choose Big Bang, depending on your needs, after consulting your vendor.
- Parallel Systems Vs Full Cutover
During replacements, you might replace your older system with a completely new one or gradually replace your older system with a new one. Now, both these approaches have their advantages and disadvantages. Let’s have a look at them briefly to help you make a considerate decision:
| Approach | Description | Advantages | Risks / Limitations |
| Parallel Systems | Old and new systems run simultaneously for a period | Safer transition, real-time comparison, easier error detection | Higher cost, data synchronization challenges |
| Full Cutover | Old system is completely replaced by the new system at go-live | Simpler operations post-migration, no duplication | High dependency on migration accuracy, limited fallback options |
TIP: Parallel systems are something that you should consider if you are working in high-risk environments to ensure patient data safety.
- Full Vs Selective Migration
Some organizations simply want to transfer the entire database to new systems, and some want to selectively migrate. Though this choice completely depends on your needs, here is a quick breakdown of both the migration strategies:
| Approach | Description | Advantages | Risks / Limitations |
| Full Migration | Entire dataset is transferred to the new system | Complete data availability, no dependency on legacy systems | Higher cost, longer migration time, risk of moving redundant data |
| Selective Migration | Only critical or recent data is migrated; older data is archived | Faster, cost-effective, improved system performance | Limited historical data access, may require legacy system reference |
TIP: Given the nature of data, many organizations adopt a hybrid approach, where they migrate active patient data and archive the historical records.
How to Choose the Right Migration Strategy?
Depending on your system needs and requirements, the right strategy for your practice might differ. There are multiple factors that you need to consider before making a decision. On that note, here are some of the factors that you need to consider:
- Risk Tolerance: If you tolerate risk with your data, then the phased and parallel approach is best suited. However, with high tolerance, a big bang with a full cutover approach can give you a completely new system.
- Data Volume & Complexity: The complexity of your clinical and administrative data, along with its volume, can also influence your strategy. For instance, large and complex databases often choose a phased and selective migration strategy, whereas smaller datasets go for a big bang.
- Clinical Impact: If your practice is currently heavily dependent on your system and its data, then for a high dependency system, minimum downtime is something that you should consider. If not, then a flexible approach can be used to enhance your system.
The safest healthcare data migration approach is that which balances risk, speed, and data criticality, while prioritizing patient safety and maintaining data integrity.
Identifying EHR Migration Risks & Best Practices
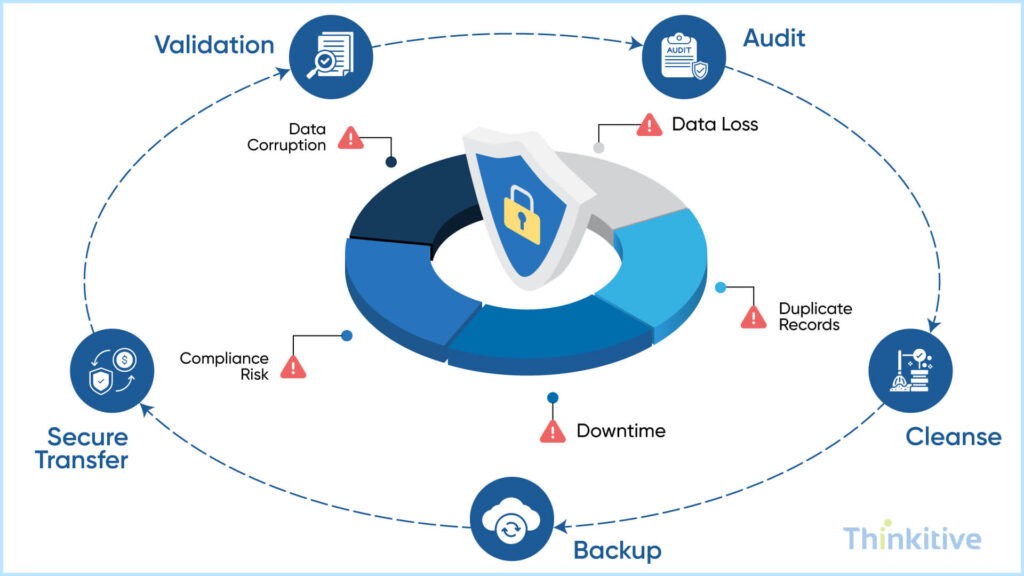
The healthcare data migration process is a high-risk process, but do you know why?
You see, the data you deal with is sensitive; moreover, it is not simple or structured; it is more complex than it appears on the surface. On top of that, the clinical importance of that data is that it can determine the course of care journey of the patient.
That is why it is important to identify EHR data migration risks before moving ahead. On that note, here is how you can identify EHR migration risks and the best practices that you can use for a safe and successful transition.
- The Dirty Data Trap
Poor data quality is still one of the most common challenges in patient data migration, and it carries the most risk as well. Poor data quality is often the result of duplicate patient records, incomplete or outdated information, data stored in inconsistent formats, etc. Now, migrating this data can lead to errors in new systems, affecting both clinical and administrative processes.
The best way to overcome this is to perform thorough data cleansing and normalize data before migration. Using AI-driven techniques can be a great help in that.
- Downtime & Operational Disruptions Risks
During migration, there is a chance that your system can experience downtime, which can have a devastating impact on patient care. Some of the aftermath of downtime can be delayed access to patient records or manual data entry, increasing the burden on staff or even interrupting workflows.
One of the healthcare data migration best practices that has been adopted by many organizations has been planning migration before, and especially doing it during low-activity hours. Another way can be by using a phased or parallel approach to minimize downtime.
- Security & Compliance Risks (HIPAA/GDPR)
Given the sensitive nature of the data, during migration, there is a chance that you might compromise the security of that data. Some of these can result in data breaches or unauthorized access, and at times even non-compliance. This can lead to severe penalties and reputation damage as well.
So, the best way to ensure compliance and maintain security is by implementing end-to-end encryption along with role-based access controls. On top of that, to be all over the process, you can maintain detailed audit logs and compliance checks.
- Data Loss & Corruption Risks
Improper migration can lead to missing patient records, corrupted clinical data, and even misaligned data fields. This can have a direct impact on patient safety and the accuracy of the diagnosis and care.
The best practice to deal with this is to conduct data reconciliation and validation checks for every process. Along with that, maintain secure backups before executions, just in case.
Best Practices to Mitigate Migration Failure
Here are some of the best practices that you can adopt to mitigate the risk of failure during EHR data migration:
- Conducting a comprehensive pre-migration audit to know the intricacies of data.
- Before starting, define a clear data migration strategy and scope, so you know exactly what you have to do.
- Use standardized data formats and terminologies.
- Involve clinical stakeholders in validation.
- Perform end-to-end testing and post-migration monitoring to ensure the data migration process is a success.
Furthermore, you can also use AI to reduce migration risk. For example, many organizations are using AI to detect data anomalies and inconsistencies early on. In fact, it has become a best-case scenario to use AI to identify duplicate or mismatched patient records and automate data quality checks and validation.
How to Migrate Patient Data Between Healthcare Systems Safely
If you’ve made it this far and read or just scanned everything in between, then I guess you are ready to know how to migrate patient data between healthcare systems safely.
Validation Protocols
First things first, you need to know the data validation protocols that you need to follow in healthcare data migration.
- Installation Qualification (IQ): This validation protocol verifies that the migration environment, tools, and infrastructure are set up as they should be.
- Operational Qualification (OQ): This validation is used to ensure that the migration process functions as intended and as per the defined conditions.
- Performance Qualification (PQ): This validation confirms that the system performs reliably in real-world scenarios with actual patient data.
These protocols ensure technical accuracy and system reliability before you deploy. One of the best, tried, and tested ways to mitigate risk during migration.
- Clinician Verification Checkpoints
In the data migration process, verifying the process from a technical aspect is important, but clinical validation is also critical, which many skip. In this, clinicians must verify the accuracy of patient history, medications, and diagnoses. Moreover, the migrated data must also be cross-checked with critical data points like allergies, lab results, treatment plans, etc.
- Data Lineage & Audit Tracking
One of the best ways to mitigate risks during data migration is by maintaining fully traceable data links. Meaning, you should know from where the data originates and how it was transformed. The logs of every transformation must be maintained at every step. This is to ensure transparency, accountability, and compliance readiness.
Safe patient data migration does not have a concrete way; in fact, it is achieved through a combination of technical validation, clinical oversight, and continuous monitoring of the process. When all these aspects come together, it ensures data integrity, regulatory compliance, and uninterrupted patient care.
Post-Migration: Legacy Decommissioning & Optimization
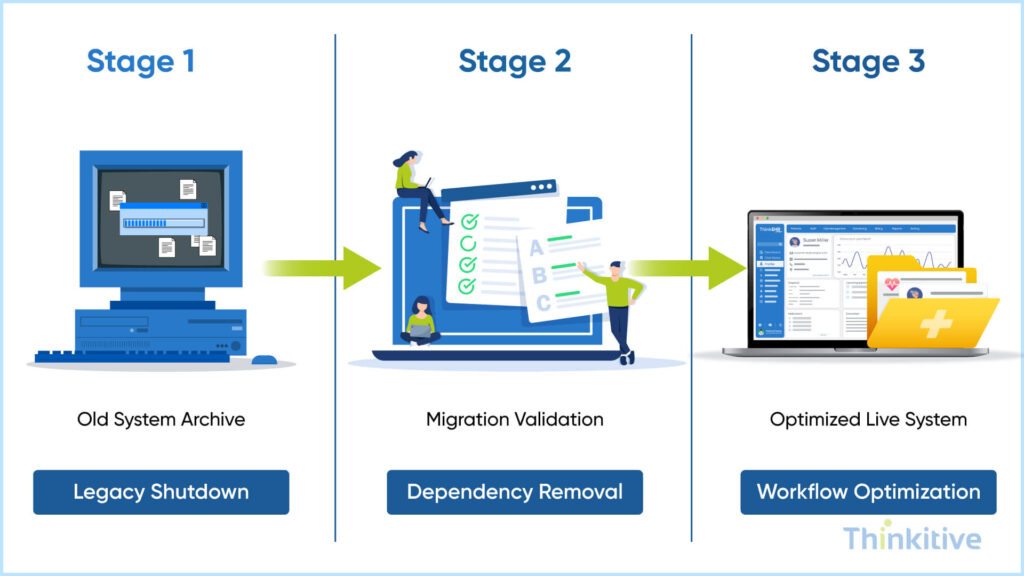
Once you go live, the data migration doesn’t complete. There are certain post-migration activities that you need to do to ensure that data remains accurate, accessible, and optimized, while you are safely retiring legacy systems without losing compliance or historical value.
And this becomes the very first activity that you need to do after you go-live. Archive all the historical data based on regulatory retention requirements. During this, ensure the security of the storage of data and gradually decommission outdated systems to reduce maintenance costs.
Once that is done, go through all the audits thoroughly. This way, you can reconcile record counts between source and target systems. Verify the accuracy of the data being migrated. This is one of the best ways to validate your migration success. Also, it helps you identify and resolve any discrepancies.
While you’re at it, also ensure that the migrated data is usable and is structurally correct for clinical workflows. Validate its searchability and reporting capabilities and confirm that it is seamlessly accessible for healthcare providers.
And the last section, as usual, is to monitor the performance of the system with respect to that of the data and support long-term stability and adoption.
Conclusion: A Strategic Foundation for Interoperability
If you have read this article, then we have hardly talked about connected healthcare systems, right?
Well, because data migration mainly deals with transferring data from one system to another. However, safe data migration is the first step towards a connected healthcare system. You see, only when the data is accessible, usable, and correctly aligned can it be used by healthcare practices for care delivery.
That is why data migration aspects must not be ignored. Plan, validate, and govern the data migration process for a successful EHR data migration venture. And yeah, almost forgot, use AI wherever you can, it can not only save you time, but also help you in processes that would be too complex to do manually.
Having said that, given the rising demand for EHR integration, this is the right time for you to make your system a part of the connected healthcare ecosystem. On that note, book your first call to discuss a future-proof healthcare data migration strategy for your system.
Frequently Asked Questions
EHR data migration refers to the process of transferring patient records from one system to another, typically during system replacement or upgrades. In contrast, EHR integration focuses on enabling continuous data exchange between systems without moving all data. While healthcare data migration is usually a one-time or phased activity, integration supports ongoing interoperability across healthcare platforms.
The timeline for healthcare data migration depends on factors like data volume, system complexity, and migration strategy. A small-scale medical data migration may take a few weeks, while large hospital systems can take several months. A well-planned healthcare data migration process with phased execution and proper validation helps reduce delays and ensures safer outcomes.
Common EHR migration risks include data loss, corruption, poor data quality (“dirty data”), downtime, and security vulnerabilities. Following EHR migration risks and best practices—such as data cleansing, validation testing, secure data transfer, and phased migration—helps minimize these risks and ensures a safe transition.
Ensuring data integrity in patient data migration involves multiple validation steps, including data mapping, record reconciliation, and clinical verification. Using structured healthcare data migration processes, along with testing protocols and audit trails, ensures that migrated data remains accurate, complete, and consistent across systems.
AI plays a critical role in healthcare data migration by identifying duplicate or mismatched patient records across systems. During medical data migration, AI-driven algorithms analyze patterns, demographics, and clinical data to detect duplicates more accurately, improving data quality and reducing manual effort in patient data migration.
Not all data needs to be migrated. In many healthcare data migration projects, organizations choose selective migration—transferring only active or recent patient data while archiving older records. The decision depends on regulatory requirements, clinical needs, and system performance considerations within the overall healthcare data migration process.
The healthcare data migration process can impact daily operations through temporary downtime, workflow adjustments, or limited system access during transition. However, careful planning—such as phased migration, parallel systems, and staff training—helps minimize disruptions and ensures continuity in patient care.
Key healthcare data migration best practices for security include encrypting data in transit and at rest, implementing role-based access controls, maintaining audit logs, and ensuring compliance with regulations like HIPAA. Secure handling of patient data migration is essential to protect sensitive health information and avoid breaches.




