EHR Integration Requirements: What to Prepare Before Starting

The success rate of integration projects is barely at satisfactory levels. According to this Medium Article, almost 84% of the digital transformation projects fail, and the majority of them are related to EHR integration.
Now, one of the major reasons why these healthcare integration projects fail is not because of these healthcare IT professionals’ inefficiencies. However, most projects fail even before they start.
You see, if we go by stats, then Standish Group’s CHAOS Report reported that only 31% of the total IT projects are completed on time, within budget, and with full score. This vaguely points towards the problem, and it’s not technology, but insufficient preparation.
This claim can be supported by this study by IBM, which highlighted 60% of project defects originate from poorly defined requirements.
On that note, let’s look beyond the technical aspects of the project and how clinical workflows, data standards, security policies, and operational processes will coordinate the success of your EHR integrations.
But here you might ask, why is defining EHR integration requirements so important?
Well, you see, when you don’t clearly define requirements upfront, even the most admirable projects can lead to delays, rework, and unexpected costs.
So, let’s try to understand the EHR integration planning process and curate an EHR integration checklist before implementation.
Core EHR Integration Requirements Framework
Before directly diving deep into the requirements, let’s first try to categorize and fit these requirements into a framework that lets us define the entire EHR integration scope. So, after delivering such projects for years, here is a near-perfect framework that every project follows:
- Business & Clinical Requirements: These requirements form the core of your project. In this, you define what the integration should achieve; some of the core aspects that are involved in this are clinical workflows, user needs, business goals, etc. In short, integrations that involve care delivery, billing efficiency, or patient experience come under this.
- Technical Requirements: Once your core requirements are clear, you move on to the technical requirements to achieve your business and clinical integration requirements. This is also important because here you define how the integration will work. Some of the core aspects covered in this are system architecture, APIs, infrastructure, performance expectations, and compatibility with existing systems.
- Data & Interoperability Requirements: Integration is nothing but connecting your system with others. However, in order to help your system understand the other system’s language, interoperability needs to be achieved. In short, with these requirements, you specify what data will be exchanged and how. It includes deciding data formats, mapping rules, data quality, and real-time vs batch exchange needs.
- Security & Compliance Requirements: Given the sensitive nature of the data that you deal with, you need to ensure that the data is protected and that you adhere to the regulatory needs. Some of the requirements of this step are HIPAA compliance, access controls, encryption, audit trails, and risk management.
- Operational & Governance Requirements: By addressing these requirements, you define how the integration will be managed ongoing, including roles, responsibilities, change management, monitoring support processes, and decision-making structures.
Technical & Healthcare System Integration Requirements
The intricacies of the technical and healthcare systems can be confusing at times. And the requirements need to be addressed with special attention. So, here are some things that you need to do to take proper requirements:
- Infrastructure Audit (Servers, Cloud Readiness, Network Capacity): The first step here for mapping its requirements is to assess whether your current system infrastructure can support integration. Some of the key aspects to address in this are server performance, cloud capabilities, bandwidth, and system scalability.
- Connectivity Standards (HL7 v2, FHIR, DICOM): Once you know the inside outs of your technical infrastructure, you need to identify which healthcare data standards your system would majorly benefit from for seamless communication between platforms. This is crucial for avoiding any data format conflicts that might be present.
- API Readiness & Vendor System Compatibility: After connectivity standards are confirmed, you need to focus on the data exchange. Here, evaluate whether your EHR and third-party system offer reliable APIs. Along with that, check whether your integrations require heavy customization or vendor limitations.
- Mapping Technical Requirements: Last but not least, align your integration needs with your current technological environment. This way, you get a clear idea about your system’s compatibility, things you need for minimizing disruptions, and identifying gaps that require upgrades or customizations.
Data Governance & Clinical Requirements
Given the attacks on healthcare software systems in recent times, during the planning or discovery stage of your integration, data governance and clinical requirements must be on your EHR integration checklist. Here are some intricacies that you must keep in mind:
- Data Scoping (Lab, Prescriptions, Imaging, Patient Records): First things first, defining which data sets will be exchanged between the two connected systems. Here, you need to ensure all relevant clinical and administrative data is included without putting an extra load on the system.
- Data Standardization (ICD-10, SNOMED-CT): Once data is defined, you need to align that data with the standardized medical coding systems. This is one of the core requirements as it defines the consistency in data, enables interoperability, and allows your system to understand data for accurate clinical interpretations across platforms.
- Data Quality, Cleansing & Normalization: After the data is standardized, it needs to be prepared for reliable outcomes and to prevent integration issues. In this, what I mean by preparing is that you need to remove duplicate records, correct errors, and standardize the format to help your system for better connectivity and communication.
- Ensuring Consistency & Accuracy Across Systems: The last box you need to check in this is by establishing rules and validation checks so that data remains synchronized, accurate, and consistent across all the systems that are part of the ecosystem.
Clinical Workflow & Operational Readiness
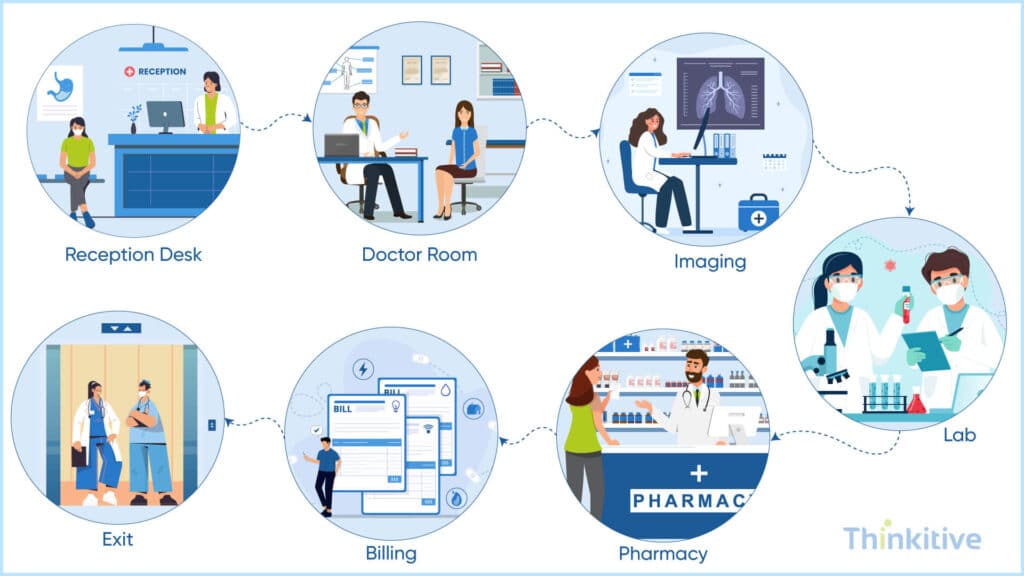
When mapping your requirements, many changes will often be associated with clinical workflows. Along with that, if your system is ready for other operations, then the entire healthcare system integration requirements can change. On that note, let’s see what you need to keep in your check for this:
- Mapping Real-World Clinical Workflows to System Logic: The very first thing on top of your checklist should be the translation of day-to-day clinical processes into system workflows. This is to ensure the integration you’re trying to achieve does support how you deliver care.
- Identifying Workflow Gaps Before Integration: After mapping your workflows and aligning them with your system, recheck the workflows. Try to find inefficiencies, redundancies, or steps that you might have missed. This is a crucial thing so that you can avoid disruptions and rework when the integration is live.
- Aligning Care Delivery Processes with Digital Systems: Once everything is done, align your systems workflows and check how the data flows in your system. Cross-check that with your care delivery process and ensure that they both align and synchronize with each other perfectly.
- Stakeholder Alignment Across Clinical, Administrative & IT Teams: The last thing you need to do in this step is to bring all the stakeholders of your practice on the same page. Since all these people are the ones using the software, you need to ensure all their requirements are covered in the integration, and everything they want is accurate, aligned, and runs smoothly.
Security, Compliance & Privacy Guardrails
The healthcare industry is one of the most highly regulated industries in the world. And as it nears completing its digital transformation arc, the security and compliance landscape is evolving. On that note, here are some of the things that you need to keep in your EHR integration requirement checklist:
- HIPAA, BAAs & Regulatory Requirements: Some of the core security and regulatory compliances that you need to align with are HIPAA. Ensure that your integration meets all the application regulations. These typically include patient data protection standards, formal agreements with the vendors, and whoever is handling your patient health information.
- Role-Based Access Control & Data Permissions: This is one of the best security aspects that you need to check from your checklist, which is role-based access control. This is crucial because it defines who can access what data based on roles to prevent unauthorized access and maintain the privacy of the patient.
- Audit Trails & Monitoring Requirements: Your systems will be dealing with a lot of data, and that too a lot of different types of data from various sources. That is why you plan to implement a tracking mechanism to log system activity, detect anomalies, and support compliance reporting.
- Data Protection & Encryption Standards: The last checklist you need to tick off is protecting your data at all times by using encryption standards. In simple words, you need to secure data both in transit and at rest using strong encryption and security protocols to minimize breach risks.
Common Mistakes in EHR Integration Planning
Most practices start their integration journey without properly defining their requirements. You see, they only need one integration, and they end up going for complete transformation. But despite having a reliable partner, many practices still commit critical mistakes during planning.
On that note, here are some of the common mistakes that you need to avoid in EHR integration planning, and how you can overcome them:
| Mistake | Impact on Integration | Recommended Solution |
| Starting integration without clearly defined requirements | Leads to scope creep, frequent changes, rework, and increased project costs and timelines | Define clear business, clinical, and technical requirements upfront with documented scope and success criteria |
| Ignoring data quality and standardization issues | Causes data mismatches, inconsistencies, and unreliable clinical and operational outputs | Perform data cleansing, normalization, and adopt standard coding systems before integration |
| Underestimating compliance and security requirements | Increases risk of regulatory violations, data breaches, and costly legal consequences | Incorporate compliance checks early, implement strong access controls, and follow encryption best practices |
| Lack of stakeholder communication and alignment | Results in misaligned goals, delays in decision-making, and poor user adoption | Establish cross-functional collaboration with regular communication between clinical, admin, and IT teams |
EHR Integration Checklist Before Implementation
Now that you know almost everything that is required for planning the discovery phase of your EHR integration, here is the final checklist that should be your guide for the EHR integration project:
| Checklist Item | What It Involves | Why It Matters |
| Stakeholder alignment (clinical, technical, leadership) | Ensuring all key teams agree on goals, workflows, and priorities | Prevents miscommunication, delays, and misaligned expectations during implementation |
| Vendor coordination and sandbox access | Working with vendors to enable testing environments and API access | Allows safe testing, faster issue resolution, and smoother integration rollout |
| Documentation of all requirements and workflows | Clearly documenting technical, clinical, and operational requirements | Reduces ambiguity, minimizes rework, and keeps the project on track |
| Infrastructure and system readiness validation | Verifying systems, servers, and networks are ready for integration | Avoids performance issues, downtime, and last-minute technical blockers |
| Timeline planning and milestone definition | Defining project phases, deadlines, and key deliverables | Ensures structured execution, better tracking, and timely completion |
Conclusion: From Requirements to Execution
Requirements for EHR integration depend on your needs, and these requirements depend on different aspects of your practice. Right from business and clinical requirements to data and integration requirements, every aspect must be carefully taken into consideration.
Only when this is done right can you successfully complete your EHR integration without many deviations. And in this way, you can be among the few who have bypassed the 84% integration project failures.
Having said that, it’s always good to prepare better; only when you do that can you successfully implement your EHR integration project. And if you need integration for your practice, then start your transition today, and get your consultation from experts.
Frequently Asked Questions
The core EHR integration requirements include defining business and clinical goals, assessing technical infrastructure, preparing data standards, ensuring security compliance, and aligning stakeholders. A well-structured approach helps organizations clearly understand what to prepare for EHR integration and reduces risks during implementation.
Organizations should evaluate servers, cloud readiness, and network capacity while ensuring systems can handle integration workloads. API readiness involves verifying that existing platforms support secure and scalable data exchange. These technical requirements for healthcare system integration are essential to avoid performance issues and compatibility challenges.
The first step is auditing infrastructure, connectivity standards (such as HL7 or FHIR), API capabilities, and system compatibility. These technical requirements for healthcare system integration help identify gaps early and ensure your existing IT environment can support seamless integration.
EMR integration planning for small practices is typically simpler, focusing on fewer systems and limited workflows. In contrast, large hospital systems require complex coordination across multiple departments, higher data volumes, stricter compliance measures, and more advanced healthcare system integration requirements.
A standard EHR integration checklist before implementation includes stakeholder alignment, vendor coordination, documentation of workflows, infrastructure validation, and timeline planning. Following a structured EHR integration checklist ensures all critical areas are addressed before starting the project.
Key EHR implementation requirements for HIPAA compliance include role-based access control, data encryption, audit trails, secure data exchange, and Business Associate Agreements (BAAs). These safeguards ensure patient data is protected throughout the integration process.
Data quality issues are identified through audits, profiling, and validation checks across systems. Resolving them involves data cleansing, normalization, and standardization using clinical coding systems. Addressing these early is a critical part of EHR integration requirements and ensures accurate, reliable data exchange.
Common mistakes include unclear requirements, ignoring data standardization, underestimating compliance needs, and poor stakeholder alignment. Avoiding these issues is essential when defining healthcare system integration requirements and following a structured EHR integration checklist.




