In-House vs Outsourced EHR Integration: Which Approach Saves More?

When it comes to IT projects, things can get quite tricky. You see, having an IT infrastructure and maintaining it for the efficiency of your practice can be quite costly. Typically, you feel like having someone else do this job for you would do the trick, but really?
Think about it. It’s like giving up your locker by opening a door yourself. But slowly, depending on the evolving needs of your practice and healthcare landscape in general, you feel like having my own team would be great.
And you’re not wrong. You just need someone who can get you data from a software in a different country to your system, right? Things sometimes simply don’t make sense. You want to go for the speed of your system, and sometimes you feel like controlling the data that is flowing into your system.
Healthcare leaders usually struggle with these instances where important choices have to be made. Because both are necessary, depending on where you see it or require it. Still, they are not to be blamed completely. The healthcare IT industry only gives them one of the two choices that it can provide – in-house vs outsourcing EMR system integration.
Having a keen attention to these aspects is necessary because these decisions shape your EHR integration strategy, and on that depends your EHR integration cost.
On that note, let’s deep dive into these strategies and check which one of them is more economical and suitable for your practice.
So, without further ado, let’s try to solve the billion-dollar question in the healthcare industry: build vs buy!
In-House EHR Integration: Control Comes at a Cost
Alright, let’s begin by addressing the most obvious question – whether to have an in-house team or not. To be honest, it has immense advantages that can change the game for your practice, if done right and if your practice actually needs it.
But let’s get a few things straight. It gives you full control over all your system, and this comes with a significant investment plan and responsibility that can be too overwhelming at times. Let’s talk about that in a little detail here:
- Internal Resources: First things first, you need to hire specialists, and that drives your entire IT landscape for your practice. These specialists must be well-versed in standards like HL7 and FHIR. This increases cost and workload, whether you have an existing team or not.
- Infrastructure Costs: Setting up and maintaining servers, APIs, and middleware can be costly. Moreover, spending on tools and technical aspects of your practice can later be costly, so it acts as an important investment.
- Compliance Responsibility: When you have an in-house team, adhering to compliance becomes absolutely necessary; your team must adhere to the regulations of HIPAA and system requirements under the 21st Century Cures Act.
- Time & Risk: Building an in-house team is a time-consuming process, and it can at times possess risks for errors, delays, and rework.
Furthermore, you need more control of your system with customization room, then this approach is perfect, but it comes bearing cost, efforts, and risk. It can be best suited for a large healthcare system where the dependency on healthcare systems is highest.
Why Healthcare IT Outsourcing Delivers Faster Results
On the other side, there is the option of healthcare IT outsourcing. Now, I know, it’s like giving your control to someone else; it can deliver results at a much faster rate, and the external expertise does open multiple ways of doing something.
Having said that, let’s see how this can be beneficial for your organization:
- Specialized Expertise: Vendors bring experienced teams with similar standards, like HL7 and FHIR, along with pre-built integration frameworks. This reduces the need to build from scratch.
- Faster Implementation: Outsourcing teams often show proven workflows, reusable components, and other aspects of development. This cuts down time drastically and speeds up the entire process.
- Predictable Pricing: On top of that, outsourcing IT teams can be quite predictable. You see, most engagement appears on a project basis, a milestone basis, or a fixed cost basis. This way, you can manage your practice’s financial aspects in a much better way.
- Shared Compliance Responsibility: Last but not least, with the vendor’s assistance, you can easily meet regulations like HIPAA and reduce the security burden by simply sharing it.
In simple words, healthcare IT outsourcing costs less for setup, leads to faster execution, and results in more predictable outcomes with reduced internal strain.
In-House vs Outsourced EHR Integration Cost Comparison
Let’s try to understand the total cost of ownership for EHR integration and discuss the hidden costs of in-house EHR integration. Refer to the table below for a better understanding:
| Factor | In-House Integration | Outsourced Integration |
| Upfront Investment | High (hiring specialists, infrastructure setup) | Moderate (vendor or project-based fees) |
| Time-to-Market | Slower due to team setup and development from scratch | Faster with experienced teams and pre-built solutions |
| Scalability | Limited by internal team size and capabilities | Easily scalable based on project needs |
| Compliance Responsibility | Fully managed internally (e.g., HIPAA) | Shared with vendor, reducing internal burden |
| Maintenance & Support | Continuous internal costs (updates, monitoring, fixes) | Managed through contracts or SLAs |
Financial Breakdown Behind the Comparison
Here is a quick breakdown of the intricacies of this breakdown.
- Direct Costs: So, first things first, let’s see what you have to pay upfront. It includes salaries, infrastructure, and vendor contracts.
- Opportunity Cost: The delayed launch and lost revenue due to inefficiencies turn into opportunity cost. Meaning, it would give you a brief note about what could be done if not spent on that.
Total Cost of Ownership & Hidden Costs
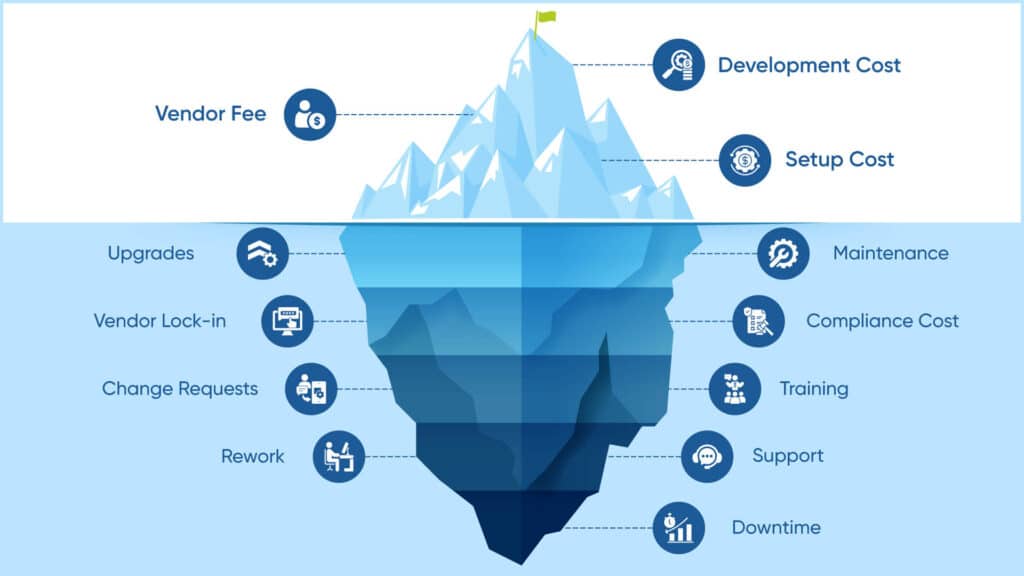
Talking about the total cost of ownership and hidden costs, here are a few things that you need to know.
So, understand, when you are investing in this, long-term ownership is something that you need to keep at the back of your mind. And what I mean by ownership is that it is about maintenance, updates, and support that comes with it.
So, here are the hidden costs of in-house EHR integration:
- Hiring Delays & Retention Challenges: Any delays in hiring will be costly and can impact processes that you never thought of. Furthermore, when it comes to the retention of these resources, it can again turn into a costly venture altogether.
- Technical Debt & Inefficient Codebases: The technical aspects of your EHR integration and codebases can be quite daunting. You see, the technical aspects can disrupt your budget, but they can be easily navigated with proper means.
- Scaling Limitations: In-house integration is often constrained by team size and internal resources, making rapid scaling difficult. On the other hand, outsourcing allows organizations to scale integration faster based on demand.
- Vendor Dependency vs Internal Scalability: Outsourcing can reduce the workload of your teams by a huge amount. Furthermore, it also creates reliance on external vendors. On the other hand, in-house gives you full control and independence over your systems.
TOC – Total Cost of Ownership
The total cost of ownership goes beyond upfront costs. You know, here you need to evaluate long-term expenses like maintenance, upgrades, compliance, and support, the true cost over a course of time for a few years.
Long-Term Cost Impact
Furthermore, as the system grows with your practice, more integrations are added to the system. In such cases, in-house costs can increase due to staffing and infrastructure. On the other hand, outsourced models can be more predictable and, at times, be recurring.
When to Choose in-House vs Outsourced Integration
Still confused about what choice to make?
Refer to this table of checklist before for better clarity on this:
| Scenario | Choose In-House Integration | Choose Outsourced Integration |
| Control & Customization | When full control and deep customization are critical | When standard workflows and faster deployment are acceptable |
| Technical Expertise | When you have a strong internal team experienced in HL7 / FHIR | When you need immediate access to specialized expertise |
| Speed & Time-to-Market | When timelines are flexible | When rapid implementation is a priority |
| Resource Availability | When sufficient internal resources and budget exist | When internal teams are limited or overloaded |
| Risk & Compliance | When you prefer full control over compliance (e.g., HIPAA) | When you want to share compliance and security responsibility with a vendor |
| Scalability Needs | When scaling can be handled internally over time | When you need flexible, on-demand scaling |
Conclusion: Which Approach Saves More?
Now, if you have made it till here, I want to ask the actual number in EHR integration cost, trust me, I don’t!
Yes, there is no definite number, because the intricacies related to cost, control, and speed can be quite intimidating. Moreover, outsourcing can reduce time-to-market and operational burden from your staff.
On the other hand, in-house can be suitable in the long term and can be highly customized systems. On that note, know which one suits your practice with this consultation call.
Frequently Asked Questions
The in-house vs outsourced EHR integration cost can vary significantly based on scope and complexity. In-house integration typically requires higher upfront investment due to hiring, infrastructure, and tooling, often reaching hundreds of thousands annually. In contrast, healthcare IT outsourcing offers a more predictable cost model with lower initial expenses.
In most in-house vs outsourced EHR integration cost comparisons, outsourcing can reduce overall costs by 30–60%, especially for small to mid-sized healthcare organizations.
Several factors directly impact EHR integration cost, including:
- Number of systems being integrated
- Use of standards like HL7 and FHIR
- Data complexity and volume
- Customization requirements
- Compliance and security needs
Additionally, long-term medical data integration cost increases with scalability requirements and ongoing maintenance.
While healthcare IT outsourcing is cost-effective initially, it can become more expensive over time if:
- Long-term dependency on vendors leads to recurring fees
- Extensive customization is required beyond standard offerings
- Integration needs are continuous and large-scale
In such cases, organizations with strong internal teams may find better value in an in-house EHR integration strategy over the long term.
The hidden costs of in-house EHR integration are often underestimated and include:
- Ongoing hiring and training of specialized developers
- Infrastructure upgrades and system maintenance
- Compliance management (e.g., HIPAA)
- Debugging, rework, and downtime risks
These hidden factors significantly increase the overall EHR integration cost beyond initial estimates.
Healthcare IT outsourcing reduces time-to-market by leveraging:
- Pre-built integration frameworks
- Experienced teams familiar with FHIR and other standards
- Established workflows and faster testing cycles
This allows healthcare providers to deploy integrations faster, reducing delays and accelerating ROI—an important factor in any EHR integration strategy.
The total cost of ownership for EHR integration includes:
- Initial development or vendor costs
- Infrastructure and tooling
- Ongoing maintenance and updates
- Compliance and security management
- Scaling and future integrations
A proper in-house vs outsourced EHR integration cost comparison should always consider TCO over 3–5 years, not just upfront investment.
The best EHR integration strategy depends on organizational goals:
- In-house is ideal for large healthcare systems needing full control and deep customization
- Outsourced works best for organizations prioritizing speed, scalability, and cost predictability
A hybrid approach is also common, balancing control with external expertise to optimize medical data integration cost over time.
Both models can be secure if implemented correctly.
- In-house integration offers full control over data and security protocols
- Healthcare IT outsourcing providers often bring advanced security frameworks and compliance expertise
Ultimately, security depends more on implementation quality and adherence to standards like HIPAA than the chosen model itself.




