How Much Does EHR Integration Cost? Complete Pricing Breakdown 2026

The need for EHR integration for healthcare practices has grown exponentially over the last few years. You see, as EHR systems slowly became the epicenter of care delivery in modern healthcare, the need for having your system part of a connected ecosystem became even more evident.
And given the intricate nature of the EHR integration landscape, EHR integration pricing looks completely different from what it was a few years ago. It moved from being a relatively predictable, interface-based model into a more dynamic and architecture-driven model.
Earlier, healthcare providers looking for EHR integration would be charged per interface; today, the EHR integration cost is decided by APIs, interoperability mandates, and the complexity of the healthcare ecosystem.
You see, modern EHR systems are built around interoperability standards like FHIR, which enables faster and more flexible integration capabilities. Moving away from the HL7 interface, which relied heavily on customization.
This shift was not only because of the evolving nature of EHR systems but also because the API-first architecture simply reduced development time and improved scalability aspects.
Talking about fixed price, in 2026, the EHR integration cost is not fixed; it depends heavily on systems, data, system complexity, APIs, compliance, etc. This might hint towards the high EHR integration cost, right?
Well, not technically. It is true that any healthcare data integration cost can be higher, but if you know the right way to approach it, you can significantly reduce the cost or plan your EHR integration budget accordingly.
On that note, let’s uncover the hidden costs of EHR integration along with factors that affect the price significantly. And while we’re at it, we’ll also try to find ways in which you can lower the EHR integration cost.
So, without further ado, let’s get started!
How Much Does EHR Integration Cost in 2026?
If you go searching for EHR integration vendors and even request a quote, then one thing that would be distinct is the estimated cost given to you.
While this might be surprising for many, in 2026, EHR integration costs are indeed highly variable. Some of the factors driving them are system complexity, data volume, interoperability standards, and overall architecture.
Unlike traditional EHR integration pricing models, modern integrations have shifted towards dynamic pricing, where the cost is calculated by how deeply systems need to communicate in real time.
Still, to give you an idea about the EHR integration cost based on the EHR integration levels, here is a table for your quick understanding:
| Integration Level | Cost Range | What’s Included | Best For |
| Basic Integration | $5,000 – $15,000 | Single API connection, read-only data access, minimal transformation | Small clinics, simple data retrieval use cases |
| Mid-Level Integration | $15,000 – $30,000 | Bi-directional data exchange, multiple endpoints, moderate data mapping & validation | Growing practices, multi-system connectivity |
| Complex Integration | $30,000+ | Multi-system interoperability, real-time workflows, advanced logic, compliance layers | Hospitals, enterprise healthcare systems |
Note: Even within these ranges, the cost can vary depending on factors like data complexity, real-time requirements, and the interoperability standards that you’re using.
Furthermore, because of the standards and type of integration, the cost can also vary significantly. On that note, here is a brief pricing overview based on different types of integrations:
| Integration Type | Typical Cost Impact | Development Effort | Maintenance Cost | Flexibility | Best Use Case |
| HL7 (Legacy Standard) | Medium to High | High (custom message parsing & mapping) | High (ongoing updates & fixes) | Low | Legacy hospital systems, older EHR platforms |
| FHIR (Modern Standard) | Medium | Moderate (standardized REST APIs) | Low to Medium | High | Modern EHRs, scalable and interoperable systems |
| Custom API-Based Integration | Variable (Low → High) | Variable (depends on API quality) | Medium | Very High | Custom apps, patient portals, AI tools, unique workflows |
Core Components of EHR Integration Pricing
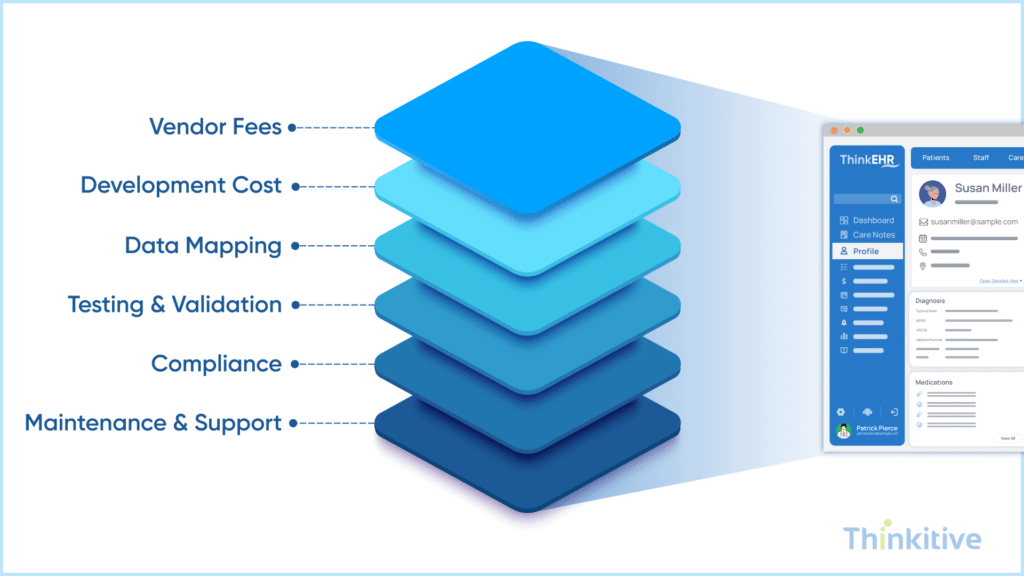
System-to-system connection is not the only factor that influences your EHR integration. And you probably know that by now. There are multiple factors, such as technical, operational, and compliance components. On the basis of these, EHR integration cost layers help you estimate budgets more accurately and avoid any surprises during implementation.
On that note, here are the core components of EHR integration pricing that you need to know to determine the pricing:
- Vendor Fees: EHR vendor systems like Epic, Cerner, or Athenahealth often charge for API access or interface licenses, Sandbox environment, or data extraction. These fees are usually fixed or subscription based or usage based. This depends on the vendor.
- Development & Engineering Effort: Development or engineering of the EHR integration bridge is the major factor that impacts the cost. Some of the core activities in this include building interfaces with HL7, FHIR, and APIs. Here, the backend logic is applied, and workflow automation is developed so that data sharing is accurate and precise. Last but not least, error handling and retry mechanisms are also deployed so that you can have multiple chances for sharing data. Costs of this phase are directly proportional to the number of systems and workflows.
- Data Mapping & Transformation: Healthcare data are rarely standardized across systems. So, converting this data into a standardized format comes with a cost. Some of the core steps involved in this were mapping fields between systems (e.g., patient records, lab results, etc.). This is followed by converting formats (from HL7 to JSON or FHIR), along with handling inconsistencies and missing data. This component is crucial because poor data mapping can lead to clinical errors.
- Testing & Validation: Before going live, the integrations need to be rigorously tested, just to ensure that data is being shared effectively, accurately, and in real-time. Having said that, some steps included in this are interface testing, such as data accuracy or completeness. After that, workflow validations must also be tested, this is where end-to-end scenarios come into play and last but not least, performance and load testing is conducted for the bridges sustainability.
- Deployment & Ongoing Maintenance: After going live, you still have to pay for production deployment and monitoring, version upgrades (EHR updates, API changes), bug fixes, and performance optimization. You see, some studies even suggest that ongoing maintenance can cost up to 15-20% of the initial development annually.
- Compliance & Regulatory Costs: Your healthcare integration must meet strict regulatory standards like HIPAA or ONC. The factors that influence costs here are encryption and access control implementation, audit logs and monitoring systems, and security testing and risk assessment.
Note:EHR integration pricing is a combination of technology, vendor dependencies, and regulatory requirements. These components must be addressed proactively; ignoring them can lead to project delays and even budget constraints.
Key Factors that Influence Integration Costs
Now, this subheading might confuse you, but there is a thin line that you need to understand. Like the core components define where the money goes, however, the factors that determine the price will be determined by the factors that we will be discussing further.
On that note, let’s get started:
- System Complexity & Workflow Requirements
Let’s get this straight: the more complex your workflow is, the higher the cost will be. For example, if your integration requirement is simple and limited to only pulling patient demographics, the cost will be less. However, if you require real-time care coordination across various systems like EHR, labs, billing, and patient apps, then the workflow would require custom logic, event-driven architecture, and real-time process.
This is one of the, if not the, major factors that directly increase development and testing efforts, in short, the EHR integration cost.
- Number of Integrations & Endpoints
Your system will hardly be connected to just one system. Having said that, with each new additional system, you have to add new interfaces, map more data, and increase testing scenarios. Now, let’s see how it influences costs. For example, if you just need to integrate with 1 or 2 systems, the cost can be predictable, but as the number of systems for integration increases, the complexity also increases, along with endpoints, which scales the EHR integration cost rapidly.
- Data Volume & Transformation Needs
Every type of data in healthcare is different. And healthcare being the largest producer of data, it needs to be treated and transformed so that it can be shared and used. But the way it increases cost is when the data volume is large, consisting of images, historical data, etc.
Along with that, complex data formats and data normalization requirements increase the cost simultaneously. A simple way to remember this is by understanding that the more data you have, the more you have to spend on processing, storing, and validation, all factors that only increase your EHR integration costs.
- Security, Compliance & Regulatory Requirements
For security purposes, you have to adhere to strict compliance standards like HIPAA for data privacy and security, and other guidelines from the Office of the National Coordinator for Health Information Technology.
Now, when your vendor says that your EHR integration project has higher security requirements, it can roughly translate to encryption levels, role-based access control, audit logs, and monitoring mechanisms.
EHR integration costs aren’t linear, meaning they won’t gradually increase. In fact, depending on the complexity of your system, it scales. And that same logic can be observed across systems. For instance, when you decide to add one more system for integration, the cost doesn’t just add or double, but it multiplies. Since with one system integration you have to deal with data relationships, workflow dependencies, and failure scenarios, the compounding effect can be easily felt.
Hidden Costs of Integration Projects
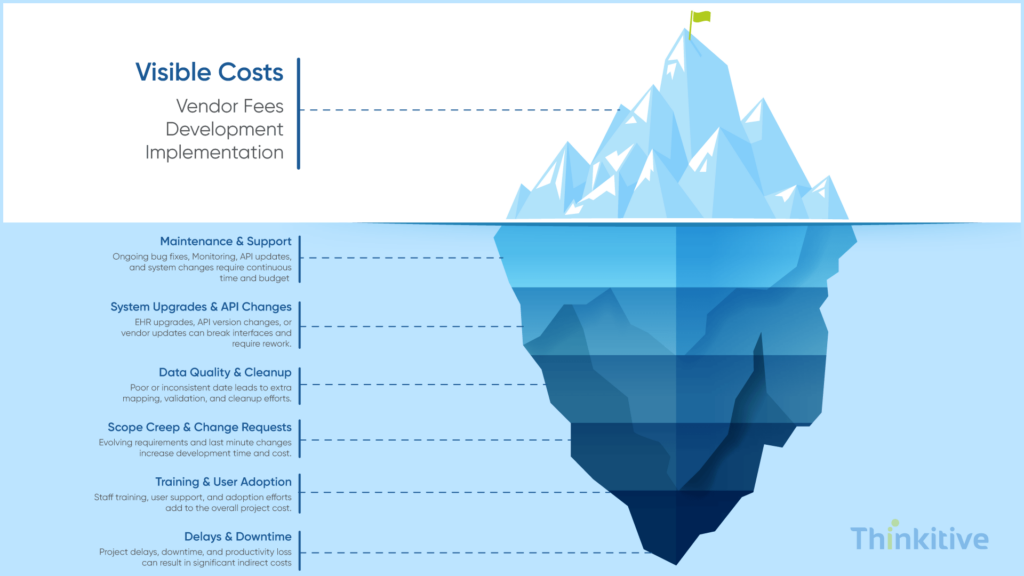
If you’ve made it this far, then you must think that your EHR integration budget will only include process requirements for development and deployment. However, this is just the tip of the iceberg. You see, the hidden cost of your project can increase the total cost of ownership if not planned.
On that note, here are some of the hidden costs that you need to consider for your EHR integration project:
- Ongoing Maintenance & System Updates
Once you go live with your integration, your system will have to continuously monitor it. Other than that, fixing bugs and data synchronization issues, adapting to the EHR updates, and performance monitoring and optimization will typically take up the EHR integration cost by 15-20% of the initial development annually.
- API Version Changes & Vendor Dependencies
As you know, modern systems majorly depend on API-based integrations based on FHIR standards. Now, these APIs evolve and adhere to these costs for every version upgrade, vendors increasing endpoint integration costs, and rework and testing that comes with it will indeed impact the cost.
- Internal Team Costs & Training
You may be dependent on external vendors for development, but your internal team still needs to understand integration workflows, handle basic troubleshooting prospects, and train staff on new processes. Now, to make your team efficient in these processes, you have to conduct training sessions, handle productivity dips during transition, etc. And all these processes come bearing a cost.
- Delays Due to System Incompatibility
You are responsible for your system, but you can’t do anything about external systems that are out of your control. In such cases, if the system is not integration-ready, then issues like legacy systems lacking modern APIs, poor documentation prospects, and data inconsistencies can delay the integration process. This can lead to delays, increased development hours, and even the need for additional middleware or custom solutions, and as usual, all these come bearing a cost, increasing your EHR integration costs.
- Long-Term Scalability & Upgrade Costs
Scalability is something that every organization needs to prepare itself for tomorrow. And as your organization grows, new systems will be added, existing integrations will need upgrades, and there will be a gradual increase in data volume and complexity. In such cases, without a scalable architecture, you will have to rebuild the architecture, resolve performance bottlenecks, and re-engineer the bridge, increasing the EHR integration pricing with new updates or upgrades.
The hidden costs of EHR integration can be overwhelming at times, but remember that they are not an option but inevitable. The best way to overcome these challenges is by anticipating and planning for them in advance. And the best time to start—if you’ve not yet—is now.
Cost Comparison by Integration Type (HL7 vs FHIR vs APIs)
In 2026, choosing the right integration approach has become a deciding factor for almost all integration projects. And for good reasons, as it directly impacts the cost, scalability aspects, and long-term ROI.
In the current landscape, the shift from legacy standards to an API-first ecosystem has already created a difference in how EHR integration costs vary. On that note, here is a brief table for cost and culpability comparison of EHR integration type or approach:
| Factor | HL7 (Legacy) | FHIR | Custom APIs |
| Initial Cost | Medium → High | Medium | Low → High (variable) |
| Development Effort | High (custom parsing, mapping) | Moderate (standardized REST APIs) | Variable |
| Maintenance Cost | High | Low → Medium | Medium |
| Vendor Dependency | High | Medium | Depends on API provider |
| Real-Time Capability | Limited | Strong | Very strong |
| Scalability | Low | High | Very High |
| Flexibility | Low | High | Very High |
Legacy vs Modern Integrations: Cost Differences
Depending on what system you use, the cost again fluctuates. Here is a quick breakdown of the cost differences between them:
- HL7 Integrations: These integrations often require custom message handling, interface engines, and continuous maintenance. So, due to the specific intricacies of this, despite having a familiar infrastructure, the long-term cost will be quite higher.
- FHIR-Based Integrations: These integrations typically use standardized APIs and enable faster scaling. Being set up in a modern ecosystem, the development lifecycle costs will be significantly lower, and the ROI has been rewarding for practices.
- Custom APIs: When it comes to flexibility, no integration comes close to custom APIs, and the best part is that the cost depends completely on implementation quality. So, depending on the scope of your EHR integration, the cost can be economical or costly.
Vendor Fee Variations Across Platforms
The fees charged by the EHR vendors like Epic Systems or Oracle Cerner often influence EHR integration costs with:
- API access pricing
- Interface licensing
- Transaction-based fees
Most of the vendors are FHIR-friendly, but some still rely on HL7, and this factor alone impacts cost, time, and effort.
Real-Time vs Batch Processing: Cost Implications
Here’s a brief cost comparison between real-time and batch processing integrations:
| Factor | Real-Time Processing | Batch Processing |
| Cost | High (development + infrastructure) | Low to Moderate |
| Implementation Complexity | High (event-driven architecture) | Low (scheduled jobs) |
| Data Availability | Instant / near real-time | Delayed (minutes to hours) |
| Use Cases | Clinical workflows, alerts, patient monitoring | Reporting, analytics, non-critical data sync |
| Scalability Needs | High (continuous data flow) | Moderate |
| Maintenance Effort | Higher (monitoring, uptime requirements) | Lower |
Real-World Pricing Trends in 2026
Given the shifting winds in healthcare technology, there is a swift shift observed from HL7-only implementation to API-first and FHIR-based ecosystems. Due to this, there is an increase in investment for EHR integration projects for:
- Real-time data exchange
- Scalable integration architecture
- Automation and monitoring tools
This trend clearly indicates that healthcare organizations are willing to spend more upfront for lower long-term integration costs and improved scalability.
Justifying the Investment: Cost vs Value
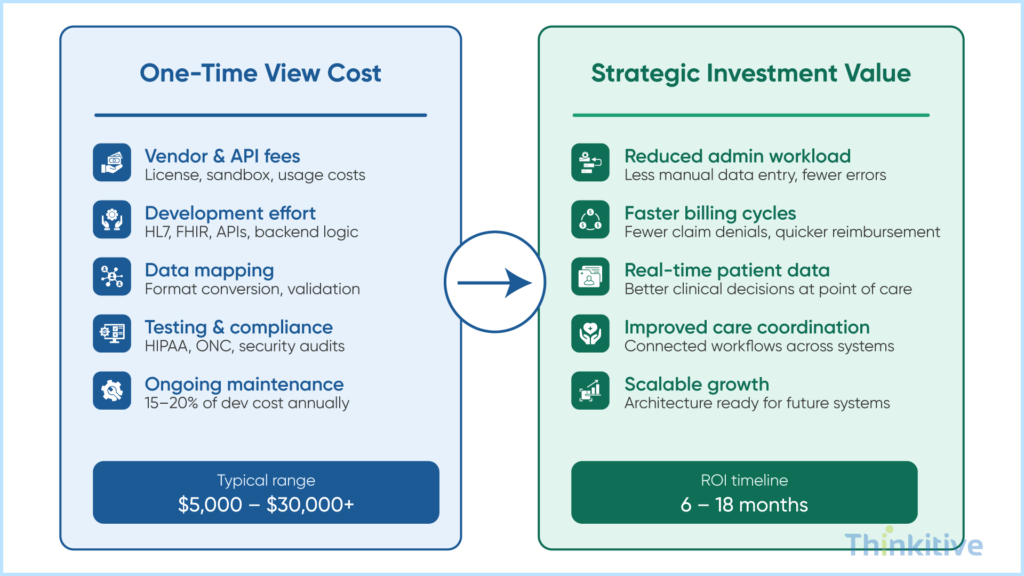
By this point, you must have realized that EHR integration does not require a small investment. However, given the several intricacies, relying on just the cost can be harmful. This is the reason why a shift is seen in healthcare organizations’ attitude toward EHR integration, where the focus has shifted from cost to value.
First things first, do not treat EHR integration as a one-time expense; rather, look at it as a strategic investment that drives operational efficiency and empowers care delivery processes. With this shift, you will be making your system smarter and prepared for future challenges.
Another aspect that you need to focus on is linking your integration costs to business and clinical outcomes. For instance, to reduce administrative workload, real-time access to patient data can be crucial. Furthermore, for faster billing cycles and fewer claims denials, improved care coordination is required.
See, the value the integration is adding to the practice’s main business goals becomes clear, and the major factor in this has been connected and accessible data.
How to Reduce Integration Costs Without Compromising Quality
As promised earlier, let’s see if you can reduce the total EHR integration cost without compromising on the quality. So, let’s see how you can do it:
- Prioritize High-Impact Integrations First: Understanding that not all integrations deliver equal value. So, focus on integration that is most important, like systems that drive revenue (billing or RCM), or the system on which your care delivery or clinical workflow depends, or on systems that have high-frequency data exchanges.
- Use Standardized APIs & Frameworks: Modern standards like FHIR reduce both development and maintenance efforts. These standardized APIs and frameworks lead to faster implementations, lower customization needs, and easier scalability, making your entire project cost-effective in the long run.
- Avoid Rework Through Proper Planning: Poor planning is one of the biggest cost drivers, and you need to prevent that. Clearly define the integration scope and workflow. Along with that, keep your system audit ready so that it can be monitored, and align your needs with those of the stakeholders so that no stone is left unturned.
- Optimize Resources with Automation & Tools: Ever since the arrival of AI, many processes can be automated, which can reduce both development and operational costs significantly. For example, you can use automated testing tools for testing integration bridges, AI-assisted data mapping for mapping data, and monitoring and alerting systems to keep an eye on your system. These processes will reduce manual effort, reduce errors, and lower long-term maintenance costs by a margin.
Cost optimization in EHR integration is about making the process smarter. Prioritize the right integrations, leveraging the right standards, and by minimizing reworks, the EHR integration cost can be reduced significantly without compromising on quality.
Conclusion
You have made the decision of EHR integration to support your practice; now, don’t look at this venture as a cost, but as a strategic investment. However, if you have been reading this, then you know that for successful EHR integration, you have to balance cost, budget, scalability aspects, and long-term value of your investment.
So, make informed decisions for sustainable healthcare growth and let this blog be your guide to determine and negotiate the right price for your EHR integration project. On that note, get your system assessment for EHR integration with our experts, and book your consultation.
Frequently Asked Questions
The EHR integration cost in 2026 typically ranges from $5,000 to $30,000+, depending on complexity. Basic integrations fall on the lower end, while multi-system, real-time integrations can exceed $30K. If you’re wondering how much does it cost to integrate with an EHR in 2026, the answer depends heavily on scope, data flow, and system architecture rather than a fixed price.
The most important EHR integration cost factors include:
- System complexity and workflows
- Number of integrations and endpoints
- Data volume and transformation needs
- Compliance and security requirements
These factors directly impact overall EHR integration pricing, making each project unique.
The average cost of HL7 and FHIR integration varies based on implementation:
- HL7 integrations: Typically fall in mid-to-high ranges due to custom development and maintenance
- FHIR integrations: More cost-efficient in the long run due to standardized APIs
While the initial EHR integration cost may be similar, FHIR usually offers lower lifecycle costs.
An EHR vendor integration fees breakdown typically includes:
- API access or interface licensing
- Sandbox/testing environment fees
- Data usage or transaction-based costs
These EHR vendor integration fees vary by platform and can significantly impact total EHR integration pricing.
Healthcare data integration cost increases with system complexity. Simple integrations with one system are predictable, but adding multiple systems creates exponential cost growth due to:
- Increased data relationships
- More testing scenarios
- Higher maintenance needs
EHR integration pricing typically includes:
- Development and engineering
- Data mapping and transformation
- Testing and validation
- Deployment and monitoring
- Compliance and security implementation
A complete EHR integration cost should account for both initial and ongoing expenses.
The most common hidden costs of EHR integration include:
- Ongoing maintenance (15–20% annually)
- API version updates and rework
- Internal training and support
- System incompatibility delays
Ignoring these hidden costs of EHR integration can lead to budget overruns.
To build an accurate EHR integration budget, organizations should:
- Define integration scope and priorities
- Evaluate all EHR integration cost factors
- Include vendor fees and maintenance
- Plan for scalability and future integrations
A well-planned EHR integration budget reduces unexpected costs.
You can reduce EHR integration cost by:
- Prioritizing high-impact integrations
- Using standardized APIs like FHIR
- Avoiding rework through proper planning
- Leveraging automation tools
These strategies optimize EHR integration pricing without sacrificing performance.
EHR integration cost is not one-time—it’s an ongoing expense. Beyond initial development, organizations must account for:
- Maintenance and updates
- Vendor API changes
- Scaling and performance optimization
This makes long-term planning essential for accurate EHR integration pricing.
Most organizations start seeing ROI within 6 to 18 months, depending on implementation scale. ROI comes from:
- Reduced manual work
- Faster workflows
- Improved billing efficiency
The timeline varies based on healthcare data integration cost and implementation strategy.
There is no one-size-fits-all answer, but generally:
- HL7: Higher long-term costs due to maintenance
- FHIR: Balanced and scalable (most cost-effective for modern systems)
- APIs: Highly flexible but cost varies widely
Choosing the right approach depends on your use case, but modern standards often provide better long-term EHR integration pricing outcomes.




