EHR Integration: The Complete Guide for Healthcare Organizations
The introduction of Electronic Health Records in healthcare has marked the beginning of data-driven care delivery. In fact, the data has become the epicenter of healthcare practices, and it has been used for administrative and financial aspects of the practice as well.
Despite this, it is surprising to see that 97% of healthcare data goes unused, according to the World Economic Forum. Though it would be practically impossible for all of the data, one of the major reasons for this gap lies in the data fragmentation, as you can see, almost 80% of healthcare data is unstructured.
Drawing parallels with this stat, the system complexity also has a role to play in this. On average, a healthcare organization uses almost 10-16 systems, according to KLAS Research.
Now, take a step back and try to understand the impact these gaps have on care delivery and other aspects of healthcare practice, such as operational efficiency and cost.
Having said that, these gaps have created a specific need for EHR integration in healthcare. Moreover, in today’s ecosystem, EHR integration enables your healthcare system to fetch, send, and receive data from disparate healthcare systems, both automatically and on demand.
But there is a lot of confusion about electronic health record integration in healthcare systems, and most people have asked how electronic health record integration works.
On that note, let’s discuss the intricacies of electronic health record integration for healthcare organizations and everything that comes in between. Moreover, let this be your EHR integration guide for your practice.
And without further ado, let’s get started!
What is EHR Integration in Healthcare?
As a healthcare provider, you might know what EHR integration is in healthcare. However, for those who have limited knowledge about healthcare data integration, let’s begin with the basics.
So, EHR integration in healthcare is the process of connecting EHR systems with other digital tools or systems, such as labs, billing, imaging, pharmacy, etc., for seamless, real-time data exchange between those systems.
Once all your healthcare systems are connected, parallels can be drawn between patients’ health data and operational data, unifying both types of data across your healthcare systems. This improves accessibility to data, streamlines operational aspects, and enables data-backed care delivery practices.
Sounds simple, right? Well, it is actually simple!
However, there is certain terminology that you must understand to fully understand EHR integration for healthcare practices:
- Data Exchange: As the name suggests, it is the simple transfer of data from one system to another. For instance, sending files from one system to another.
- Integration: As defined earlier, it is the process of connecting different and disparate systems so that they share data more efficiently. This is usually done by APIs, interfaces, or middleware.
- Interoperability: Now, this is where it gets tricky. You see, interoperability is the ability of systems to exchange, interpret, understand, and use data in connected systems meaningfully.
Remember the unstructured data problem we talked about earlier? Well, with interoperability, that data can be structured, standardized, and usable for your system and practice to make real-time decisions.
Furthermore, there are different types of integrations. Let’s have a brief understanding of that below:
- API-Based Integration: In this type of integration, systems communicate and exchange data with each other directly using APIs (Application Programming Interfaces), typically REST APIs.
- Middleware Integration: In this, a central layer, also known as an integration engine, is used to connect multiple systems, and it manages how the data flows between systems.
- Point-to-Point Integration: Unlike the previous types of integration, in this type of integration, a direct connection is established between two systems, and the data flows directly between them.
All these types of integration can be used, but they come with their own advantages and disadvantages. However, the best possible option for your system and practice can be decided depending on your needs.
How Electronic Health Record Integration Works
Answering your main question: how does electronic health record integration work? Let’s start with the basics, yet again.
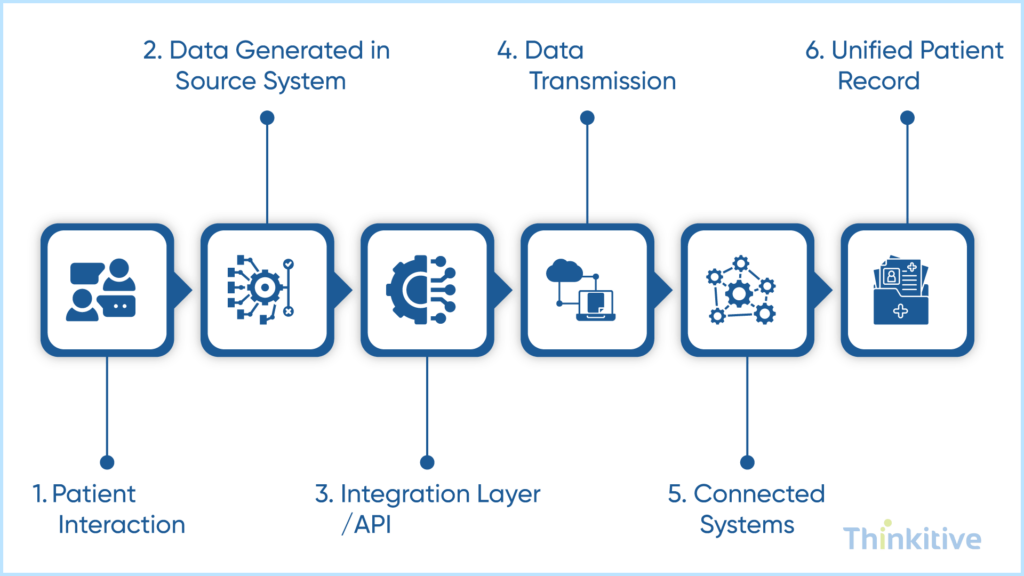
At the core, EHR integration is nothing but moving and synchronizing patient data across the system so that providers can get a complete and up-to-date overview of the patient’s health. For understanding this better, let’s try to understand this flow:
- A patient interaction occurs, such as a patient visit, lab tests, prescription, etc.
- The data gets generated in that system, for instance, in the lab systems.
- This data is then captured by the integration layer or APIs and converted into a standardized format.
- This standardized and formatted data is then transmitted to other connected systems.
- The receiving system stores and displays the data in the right context to avoid confusion.
In this way, a unified patient record is created with EHR integration. Some of the systems that are typically connected refer to this table for a comprehensive overview:
| System Type | What Data It Handles | Why Integration Matters |
| EHR / EMR System | Patient records, history, diagnoses, medications | Acts as the central hub for all patient data |
| Lab System (LIS) | Test orders and lab results | Enables faster diagnosis with real-time updates |
| Billing / RCM System | Claims, invoices, insurance data | Ensures accurate billing and fewer denials |
| Radiology (RIS/PACS) | Imaging data (X-rays, MRIs, CT scans) | Provides seamless access to diagnostic images |
| Medical Devices / IoT | Vitals and monitoring data | Supports real-time patient monitoring |
| Patient Portal / Apps | Appointments, records, communication | Improves patient engagement and experience |
One of the most important things you need to know during healthcare data integration is that the connected system must be able to speak the same language. For this standard, your EHR integration should rely on standards like HL7, FHIR, DICOM, etc. This ensures that your data is structured, consistent, and interpretable.
Real-time vs Batch Data Exchange
There are two major types of data exchanges that are being used in healthcare systems. From the subheading, you must have got an idea, real-time exchange and batch exchange:
Let’s try to understand it briefly:
So, real-time data exchange is when the data is shared instantly. This is typically used for critical workflows such as alerts, vitals, emergency care, etc. On the other hand, batch data exchange is when the data is sent at scheduled intervals, and this type of approach is typically used for reporting, billing, and analytics.
Given the need for healthcare practices and data, most practices use a hybrid approach for their data exchange, depending on their needs.
Security Basics
Given the sensitive nature of data, the integration must be secure. On that note, here are some security basics that will be useful for you:
- Data Encryption: Encrypt your data both when it is at rest and during transit, to prevent unauthorized interceptions.
- Access Control: Implement role-based access controls to allow only authorized users to see specific data.
- Secure APIs: Use APIs that use secure protocols such as HTTPS and OAuth to ensure only trusted systems can exchange data.
Why EHR Integration is Critical for Healthcare Organizations
The digital push brought in by the use of healthcare technology has made electronic health record integration in healthcare systems a necessity. In this section, let’s try to understand why EHR integration has become so critical for healthcare organizations.
- Eliminating Data Silos: EHR integration in healthcare basically solves the problem of data silos. You see, when you use multiple systems for managing your healthcare practice, the data gets stored in different systems, isolating the data. However, with this EHR integration use case, data isolation or data silos can be easily overcome, creating a unified data system.
- Improving Clinical Decision-Making: Access to data is indeed improved with healthcare data integration. Due to this, both providers and healthcare staff can access healthcare data in real time, allowing them to make quick decisions backed by data.
- Enhancing Operational Efficiency: With both clinical and administrative data being at your disposal, operational activities that used to be delayed due to the unavailability of data can be streamlined. Due to this, billing processes, claims submission, referrals, and reminders can be streamlined.
- Supporting Value-Based Care: The entire healthcare industry is shifting towards value-based care delivery, and this data has a crucial role to play. Here, EHR integration gives instant access to providers, allowing them to pivot from traditional care delivery to data and evidence-backed value-based care.
Due to the reasons mentioned above, EHR integration has become so critical for healthcare organizations. Another benefit that healthcare organizations get with EHR integration is scalable solutions.
EHR Integration Use Cases in Modern Healthcare
Most of the time, as a healthcare provider, you might know some of the use cases of EHR integration. However, some of the use cases might still surprise you. On that note, here are some of the EHR integration use cases that you need to know before moving ahead with your custom EHR integration venture:
- Hospital System Connectivity: Being one of the most popular use cases of EHR integration, it is what most healthcare providers aim for. When your system is connected to the hospital systems, care delivery can be enhanced.
- Telehealth & RPM: Telehealth has become a new norm in the healthcare space, given the patient demand. On top of that, integrating your system with IoMT and RPM devices, you can even collect data in a remote setting and adopt a complete digital care experience.
- Billing & Revenue Cycle Integration: EHR integration gives you access to almost all the types of data that are required for billing. Due to this, your billing processes can be improved, and the revenue cycle can be streamlined and predictable, allowing you to take necessary steps to improve your practice’s financial health.
- Patient Engagement Platforms: Patient engagement is one of the core aspects of healthcare delivery. And for keen engagement, you need to empower patients and make them aware of their health. On the basis of data, this can be done, and EHR integration has a huge role to play in this, as it can directly show patient data in the patient portal.
- Multi-Provider Care Coordination: How can you ensure all the care team members in the patient’s care team are on the same page and working towards the same goal? Well, again, it can be done with EHR integration. You see, with access to data in real-time, providers can coordinate care accordingly and ensure an appropriate care journey for the patient while considering their needs and preferences.
EHR Integration for Specialty Practices
Over the years, healthcare practices have moved from general hospitals and clinics to specialized practices in certain specialties. This is where you need custom EHR integration. Wondering why?
Well, specialty practices require a unique integration approach, given their workflow and data requirements. For instance, in cardiology, the workflow moves from consultation, tests, prescriptions, and the rest. Here, the EHR integration process needs to be curated specially so that it can align with the needs of the practice.
The same is the case with radiology of behavioral health; as the workflow changes, the intricacies of the healthcare data integration also change. Along with that, one of the EHR integration challenges that you will face for a specialty is data standardization. Since some data is measured in unique formats, that data needs to be standardized so that your system can understand and make appropriate use of it.
Custom EHR Integration for Complex Workflows
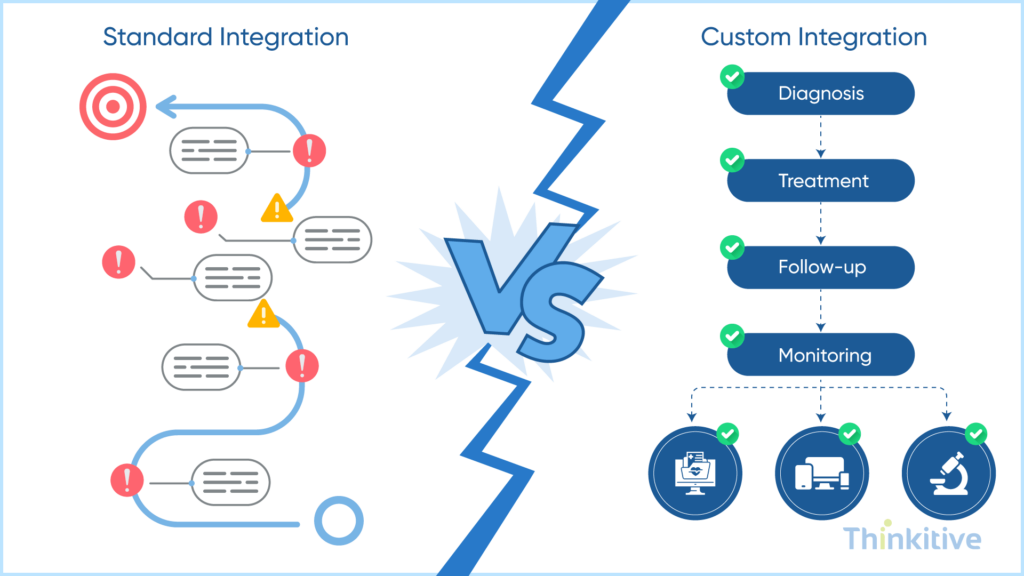
Standard EHR integration practices work well for common use cases, such as data transfer from labs or pharmacies to your system. However, given the specific case for healthcare practices, it is quite rare to find a standard EHR integration use case for your workflows. This is why custom EHR integration becomes necessary to address complex workflows and ensure your system aligns with your care delivery.
Let’s dive deep into the intricacies of custom EHR integration for complex workflows:
- Limitations of Standard Integrations: First things first, standard integrations are designed for generic healthcare workflows. Due to this, specialty-specific EHR integration can be hard to achieve. Along with that, with rigid data formats and workflows, handling multi-step processes becomes difficult, and poor support is shown for unique business rules.
However, you might think, ‘Why do I need custom EHR integration?’
Well, here are some of the reasons why you need a custom EHR integration:
- Specialty practice with specialty-specific workflows
- Multiple systems with a unique need for complex coordination
- Requirement of real-time decision support or automation
- Still uses legacy systems that don’t support APIs or modern standards.
- Practice’s unique operational or compliance requirements
With custom EHR integration, you can define the architecture that matches your real clinical and operational needs. For instance, if your practice has a multi-step care pathway, like diagnosis followed by treatment, then follow-up, and then monitoring.
Also, you will need custom EHR integration if you need to integrate device data with alerts and clinical action, or if you have specialty-specific data models. However, most of the time, custom EHR integration is commonly used for conditional workflows, so that your system can adapt to the unique workflows.
And last but not least, the benefits that you get with this are flexibility, scalability, control over data, logic, and integrations, and improved efficiency and outcomes.
EHR Integration Challenges & How to Approach Them
EHR integration has become a crucial part of healthcare practices’ digital ecosystem; however, integrating is easier said than done. The EHR integration process is filled with technical, operational, and regulatory hurdles that can slow down your integration efforts or create complications in implementation.
In this section, let’s look at some of the major EHR integration challenges and how you can overcome them:
| Challenge | What It Means | Solution |
| Data Silos & Interoperability Gaps | Patient data is fragmented across systems, making it hard to access and use effectively | Use standards like FHIR, implement APIs/middleware, and focus on unified data exchange |
| Legacy Systems & Limited APIs | Older systems lack modern integration capabilities and use proprietary formats | Use middleware to bridge systems, adopt hybrid integration, and modernize gradually |
| Compliance & Security Concerns | Sensitive healthcare data requires strict protection and regulatory adherence | Implement encryption, role-based access, secure APIs, and align with frameworks like HIPAA |
| Cost & Resource Constraints | Integration projects can be expensive and resource-intensive | Prioritize high-impact use cases, adopt phased implementation, and use scalable technologies |
| Lack of Strategy & Planning | Poor planning leads to delays, inefficiencies, or failed integrations | Define clear goals, create a roadmap, align stakeholders, and choose the right integration approach |
Key Technologies Behind EHR Integration
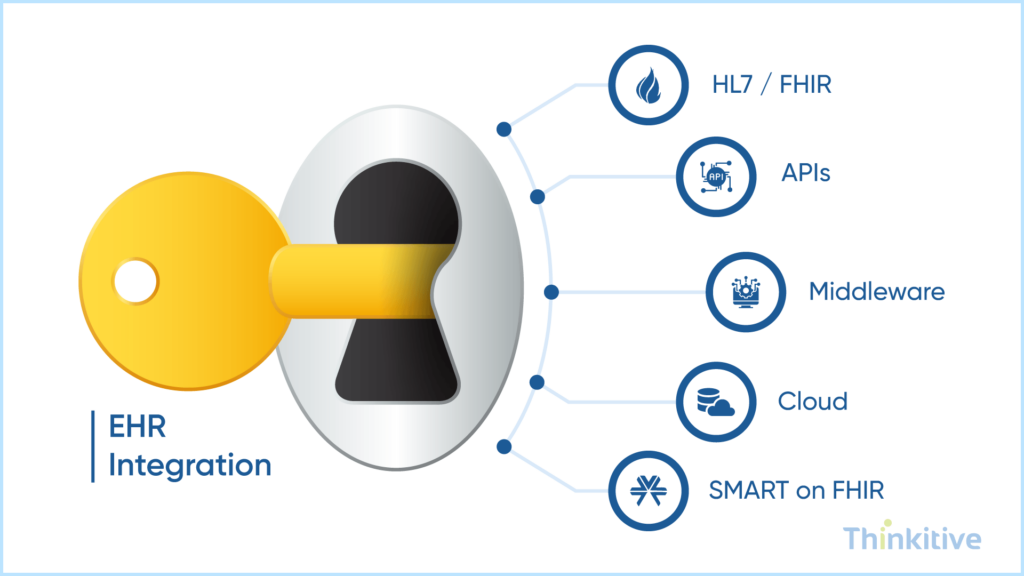
The technological landscape for EHR integration is quite different from what you usually encounter in healthcare software development. While you might be familiar with the terminology, here is a brief about the technologies behind xxxx`EHR integration:
- HL7 & FHIR: Remember the healthcare standards we talked about earlier? Well, HL7 or Health Level Seven is the organization that develops the international standards for healthcare data exchange. Furthermore, FHIR, also known as Fast Healthcare Interoperability Resources, is HL7’s modern standard, which is driven by APIs. These standards are designed to enable the sharing of electronic health data securely and efficiently.
- APIs & Middleware: As explained earlier, middleware is the integration layer that connects your system with other systems, and data exchanges are fostered through that layer. On the other hand, APIs are a set of rules and protocols that allow your system to communicate with other systems and exchange data. It basically acts like a middleman for the two systems.
- Cloud Platforms for Healthcare Data Integration: Cloud platforms give you enough space to store data. However, the advantage you get with using cloud platforms for healthcare data integration is that it breaks all the accessibility barriers and allows your system to connect and share data instantly.
- SMART on FHIR Ecosystem: This is an open-standards-based technology framework that allows healthcare applications to securely and seamlessly connect with EHRs to exchange information in real-time.
Best Practices for EHR Integration Success
EHR integration is quite a complex process, and if you have gone through all the challenges that are mentioned above, then you must know that the success of your EHR integration project heavily depends on the approach that you choose.
On that note, here are some of the best practices that you must be aware of for EHR integration success:
- Define Clear Goals & Use Cases: The very first factor that determines the success of your EHR integration project is defining the project’s goals and the use cases of EHR integration. With clear goals, you would know which part of the data you need from another system and how to use it. Due to this, most of the processes and the implementation roadmap become clear.
- Choose the Right Integration Approach: The right EHR integration approach is a crucial factor in your project’s success. You see, depending on your needs, system, and use cases, not only the type of integration but also its nature can change. That is why choosing the right integration approach is important, and consulting healthcare IT professionals can prove to be crucial in this.
- Ensure Security & Compliance: Given the sensitive nature of healthcare data that you deal with, your EHR integration project must comply with HIPAA, implement data security features like data encryption and role-based access. Along with that, during the entire implementation process, ensure that your EHR integration processes align with the regulatory requirements right from the start.
- Design for Scalability & Future Interoperability: Design the EHR integration architecture with considerations of scalability. You see, your practice is bound to grow with time, and for your system to accommodate huge volumes of data, your integration bridge needs to be scalable and aligned with future interoperability.
- Align Clinical, Technical & Operational Stakeholders: Ensure that all the stakeholders of your practice are involved during the process. This is important so that you can align the clinical, technical, and operational needs of your practice.
EHR Integration Implementation: High-Level Roadmap
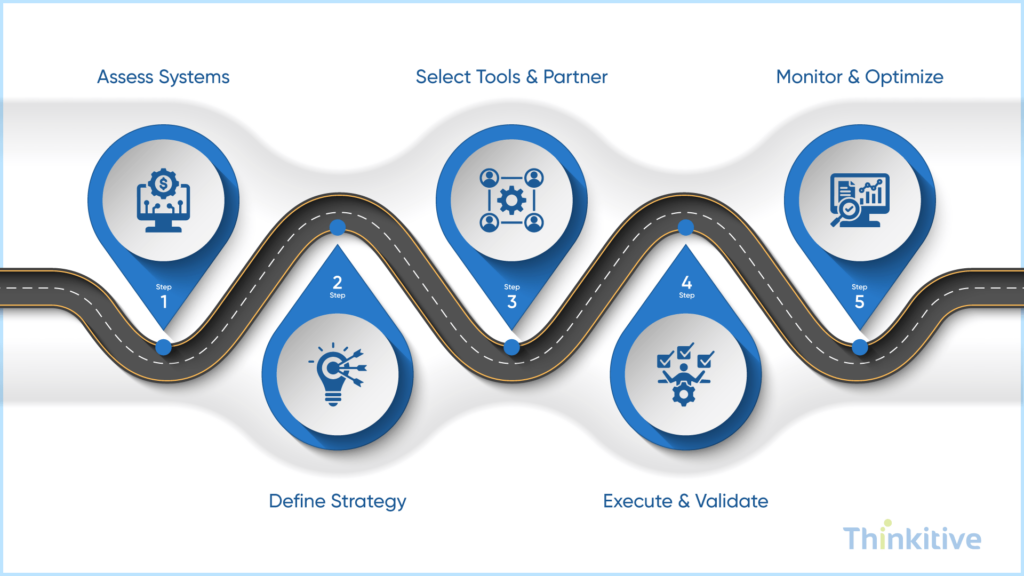
If you have made it till here, then you’re in for a treat, my friend. The EHR integration implementation roadmap will help you ensure that no stone is left unturned during the EHR integration implementation.
- Assess Current Systems & Integration Gaps: The very first step in this roadmap is to assess your current system for integration and find the gaps that act as a barrier to your EHR integration. Why is this important? Well, when you assess the system and find out the gaps, the future roadmap of implementation becomes clear.
- Define Integration Strategy: Now that you have the implementation roadmap, it’s time to curate and define an appropriate EHR integration strategy that will cover all the aspects of your integration process.
- Select Tools & Partner: From standards to necessary tools, everything becomes important when it comes to implementation. However, the most important aspect in this is clearly your EHR integration partner. Select the right tools and the right partner so that your EHR integration works just like you want it to.
- Execute & Validate Integrations: Once you have the plan ready, execute these integrations and validate them so that you can ensure they function as they are intended to.
- Monitor & Optimize Performance: Once the integration is validated, all you need to do is sit back and monitor the integration for its relevance and correctness. Also, while monitoring, note down the gaps so that you can improve the EHR integration performance.
Future Trends in EHR Integration
As the technological and healthcare landscape evolves, keeping an eye on future trends in EHR integration can help you stay one step ahead.
- Rise of FHIR-first Ecosystems: With FHIR being a widely used standard for EHR integration. So, having an FHIR-first ecosystem can help you future-proof your system for integrations.
- Growth of Patient-Centric Data Exchange: Another trend that is gaining traction in the healthcare industry is that of patient-centric data exchange. This can not only push your practice for value-based care delivery, but also ensure the correctness of other processes.
- Integration with Wearables & Digital Health Platforms: With RPM entering the mainstream healthcare delivery process, integration with wearable devices and digital health platforms will help you make your practice future-proof for the digital care delivery landscape.
- AI-Driven Integration & Intelligent Data Utilization: With AI-driven integration and intelligent data utilization, your system can not only help you automatically bridge the gaps in the integration bridge but also use all the data to provide healthcare professionals with a comprehensive overview of the patient’s health data.
- Automated Data Mapping & Normalization: Another use case of AI in EHR integration is that of the automated data mapping and data normalization processes. Due to this, most of the processes of your data integration in healthcare can be covered.
Conclusion: Building a Connected Healthcare Ecosystem
Hush, if you’ve made it till here, then I appreciate your dedication, and somewhere it also tells me that you’re quite serious about EHR integration. Having said that, understand that integration is a long-term strategic investment for your practice.
In simple terms, it sets the foundation of a connected healthcare ecosystem. So, if you are considering a custom EHR integration, then this is the right time to move towards a unified and intelligent healthcare system. And I hope this guide will help you in ensuring the success of your EHR integration project.
So, what are you waiting for? Get your first consultation and set the foundation of a future-ready care delivery system.
Frequently Asked Questions
EHR integration in healthcare refers to the process of connecting electronic health record systems with other healthcare applications, platforms, and data sources. This enables seamless data exchange, improves clinical workflows, and ensures that patient information is accessible across systems in real time.
Electronic health record integration in healthcare systems works by using APIs, middleware, and interoperability standards like HL7 and FHIR to enable data exchange between systems. It allows data to flow between EHRs, labs, billing systems, and other healthcare platforms without manual intervention.
EHR integration focuses on connecting systems to exchange data, while interoperability ensures that the exchanged data is understood and usable across different systems. In simple terms, integration enables connectivity, whereas interoperability ensures meaningful data exchange.
EHR integration in healthcare improves care coordination, reduces administrative burden, minimizes data duplication, and enhances clinical decision-making. For healthcare organizations, it leads to better patient outcomes and more efficient operations.
Healthcare data integration acts as the backbone of EHR integration by aggregating, transforming, and synchronizing data across multiple sources. It ensures consistency, accuracy, and accessibility of patient data across healthcare systems.
Common systems that can be connected through electronic health record integration for healthcare organizations include:
- Laboratory Information Systems (LIS)
- Radiology Information Systems (RIS)
- Practice Management Systems (PMS)
- Billing and Revenue Cycle Management (RCM) systems
- Patient portals and mobile apps
- Remote Patient Monitoring (RPM) devices
- Health Information Exchanges (HIEs)
Typical EHR integration use cases include:
- Lab and diagnostic data integration
- ePrescribing and pharmacy connectivity
- Patient portal synchronization
- Telehealth platform integration
- Billing and claims automation
- Remote patient monitoring data capture
Common EHR integration challenges include:
- Data silos and inconsistent formats
- Limited API access in legacy systems
- Compliance and security concerns
- High implementation costs
- Complexity in mapping and standardizing data
Custom EHR integration is needed when healthcare organizations have complex workflows, use multiple legacy systems, or require specialty-specific features that standard integrations cannot support. It ensures flexibility and scalability tailored to unique operational needs.
EHR integration in healthcare enables specialty practices to connect tools specific to their domain, such as imaging systems for radiology or therapy management tools for behavioral health. This improves workflow efficiency and ensures accurate, context-specific patient data access.
Key technologies used in how electronic health record integration works include:
- HL7 and FHIR standards
- RESTful APIs
- Middleware and integration engines
- Cloud-based integration platforms
- Data transformation and mapping tools
Yes, electronic health record integration in healthcare systems can be secure and HIPAA-compliant when implemented with proper safeguards such as encryption, access controls, audit logs, and secure APIs. Compliance depends on following regulatory standards and best practices.
The timeline for EHR integration in healthcare varies depending on complexity. Simple integrations may take a few weeks, while custom EHR integration projects involving multiple systems and workflows can take several months.




