EHR Integration ROI: How to Measure the Business Impact

Electronic Health Records have made record-keeping easier than ever before. Though it has solved one problem, another aspect was left open for inefficiencies to slip in.
This is one of the core reasons why the demands of EHR EMR integrations seem to be as high as ever.
But let’s first try to understand why integration has become a core part of the modern healthcare landscape. You see, physicians spend more than 49% of their time on EHR or desk work, according to the Annals of Internal Medicine. Also, in the same research, it was found that for every 1 hour a physician spends on patient care, 2 hours are spent on EHR tasks.
This exactly shows the need for your EHR system to be a part of the connected healthcare ecosystem. It not only fosters better care but also helps you save costs massively.
And given that integration projects can be costly, many practices simply choose to ignore the EHR integration benefits that majorly involve cost saving, while enabling scalability, interoperability readiness, a holistic care approach, and better patient experience.
To give you an example, a study by HIMSS reported that with interoperability, administrative costs can be reduced up to 15%.
So, when someone asks you about the benefits of integration, rather than just telling them, give them a blueprint of EHR integration ROI and EHR efficiency metrics that the practices can unlock.
However, here you might ask, ‘How to measure EHR integration ROI?’
Well, try to understand the intricacies of EHR integration ROI calculation, so that you can have a brief idea about the costs involved in it and the returns you can achieve through it.
On that note, let’s unlock the ROI of healthcare technology and how to measure its business impact on your EHR EMR integration projects.
So, without further ado, let’s dive deep!
How to Measure EHR Integration ROI
Everything comes down to money after all. In the context of EHR integration, the project cost can vary significantly depending on your needs and complexity. However, even if you have a vague idea about your integration projects, then EHR integration ROI calculation becomes quite easier.
On that note, here is a rough way in which you can measure your EHR integration ROI.
First things first, before beginning the process, you must know where you stand and what to improve. For that, first establish a baseline. In this record, the current performance of your system. Some of the KPIs that you can measure are:
- Staff time
- Claims denial rates
- Patient throughput
- Documentation delays
- Avg. errors in a single patient record
While this list can be quite lengthy, the above are some of the key pointers that you have to measure. Having said that, once you’re done with recording the current performance, what you need to do next is define clear KPIs.
Remember, these KPIs should be measurable indicators, and they should be spread across different facets of your practice. For instance, on the operations side, your KPIs can be – time saved, workflow speed, etc. Whereas, on the financial aspect, it can be revenue cycle efficiency, reduced denials, first claims pass, etc. And the most important, for clinical aspects, your KPIs can be care coordination, error reduction, time to care, etc.
Once you’ve defined the KPIs, discuss these with your vendor and tell them your expectations about the improvement you want to achieve after integration.
However, just defining these KPIs is not enough. You have to track the performance of your system and integration continuously. In fact, you can use the dashboards and reporting tools within your EHRs or analytics systems to monitor the changes in real-time.
Once your performance monitoring mechanisms are in place, give it some time and then compare the improvements by comparing the integration metrics you record prior to integration with the post-integration results. This will clearly show you if you have gained anything from this project.
Last but not least, ensure that all your ROI metrics support standards like CMS’s quality measures and programs such as MIPS under MACRA. This way, your ROI is tied to reimbursements and regulatory success. Covering almost every aspect of your EHR integration project.
Quantifying Operational EHR Efficiency Metrics

The ROI of healthcare technology is quite different from that of other industries. While other industries clearly show the ROI metrics, in healthcare, especially with EHR integration, the quantifying results are often highlighted in the operations, which can directly or indirectly impact the EHR integration ROI.
One of the best examples of this can be seen in improved staff productivity. You see, research by McKinsey & Company found that integrated systems can improve staff productivity by 20-30%.
In short, what I mean to say here is that EHR integration improves your day-to-day operations and staff efficiency. And the ROI of your EHR integration can be proven, showing less time wasted, faster workflows, or more output with the same resources. On that note, here are some quantifiable operational metrics that you can use to measure your EHR integration ROI.
- Reduced Manual Work: Track how much time is saved by eliminating duplicate data entries and other manual administrative tasks across the system. In fact, a study suggested that EHR integration can roughly reduce documentation burden by 25% to 35%, according to Research Gate.
- Improve Workflow Speed: Another measurable metric you can use to measure your ROI is by measuring how fast your clinical processes have become. This includes tasks like patient intake, documentation, and billing.
- Measure Across Departments: EHR integration impacts every department across your practice. So, when measuring its ROI or impact, don’t just limit it to one department or one aspect of your clinical. Measure performance across systems.
- Assess Automation Impact: With EHR integration, certain processes in your system will be automated. Now, by measuring the impact of such automated workflows like data syncing, order entry, reporting, etc., it reduces delays, errors, and manual efforts across systems.
Financial Impact & EHR Integration ROI Calculation
As I said earlier, everything comes down to cost. So, let’s try to translate the operational improvements that we have discussed earlier into clear financial outcomes. You know, just to give you an idea about the financial benefit you can enjoy with EHR integration.
- Improved Revenue Cycle Performance: Access to data in real-time is the critical factor that plays a huge role in improving your revenue cycle performance. With accuracy in data and your system acting as a single source of truth, claims denial rates can be reduced. The aftermath of this can be seen in the billing cycle, speeding it up and accelerating reimbursements, which directly increases cash flow in your practice.
- Reduce Unnecessary Costs: By eliminating duplicate tests, repeated manual data entry processes, and inefficient workflows, your practice can save significantly.
- Optimize Resources: By shifting the focus of your resources from administrative workload to clinical care, you can actually put your staff to meaningful use. You see, by reallocating staff from admin-heavy tasks to higher-value activities that can care for delivery, you can give more output without increasing your staff numbers.
ROI Formula
When it comes to cost, it is all about cost. On that note, here is a simple formula that can help you calculate your EHR integration ROI:
ROI = (Total Benefits – Total Costs)/Total Costs
Furthermore, here is a simple flowchart that can help you understand how integration impacts your finances in a step-by-step manner.
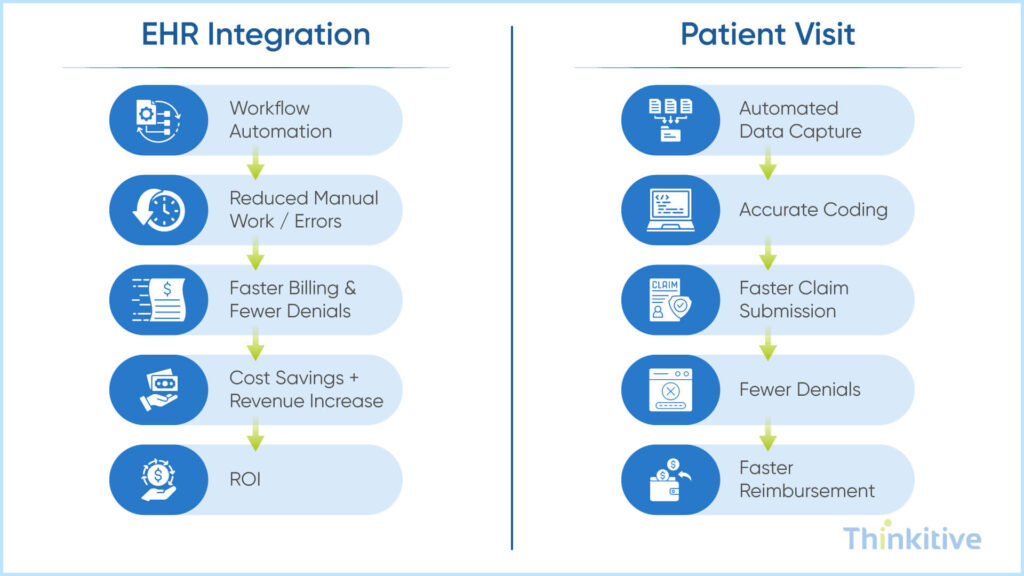
Also, here is a simplified table that shows financial and operational improvement from our latest EHR integration project:
| Metric | Before Integration | After Integration |
| Claim Denial Rate | 18% | 10% |
| Billing Cycle Time | 10 days | 6 days |
| Admin Hours/Week | 40 hrs | 25 hrs |
Clinical Outcomes & EHR Integration Benefits
A practice does not opt for an EHR integration project just because of the financial benefits it provides. In fact, care delivery and ease in other clinical aspects of your practice are why you want to go ahead with EHR integration.
On that note, let’s see how EMR EHR integration improves patient care quality and clinical effectiveness that goes beyond care and efficiency.
- Reduced Medical Errors & Duplicated Tests: EHR integration helps in centralizing your system. With this, you get unified patient data across systems. This eliminates the chances of errors by a huge margin, and repeated diagnostic processes can also be reduced. However, the main EHR integration benefits can be seen in eliminating manual entry errors.
- Enable Faster Diagnosis & Better Coordination: Real-time access to complete records of a patient allows the providers to make important clinical decisions quickly. This sets the pace of care delivery, where you can ensure that every member of the care team is on the same page and working towards the same goals. This shows how collaboration improves care delivery.
- Improve Patient Engagement & Satisfaction: Integrated systems support better communication, for instance, patients can easily check their data on patient portals and even update their data in real-time. Also, follow-ups become more accurate, leading to more informed and satisfied patients.
- Enhanced Population Health Outcomes: With aggregated and connected data, healthcare providers can easily track trends in patient populations. This has been effectively used by many practices to manage chronic conditions and improve patient outcomes at scale.
In short, EHR integration ROI is driven by not just savings but ensuring your care delivery processes become much safer, decision-making is faster, and patient outcomes improve by a margin.
Common Challenges in Measuring EHR Integration ROI
Measuring EHR integration ROI isn’t as straightforward as it appears for other industries. There have been certain challenges that can give you an unclear or incomplete picture. Here are some of the common EHR integration ROI challenges you’re likely to encounter while messing with and how you can overcome them:
| Challenge | Meaning | Impact on ROI Measurement | Solution |
| Lack of baseline data | No clear pre-integration metrics to compare against | Makes it difficult to quantify actual improvements and prove ROI | Establish baseline KPIs before integration (e.g., denial rates, admin hours, patient throughput) and document them consistently |
| Attribution challenges | Hard to separate the impact of integration from workflow or process changes | Can lead to overestimating or underestimating ROI | Use phased implementation or pilot programs to isolate impact and compare controlled before–after scenarios |
| Measuring intangible benefits | Benefits like patient experience and care quality are not easily quantifiable | Important value is overlooked or undervalued in ROI calculations | Use proxy metrics like patient satisfaction scores, readmission rates, and clinician feedback surveys |
| Inconsistent tracking systems | Disconnected tools or lack of standardized KPIs | Results in inaccurate, fragmented, or unreliable ROI reporting | Implement centralized dashboards and standardize KPI definitions across departments |
Maximizing EHR Integration ROI
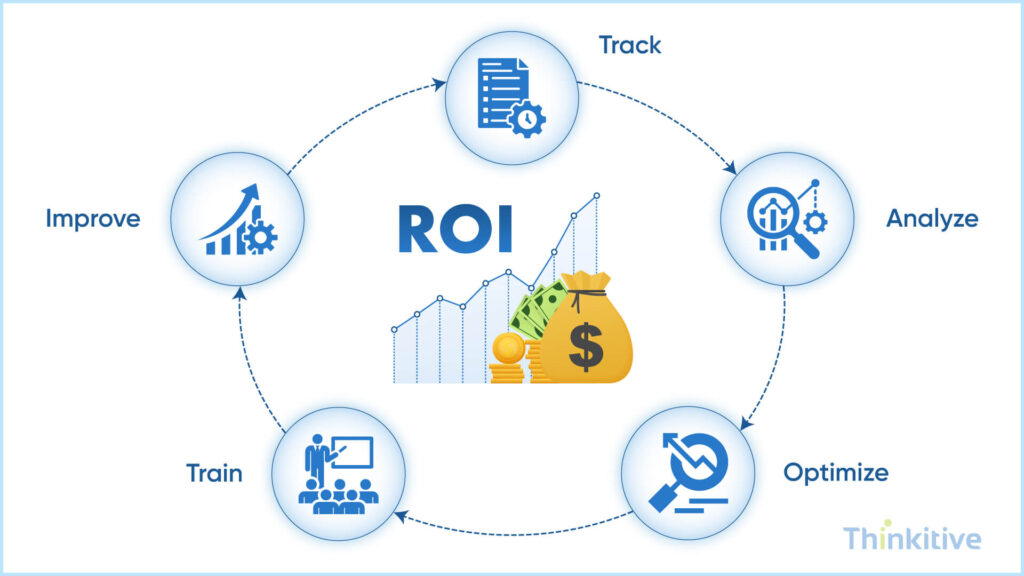
Sustaining and increasing your ROI is a continuous process. You can achieve it once indeed, but if you stop there, it can negatively impact the further processes of your system, which can impact your practice’s finances over the course of time.
On that note, here are certain best practices that can help you maximize your EHR integration ROI:
- Continuously Track ROI KPIs: As they say, consistency is the key; this is true everywhere. You see, you have to regularly monitor the key metrics of your ROI across various processes, right from a financial standpoint to operational efficiency and clinical accuracy. This is to ensure gains are maintained, and new opportunities can be identified.
- Align with Business & Clinical Goals: Ensure that your integration outcomes support the broader objectives of your business, like revenue growth, improved care quality, and compliance with necessary regulatory bodies. This is to ensure that your ROI stays relevant and does not go off track.
- Drive User Adoption: You can harness maximum EHR integration benefits when your users are able to use it effectively. So, invest in training and workflow alignment for maximum utilization.
- Using Performance Insights to Optimize Performance: Leverage data from your dashboards and reports to refine your workflows. Data can be your roadmap for growth, which allows you to identify gaps, fix bottlenecks, and improve outcomes continuously.
Conclusion
Understand that EMR EHR integration ROI is not just a one-time result. In fact, it is an ongoing process of tracking, optimizing, and aligning technology with real-world outcomes.
Furthermore, the true value of your EHR integration ROI can also be achieved with continuous performance tracking. Furthermore, develop a continuous performance monitoring mechanism so that you can reinforce the long-term business impact of your EHR integration.
So, this is how you calculate your EHR integration ROI. And if you’re still looking for a vendor for your EHR integration, then book a call with our integration experts, and let’s see your system readiness for EHR integration.
Frequently Asked Questions
EHR integration ROI refers to the measurable financial, operational, and clinical value gained from connecting healthcare systems. It evaluates how integration improves efficiency, reduces costs, and enhances care delivery.
Understanding the ROI of healthcare technology is important because it helps healthcare organizations justify investments, prioritize initiatives, and ensure long-term value from their digital infrastructure. It also enables leadership to align IT decisions with business and patient care goals.
To understand how to measure EHR integration ROI, organizations must first establish baseline performance metrics and then track improvements after integration.
This involves:
- Defining KPIs across financial, operational, and clinical areas
- Monitoring performance through dashboards and reporting tools
- Comparing pre- and post-integration outcomes
A structured EHR integration ROI calculation ensures that both tangible and intangible benefits are captured effectively.
The EHR integration ROI calculation relies on a mix of financial, operational, and clinical metrics, including:
- Claim denial rates and billing cycle time
- Administrative workload and time savings
- Patient throughput and staff productivity
- Reduction in duplicate tests and medical errors
These EHR efficiency metrics provide a comprehensive view of how integration impacts performance and profitability.
The most impactful EHR integration benefits include:
- Reduced manual data entry and administrative costs
- Faster clinical workflows and improved care coordination
- Fewer claim denials and faster reimbursements
- Enhanced patient experience and engagement
These benefits directly influence the ROI of healthcare technology by improving both financial outcomes and care quality.
EHR efficiency metrics play a critical role in quantifying ROI by measuring improvements in time, productivity, and workflow performance.
For example:
- Reduced documentation time per patient
- Increased number of patients seen per day
- Lower administrative workload
These metrics help demonstrate the ROI of automated clinical workflows, showing how integration drives measurable operational gains.
Measuring EHR integration ROI can be complex due to:
- Lack of baseline data for comparison
- Difficulty in isolating the impact of integration from process changes
- Challenges in quantifying intangible benefits like patient experience
- Inconsistent tracking systems across departments
Addressing these challenges is essential for accurate EHR integration ROI calculation and decision-making.
The timeline for achieving EHR integration ROI typically ranges from 6 to 18 months, depending on the scale of implementation and system complexity.
- Short-term gains: workflow efficiency and time savings
- Mid-term gains: improved billing and reduced denials
- Long-term gains: enhanced care outcomes and scalability
Tracking EHR efficiency metrics consistently helps organizations monitor progress and validate ROI over time.
To maximize EHR integration ROI, organizations should:
- Continuously track ROI-focused KPIs
- Align integration outcomes with financial and clinical goals
- Improve system adoption through training and workflow optimization
- Use performance insights to refine processes
Focusing on the ROI of automated clinical workflows and ongoing optimization ensures sustained value and long-term success.




