The Future of EMR Software
As technology has penetrated the core of the healthcare industry, it has moved from paper-based recordkeeping to digital recordkeeping. And as the winds of AI dominate the world, it is slowly transitioning to intelligent systems with analytics and other AI-powered features.
At the helm of this healthcare software systems’ transition is EMR, since it has found itself at the epicenter of healthcare practices. When talking about the future of healthcare, we have to mention something about the future of EMR software. And for good reasons, you see, the usage of AI and other systems has become massive in healthcare lately.
For instance, 2 in 3 physicians are using predictive AI in their healthcare systems. Statistics show a significant increase, with 71% of non-federal hospitals adopting these systems, according to the American Medical Association.
Furthermore, technology is incomplete without mobile, and the impact of mobile technology on EMR has also been phenomenal. It has, in short, given new direction to not only care access but also care delivery. According to SAGE Journals, more than 90% of physicians own and use smartphones in clinical settings, improving access to healthcare tools and data.
The same is seen across the industry as the use of AI tools in healthcare has reportedly seen a jump from 66% to 78% as US physicians continue to use AI for documentation, billing codes, and clinical support.
But in this smoother transition, the transition from static systems to adaptive and intelligent healthcare platforms, the traditional EHRs do not have the capacity to adapt effectively. That is why many healthcare institutions have EMR development.
On that note, let’s see the future trends in EMR software and how it will impact the future of healthcare. So, without further ado, let’s get started!
EMR Software Trends Driving the Rise of ClinicalIntelligence
The future trends in EMR software will define how EMR software will evolve, and it will depend on the needs and requirements of healthcare practices and providers. Some of the current trends that are dominating the development are:
- Interoperability-First & Cloud-Native Architecture:
The rising dependency of data for care delivery and administration is increasing among patients. Due to this, your systems are becoming more dependent on other healthcare software systems. To improve connectivity with these systems, providers are demanding interoperability-first and cloud-native architecture. This will improve accessibility to the information in real-time, which could be accessed anytime and anywhere.
- API-Driven Ecosystems:
APIs have become easy to fetch information, which is why many development ventures are demanding API-driven ecosystems to improve connectivity. For instance, with open APIs, healthcare apps can plug into each other’s systems to exchange data in real-time. Some of the systems that you can connect with labs, pharmacies, RPM tools, and telehealth. Due to this, a single longitudinal patient record can be created, eliminating data silos, and faster care coordination can be achieved.
For modern EHR systems, it is important to have a scalable and future-ready system because, with time, the practice is bound to grow in patient flow. And for your system to be able to adapt to these growing needs, a scalable architecture forms the base, with cloud-native architecture defining the future EMR software trends.
The Role of AI in Custom EMR Development & Automation
AI in custom EMR development is the demand that is dictating the development trends in healthcare lately. This has been one of the major demands of healthcare providers as they are trying to make their EMR systems into intelligent clinical assistants that will help in care delivery as well as administration.
Some of the main features that are enabling this transition are automation, predictive analysis, generative AIs, etc. These features ensure accuracy in documentation processes and reduce manual data entry processes. Furthermore, automation and analytics features have had a significant impact on reducing clinicians’ burnout, and some studies even show a reduction in pajama times or after-hours for providers. For instance, according to ScienceDirect, ambient clinical intelligence decreased by almost 2.5 hours per week of off-hours documentation.
A core feature that is a constant demand of AI in custom EMR development is AI-powered clinical decision support systems (CDSS). Since they act as an assistant for healthcare providers, they help in medication prescriptions, diagnosis processes, care planning, etc., and other healthcare delivery procedures.
With this feature, providers can not only provide better care, but also adopt a holistic approach with access to a complete overview, where your AI-powered EMR system can itself analyze complete patient data and suggest appropriate care measures to derive the best possible patient outcomes.
Impact of Mobile Technology on EMR Accessibility & Care Delivery
Next-generation EMR systems are already here, and they have come as mobile-first EMR solutions. You see, almost everyone owns a mobile phone of some kind. A survey of the Pew Research Center showed that almost 91% of the adults in the US own a smartphone.
This stat might give you an idea about the use of mobile phones in the day-to-day lives of individuals. So, it makes perfect sense to allow providers to deliver care through smartphones and for patients to access care.
If implemented correctly, it can break free from desk-bound clinical workflows and enable the delivery of care with convenience. Also, with real-time access to patient data during hospital rounds, accessing it on mobile devices could enable timely care. Furthermore, a more personalized care delivery approach can be adopted, with easy access allowing providers to stay connected with the patients all the time. This proves to be a turning point in making care delivery better with proper preventive care measures.
This can only be achieved with mobile-first EMR solutions, as it is completely based on cloud and wireless technologies, enabling responsible care, further bridging the gap between care providers and patients.
Mobile-First EMR Solutions & Modern EMR Application Development
If you’re still wondering how EMR software will evolve in the near future, then you need to closely observe the impact of mobile technology on EMR application development. So, if you want to stay ahead of the curve, building a mobile-first EMR solution is a must. In this regard, here are some things that you need to know:
Most of you might confuse mobile-first EMR solutions with mobile-friendly EMR solutions. You see, mobile-friendly solutions are typically built on the desktop, but can be accessed on mobile devices. However, with a mobile-first EMR solution, you build the EMR software for the mobile ecosystem, but it can also be accessed over a desktop.
Now, though this might sound the same, with a mobile-first design approach, navigation, accessibility to features, and other aspects are designed with mobile phones as the primary device. Due to this, you have to prioritize handheld workflows over desktop-centric systems. The major difference comes in the screen size and how it operates, given different usability.
Having said that, one of the major advantages of mobile-first EMR solutions comes in the form of offline accessibility. Desktop systems work on the internet; however, with mobile phones, you can use the EMR system over your phones and do necessary tasks even without an internet connection. However, this does not completely eliminate the need for the internet; you will still need to rely on internet connections for synchronizing the data across the ecosystem.
Still, the convenience and performance optimization prospects with mobile-first EMR solutions can be huge and play a critical role in care delivery. However, to achieve this convenience, a clinician-focused UX must be adopted so that the usability of the software is easy, and even someone new to the software can use and navigate it smoothly.
Cybersecurity as a Core Requirement in Next-Generation EMR Systems
Future EMR technology is expected to make this healthcare IT ecosystem more connected and synchronized, where data sharing is much easier, accurate, and in real-time. Now, this increases the chance of data theft or cyberthreats, given the type of data you store and share from your system.
This is crucial data of your patients, which needs to be protected as part of their fundamental rights. And in connected environments, it is even more important as it is not just important to make your system secure, but also ensure that the bridge between your system and other systems is also secure.
One of the best practices of secure EMR software development is the implementation of zero-trust architecture. It is a cybersecurity framework that asks the user to verify themselves before allowing access to the features and data of the software. It minimizes the attack surface and prevents lateral movements by using micro-segmentation and least-privileged access to protect data, applications, and services.
You can also leverage blockchain technology to ensure data integrity inside your system. As blockchain technology keeps a record of every transaction, which can be traced and not erased, you can easily identify and address the security threats.
Also, while you’re riding the wave of AI in custom EMR development, you can even implement AI to detect threats. For instance, with AI embedded into your workflows, it can easily identify abnormal access patterns and prevent breaches by informing the admin or blocking the access of such users.
Key Characteristics of Next-Generation EMR Systems
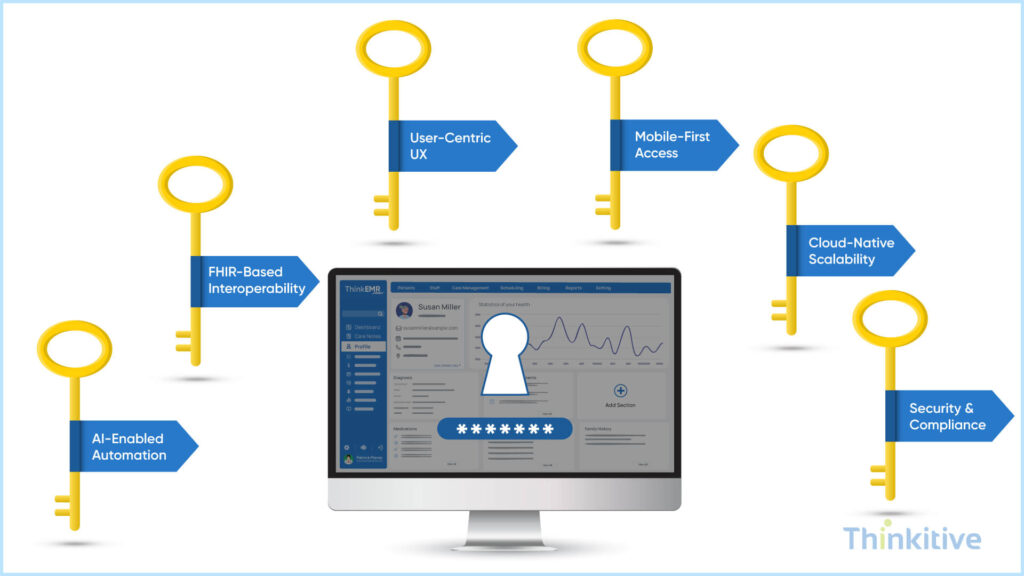
If you’ve made it this far into the article, then you now know some of the major trends dictating the future of EMR software. Furthermore, these next-generation EMR systems have some of the key characteristics that you need to know if you’re planning for custom EMR system development as well. On that note, here are some of the key characteristics:
- AI-Driven Insights Embedded into Clinical Workflows: As discussed earlier, AI-driven insights embedded into clinical workflows are one of the core characteristics of future EMR technology. The reason why this makes your EMR system a next-generation EMR system is that it bridges the gap between accessibility, and rather than being layered, it acts as a part of the system, making your system much more intelligent.
- Mobile-First & Device-Agnostic Access Across Care Settings: Another core characteristic of next-generation EMR systems is their ability to work seamlessly on smartphones, tablets, laptops, and desktops without compromising their functionality and security. This way, workflows stay more consistent across devices and reduce dependency on traditional devices. The advantage you get with this is that it improves responsiveness, efficiency, and continuity of care.
- Interoperable, API-First System Architecture: Data accessibility and sharing across systems will be another key characteristic of next-generation EMR systems. For this, the systems will be interoperable with API-first connectivity, ensuring seamless data sharing in real-time.
- High Performance, Security & Compliance Readiness: Given that the development will be new age technologies, the custom EMR systems are bound to be high performing, with enhanced security. Furthermore, given the ever-changing landscape of regulatory requirements and compliance, the next generation of EMR systems will be more flexible.
Despite these characteristics of next-generation EMR systems, the system will truly be futuristic when it continuously adapts to newer technologies. Since the technological and healthcare landscape is constantly evolving, it will prove to be one of the core characteristics of EMR systems.
Conclusion: What the Future Holds for EMR Software
EMRs are evolving from a data storage system into an intelligent care delivery platform that not only helps healthcare practices deliver data-driven, holistic care but also accurate and synchronized documentation. Due to this, the systems will be more personalized for providers in providing care to patients while accessing and receiving care.
Furthermore, with AI in custom EMR development, if implemented successfully, then it can be a pinnacle of deeper AI-human collaboration in care delivery. And since EMR systems have become the epicenter for healthcare practices, they will soon become central hubs within connected healthcare ecosystems.
On that note, I hope we’ve nudged you in the right direction about the future of EMR software and equipped you with insights for developing next-generation EMR systems. So, what are you waiting for? Get started with your EMR system transformation to an intelligent system. Let’s start with a system assessment and get your first free consultation.
Frequently Asked Questions
The future of EMR software is moving away from rigid, documentation-heavy systems toward intelligent, workflow-aware platforms. Future EMRs will actively support clinical decision-making, reduce administrative burden, and adapt to specialty-specific workflows. Instead of being passive data repositories, EMRs will become real-time clinical assistants that improve efficiency, care quality, and provider satisfaction.
Next-generation EMR systems are designed around usability, automation, and interoperability—unlike traditional EMRs that focus primarily on compliance and record-keeping. Modern systems leverage AI, mobile-first design, and modular architecture to streamline workflows, surface insights automatically, and integrate seamlessly with other healthcare technologies.
Healthcare organizations are realizing that one-size-fits-all platforms limit efficiency. The shift toward EMR application development tailored to specific specialties, care models, and operational goals allows providers to eliminate unnecessary features, reduce workflow friction, and scale functionality over time. Custom solutions also align better with evolving regulatory, data, and AI requirements.
AI is foundational to future EMR technology. From clinical documentation automation and predictive analytics to intelligent alerts and decision support, AI in custom EMR development enables systems to work proactively rather than reactively. AI transforms EMRs into adaptive platforms that learn from clinical behavior and continuously optimize workflows.
AI reduces burnout by minimizing manual tasks such as documentation, chart review, and repetitive data entry. Features like ambient clinical documentation, smart order suggestions, and automated coding allow clinicians to focus more on patient care. As future trends in EMR software evolve, burnout reduction is becoming a primary design goal—not an afterthought.
The impact of mobile technology on EMR usability is significant. Clinicians expect anytime, anywhere access to patient data, task management, and communication tools. Mobile access improves responsiveness, speeds decision-making, and supports care delivery beyond traditional clinical settings, driving higher adoption and satisfaction.
Mobile-first EMR solutions align with how clinicians actually work—on the move, across locations, and under time pressure. These solutions prioritize fast access, intuitive navigation, and context-aware interfaces, making them essential for modern workflows such as remote care, home health, and hospital rounding.
Modern EMR application development focuses on modular design, cloud-native architecture, and API-driven interoperability. This allows healthcare organizations to add new capabilities—AI tools, RPM platforms, analytics modules—without rebuilding the system. Flexibility and scalability are now core requirements.
As EMRs become more connected and data-rich, security challenges expand. Next-generation EMR systems must address threats related to AI models, mobile access, third-party integrations, and real-time data exchange. Advanced encryption, zero-trust architecture, continuous monitoring, and compliance automation are critical components of future-ready security strategies.
Future EMR technology is built around interoperability by design. Standards-based APIs, real-time data exchange, and ecosystem integration allow EMRs to connect seamlessly with labs, imaging systems, wearable devices, and care coordination platforms—enabling truly connected, longitudinal patient care.
Key characteristics include:
- AI-driven automation and intelligence
- Mobile-first and clinician-centric design
- Modular, cloud-based architecture
- Built-in interoperability
- Advanced analytics and reporting
These attributes define EMR software trends shaping the next decade of healthcare IT.
To understand how EMR software will evolve, look beyond records management. Future systems will synthesize data, predict outcomes, guide decisions, and continuously adapt to clinical behavior. EMRs will act as intelligent care platforms—supporting population health, personalized medicine, and value-based care rather than simply storing information.




