EHR Integration Process: From Requirements to Go-Live
Do you know that in the Electronic Health Record system, there are around 8-12% of duplicated patient records?
Yes, the huge amount of duplicated data often creates errors in clinical processes and, at times, even in administrative aspects. But that is not all, the most pressing problem, other than just duplicated data, is the unstructured data.
According to several citing sources, almost 80-90% of all healthcare data is still unstructured, compromising non-traditional data like video, audit, and text. This is the reason why we feel healthcare is stuck, or in simple terms, just a mess.
Upon digging deeper into these stats, one of the reasons why these healthcare practices fail is because of poor integration planning. You see, healthcare practices do know EHR integration, but due to poor planning, the transformation simply fails.
This is so crucial because the EHR integration process often involves a separate clinical and technical journey. And the aftermath of this directly impacts patient outcomes and care delivery operations. So, for proper planning of EHR integration, you need to know the EHR integration process.
On that note, let this blog be your EHR implementation guide, and let’s uncover some of the intricacies of clinical data integration, EHR integration workflows, and the EHR integration process.
So, without further ado, let’s get started!
EHR Integration Lifecycle: Step-by-Step Overview
First things first, let’s first understand or get familiar with the EHR integration lifecycle and all the steps that are involved in this. So, here are the 8 key phases that are usually involved in EHR integration:
- Requirement Gathering & Gap Analysis: This is the first step and lays the foundation for the entire process. Here, mostly you’ll identify business goals, define clinical workflows, and exchange needs. If you do this right, you will not have to rework this later.
- Team Setup & Resource Planning: Once you know what you have to do, the success of your integration depends on your team. Curate your team that has technical, clinical, and project management expertise.
- Strategic Approach (Build vs Buy): Depending on everything that you have done till here, now, it’s time to make a strategic decision, either to build custom integrations or use an interface engine or something like that. Remember, this decision should be made on factors like scalability, cost, timeline, and long-term flexibility.
- Architecture Design & Data Mapping: If you have decided to build custom integration, then at this stage you design the framework of how your systems will communicate and how the data will flow from one system to another. It includes selecting standards, integration methods, data mapping, etc.
- Development & Data Transformation: Once you’re done with the design, the development process begins. Here, interfaces are built, APIs are configured, and data is transformed to connect the systems and allow them to communicate with each other efficiently.
- Testing & Validation: Before deployment of the integration solution, you need to do one thing – test the integration bridge to ensure accuracy, reliability, and compliance. Some of the most important tests conducted here are unit testing, system integration testing, and user acceptance testing.
- Go-Live Execution: After successful testing, you finally deploy the integration in the production environment. In this stage, along with deploying, you also ensure minimal disruptions to clinical operations and include final data checks, system monitoring, and contingency planning.
- Post-Go-Live Optimization: Once the integration is deployed, you move on to the continuous monitoring phase. Here you monitor the performance of the integration, tune it whenever requirements change, and solve issues based on real-world usage. This is an ongoing process.
Apart from these lifecycle stages, here are a few things that you need to know when it comes to the EHR integration process.
- EHR integration workflow: The EHR integration workflow decides how data moves between systems and how they communicate and coordinate care. It is necessary so that your system can provide you with the right information, from the right system, at the right time.
- Data Flows Across Multiple Systems: When building an integration ecosystem, you need to ensure that the patient data flows between multiple systems, such as EHRs, laboratory systems, billing platforms, and other third-party applications.
- Real-Time vs Batch Processing: There are two modes in which EHR integration can operate, real-time or batch. While real-time processing enables instant exchange of data, the other one transfers data in bulk, typically used for non-urgent tasks.
What Makes or Breaks the EHR Integration Process

There are certain aspects in the EHR integration process that, if not handled correctly, can make or break your EHR integration. On that note, be careful about these and consider them before starting your EHR integration process:
- Data Silos & Fragmented Systems: Data silos and fragmented systems keep the data isolated from other systems. This is still the major problem for many clinics, and data silos can instantly break your EHR integration process.
- Legacy Infrastructure Limitations: If you’re still using legacy systems, then this infrastructure comes with certain limitations. This can stop your system from coping with the evolving needs, such as API-based data exchange, etc.
- Compliance & Security Risks: Non-compliance and insurance EHR integration bridge can not only lead to penalties, but it can disrupt your care delivery process immensely, which can have a direct impact on your practice.
- Resistance from Clinical Staff: Users often get comfortable with the system they are using. So, when shifting to a new one, certain clinicians can resist the change. That is why proper training is necessary for a smoother transition.
- Continuous Monitoring & Feedback Loops: Another problem that many practices ignore is monitoring the performance of their integration and not having any feedback mechanism to identify any gaps that are faced by end-users.
While there are some factors that can break your EHR integration process, there are certain factors that can even determine the success of your EHR integration process:
- Stakeholders Alignment: When your stakeholders are aligned with each other across clinical, technical and operational terms, all your needs become crystal clear, which makes the process much easier to implement and understand.
- Clear Governance & Ownership: Throughout the EHR integration life cycle, there should be clear governance and ownership so that no stone is left unturned.
- Accurate Mapping between Workflows & System Logic: Data mapping between different workflows must be done accurately, and the logic that runs between the system should be clear.
- Scalable Design: Have a scalable design so that you don’t have to rework the intricacies whenever there is a change.
- Continuous Monitoring Feedback Loops: Create a continuous feedback loop, so that when the end-users experience any problems, they can easily anticipate that, and continuous improvement in the bridge can be ensured.
Phase 1: Requirement Gathering & Gap Analysis
So, in the first step, which is the most important step in the EHR integration process. Here, you need to understand how clinical and operational workflows function. Furthermore, what do you want to achieve with this integration? It usually consists of identifying key data exchange requirements, user needs, and desired outcomes.
Here, the existing systems are audited to evaluate current capabilities, data structure, and integration limits. This will help uncover the gaps between legacy and infrastructure and modern interoperability requirements.
It is also at this stage that you curate the integration process by aligning it with necessary compliances and healthcare interoperability standards such as HIPAA, SOC 2, ONC, etc.
Last but not least, in this stage, you define the success criteria for this project and define KPIs, setting the strong foundation for all integration phases.
Phase 2: Team Setup & Resource Planning
The next phase is where you assemble the right team and ensure the necessary resources are in place so that execution is done exactly as planned. This is why roles are clearly defined, and the roles that are typically involved in this are project manager, integration engineers, QAs for validation, and stakeholders to ensure workflows align with real-world use.
This is also where practices must assess their internal capabilities. One of these should be standards like FHIR, HL7, and API-based integrations. Last but not least, establish a strong collaboration and governance model so that the team can coordinate and make decisions to build the EHR integration bridge.
Phase 3: Strategic Approach (Build vs Buy)
This is the strategic step, where you decide to build a custom EHR integration or rely on third-party applications. So, to help you make a better decision, refer to the table below:
| Criteria | In-House (Build) | Third-Party / Buy |
| Control & Customization | Full control over logic, workflows, and data handling | Limited to vendor capabilities and configurations |
| Time to Market | Slower (requires development from scratch) | Faster (pre-built connectors and frameworks) |
| Initial Cost | Higher upfront investment (team, infrastructure) | Lower upfront, often subscription-based |
| Total Cost (TCO) | Can increase over time (maintenance, upgrades) | Predictable but ongoing licensing costs |
| Scalability | Highly scalable if designed well | Depends on vendor’s scalability limits |
| Expertise Required | Requires strong knowledge of standards like FHIR and HL7 | Minimal internal expertise required |
| Maintenance Effort | Fully owned by internal team | Managed partially or fully by vendor |
| Flexibility for Future Integrations | High flexibility | May face limitations based on vendor roadmap |
| Risk Factors | Resource dependency, longer timelines | Vendor lock-in, less control over updates |
Phase 4: Architecture Design & Data Mapping
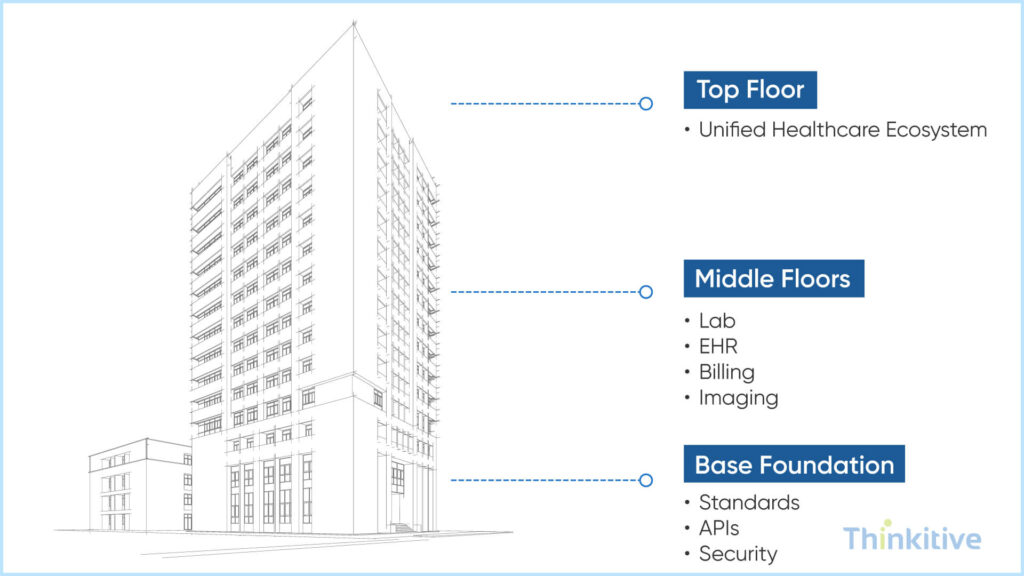
This is one of the most crucial stages in the entire EHR integration process. It is at this process that you decide how your systems communicate, how data flows, and how consistency is maintained across the ecosystem. You see, a well-designed architecture is something that ensures seamless interoperability but also supports scalability, performance, and future integration aspects.
The first step in this is to choose the right integration model. On that note, here are the three integration models that you need to choose from:
- Point-to-Point: In this type of model, direct connections between systems are established. It is simple to implement; however, if the number of integrations grows, then it can be quite difficult to manage and can lead to tight coupling and scalability issues.
- Hub-and-Spoke: In this model, a centralized hub is created that manages all the communications between your system and others. It reduces the complexity and also improves its maintainability. It is best suited for mid-sized healthcare organizations.
- Enterprise Service Bus (ESB): This is an advanced model, which is driven by a middleware architecture that enables standardized messaging, routing, and transformations. ESB supports high scalability and can be ideal for large healthcare organizations with complex integration needs.
When designing the EHR integration architecture, design it as a scalable healthcare integration architecture that can:
- Support API-first design
- Enable real-time and asynchronous communication.
- Align with interoperability standards like FHIR and HL7.
- Ensure high availability, fault tolerance, and performance optimization.
Here are some of the other intricacies that are involved in this phase:
- Data Mapping, Normalization & Semantic Consistency
Data mapping, data normalization, and ensuring semantic consistency in data are very important. You see, data mapping ensures that fields from one system correctly align with another.
Other than that, data normalization ensures that data formats across the systems are standard. While this ensures structural alignment of your system, there should also be semantic consistency so that the clinical meaning of the data remains consistent across systems.
This can be achieved using standardized terminologies such as SNOMED CT or LOINC. This reduces mapping errors, improves data usability, and supports accurate clinical decision-making.
- Handling Legacy System & Interoperability Gaps
Many healthcare organizations are still relying on legacy systems that lack modern APIs and standardized data structures. Due to this, your integration architecture may require custom interfaces of middleware, data transformation layers, etc.
Addressing these gaps in interoperability due to legacy systems can prevent bottlenecks and ensure smooth data exchange across systems.
Furthermore, you can leverage AI in data mapping and quality management, as it can automate certain processes and help you improve data quality.
Phase 5: Development & Data Transformation
In this stage, you bring the designed architecture to life. In this stage, you build interfaces, transform data, and establish and enable seamless communication between applications. And the main focus is on ensuring that data flows accurately, consistently, and in an understandable format at all times.
Here are some of the intricacies that are involved in this stage:
ETL Pipeline (Extract, Transform, Load)
The core of this phase depends on this pipeline process.
- Extract: Data is pulled from source systems such as EHRs, labs, billing, etc.
- Transform: The pulled data is cleaned, structured, and converted into a standardized format that your system can understand.
- Load: The transformed data is then delivered into the target system for use in clinical and operational workflows.
This phase is important because a well-designed ETL pipeline can ensure data integrity, minimize latency, and support both real-time processing and batch processing requirements.
Data Standardization & Transformation
Different healthcare systems store different data formats as per their requirements and interoperability standards. Most of the time, you would have to convert legacy formats into modern standards like FHIR or APIs, etc.
Some of the key things included in this are:
- Normalization of data structures and field formats
- Ensuring semantic consistency across systems
- Preserving clinical accuracy during transformation
- API & Integration Layer Development
The integration layer is basically a bridge that connects your system with the other system. Now, typically, this layer is built using RESTful APIs or middleware platforms. Now, this layer is responsible for data routing between different systems to their destination, authentication and authorization of data, and last message transformation and validation.
Error Handling, Monitoring & Reliability
There are bound to be errors in the data. That is why you need to implement robust error handling mechanisms to maintain system stability and data accuracy. Some of the critical aspects in this are:
- Dead Letter Queues (DLQs): This mechanism captures failed messages for later analysis and reprocessing of data.
- Retry Mechanisms: Automatically reattempt failed transmissions so that they can handle temporary issues.
- Monitoring & Alerts: Provide real-time visibility into integration performance and failures.
With these safeguards, data issues can be identified proactively and resolved quickly without disrupting clinical or operational workflows.
Phase 6: Testing & Validation Before Go-Live

This is another crucial phase of integration, where you test the integration for its reliability and accuracy so that the integration is ready for real-world use. There are various intricacies in the process, especially with validation, where you ensure that data flows correctly between systems without duplication, errors, and loss.
There are certain testing scenarios involved in this, which are as follows:
- Unit Testing: This is where each component of the EHR integration is tested individually.
- Interface Testing (Data Exchange between Systems): In this type of testing, the whole integration is tested to ensure that data exchange between systems is accurate, compliant, and complete.
- End-to-End Testing: This type of testing is done to ensure that the complete bridge is working as intended, along with verifying the complete workflow structure.
In all these testing cases, special attention to real-world clinical scenarios is given so that the integration supports the actual care delivery process. And lastly, the validations are done to minimize risks, prevent disruptions before you go-live, so that a smooth transition can be ensured into production.
Phase 7: Go-Live Execution & Hypercare
This phase starts when you completely test your EHR integration. This is the phase where you make the integration fully operational in real-world clinical environments. A well-planned go-live process can ensure minimal disruptions to workflows and ensure continuity of care.
There are two roll-out strategies that you can adopt, as given below:
- Big Bang: Here, all the systems in your integration are deployed simultaneously. It is much faster in implementation, however, and possesses a higher risk if any issues are encountered.
- Phased Rollout: In this rollout, gradual deployment by module, department, or location is planned. The advantage that you get with this is that it possesses minimal risk; however, it can be a lengthy process.
While you can adopt the strategies that suit your practice the best, you must also be aware of the steps involved in the Go-Live process. On that note, here are the most important steps involved:
- Pre-Flight (Backup & Validation): Final checks are performed, backups are created, and configurations are validated so that everything is in place before you go live.
- Cutover (Production Transition): In this step, systems are switched from testing environments to live environments. Data flows are activated, and integrations begin to operate in real-time.
- Validation (Early Monitoring): Initial transactions are closely monitored so that the performance of the integration can be measured. Here, data accuracy is verified along with workflow continuity, and any anomalies that can be fixed are fixed.
After you go-live, a dedicated hypercare period is agreed upon so that the system can be closely monitored and immediate support is provided, if needed. Teams actively track system performance, resolve issues in real-time, and assist end users for effective use.
Phase 8: Post-Go-Live Optimization & ROI
After the system is deployed, the focus is all on monitoring the performance of the integration. Here, workflows are optimized, and it is ensured that the integration meets its defined goals.
KPIs that are decided in the first phase are tracked regularly to ensure the success rate of the integration. Some of the core KPIs here are a reduction in duplicate diagnostic tests, faster clinical documentation, and charting time. Along with these, improved billing accuracy and quicker claim processing are also tracked to measure the impact.
However, some of the core aspects in the process are continuous monitoring, performance tuning, and user feedback loops so that the system evolves with evolving needs, which will automatically maximize ROI and be critical in long-term integration success.
Conclusion: Managing the Continuous Lifecycle
If you have made it this far, then I can be assured that you know almost all of the intricacies that are required for custom EHR integration. We have covered some of the most crucial aspects in this, which are the steps involved in EHR integration implementation.
Furthermore, you need to understand that integration is an ongoing process, and as progress is made and needs evolve, the EHR integration should also evolve. On that note, let this blog be your guide for a long-term EHR implementation guide.
And if you’ve already passed that phase, then get your free call and let’s discuss your EHR integration implementation.
Frequently Asked Questions
The EHR integration process, step by step, follows a structured approach that includes requirement gathering, system analysis, architecture design, data mapping, development, testing, go-live, and post-deployment optimization. This EHR integration lifecycle in healthcare ensures seamless data exchange across systems while maintaining compliance, accuracy, and performance.
The EHR integration process typically takes anywhere from 4 to 16 weeks, depending on system complexity, number of integrations, and data volume. Large-scale healthcare system integration processes involving multiple systems or legacy platforms may take several months to fully implement.
Key EHR integration requirements include clearly defined clinical workflows, interoperability standards (such as FHIR or HL7), data mapping strategies, compliance considerations, and a well-defined project scope. These elements form the foundation of a successful EHR implementation process.
The choice between in-house vs outsourced EHR integration depends on internal expertise, budget, and scalability needs. In-house development offers greater control and customization, while outsourced solutions accelerate implementation and reduce operational burden. Many organizations adopt a hybrid approach for optimal flexibility.
In a Big Bang approach, the entire system goes live at once, offering faster deployment but higher risk. A phased rollout introduces integrations gradually, reducing risk and allowing better control. The choice depends on the organization’s readiness and the complexity of the EHR integration workflow.
An EHR integration workflow defines how data flows across systems such as EHRs, labs, billing, and third-party applications. It includes data capture, validation, transformation, and transmission—ensuring seamless clinical data integration and consistent patient records across the ecosystem.
Common challenges in the EHR integration lifecycle in healthcare include legacy system limitations, inconsistent data formats, interoperability gaps, and integration complexity. These can be mitigated through standardized data models, robust architecture design, thorough testing, and adherence to interoperability frameworks.
EHR integration testing is conducted in sandbox or staging environments that replicate real-world scenarios without impacting live systems. This includes unit, interface, and end-to-end testing, along with validation of clinical workflows to ensure safe deployment during the EHR implementation process.
Hypercare is a dedicated post-go-live support phase where teams closely monitor system performance and resolve issues in real time. It is critical to ensure stability, minimize disruptions, and support users during the early stages of the EHR integration process.
EHR integration ROI is measured using KPIs such as reduced duplicate tests, improved clinical efficiency, faster documentation, and enhanced billing accuracy. These metrics help quantify the value delivered by the healthcare system integration process.
The best model depends on scale and complexity. Point-to-Point works for simple setups, Hub-and-Spoke suits mid-sized environments, and ESB is ideal for enterprise-level EHR integration processes requiring scalability, flexibility, and centralized control.
AI enhances clinical data integration by automating data mapping, identifying patterns, and detecting anomalies in datasets. This reduces manual effort, improves accuracy, and accelerates the overall EHR integration process.
Key KPIs include data accuracy rates, system uptime, reduction in duplicate tests, documentation time, and billing efficiency. Tracking these metrics ensures continuous improvement and helps maximize EHR integration ROI after deployment.




