Intake to Discharge: Fixing the Broken Mental Health Patient Journey
In most mental health clinics, the mental health patient journey feels more like a hurdle course rather than a seamless journey. During every transition in the intake to discharge process, patients face disconnected care, repetitive questions, and disjointed transitions.
The result is a broken mental health care journey that leads to frustration, burnout, and low clinical outcomes. In addition, poor behavioral health care coordination across mental health clinics becomes another reason for these broken mental health workflows.
When there is a lack of coordination, the care teams can’t be on the same page and cannot view the updated patient profiles. This creates confusion and repetition, leading to a patient journey that is more chaotic than structured.
Furthermore, many mental health practices use a generic EHR, which is not designed to support the mental health care journey. They can handle all basic tasks, but with complex workflows and operations, they slow down care. These systems create silos rather than coordinating and connecting the care journey while limiting visibility.
However, this doesn’t have to be the reality, as a custom behavioral health EHR can easily streamline the whole process. Through mental health EHR mobile app development, clinics can build connected, mobile-first systems that simplify documentation and make coordination effortless across teams.
With unified systems, centralized documentation, and improved behavioral health care coordination, every step of the patient health journey is connected, consistent, and outcome-driven.
In this blog, we will dive into how EHR systems can improve the patient journey in behavioral health and the steps to improve continuity of care from intake to discharge.
Understanding the Mental Health Patient Journey
When it comes to every mental health patient’s journey, it starts at intake and ends with discharge. From the moment patients’ registers to the day they go out of the facility, every step requires a smooth transition and coordination.
However, if this coordination fails, the care, rather than being supportive, becomes fragmented. Here’s how each phase works and impacts patient engagement as well as care continuity in behavioral health:
1. Intake: Setting the Foundation
This is the first step that patients have to complete, and it helps providers set the course of the patient’s treatment. Here, providers enroll the patients and collect all the patient details, including demographic details, insurance information, consent forms, and initial mental health assessments. Without this step, providers can’t proceed with the next stage of the patient journey.
Moreover, if this step goes smoothly, then patient trust increases, and the chances of them dropping out are much lower. So, this step can be said to be the first impression of your clinic.
2. Assessment: Defining Needs & Goals
After the enrollment or intake comes the assessment phase, where providers evaluate the seriousness of the patient’s condition. With the help of validation tests like PHQ-9 and GAD-7, clinicians understand the patient’s state, finalize the diagnoses, and set treatment goals. In this, the groundwork for care personalization is established.
However, if the tests are not completed effectively, clinicians have to re-enter data manually, increasing the chances of errors and creating gaps in treatment.
3. Treatment: Driving Consistency & Progress
This is the stage where the actual care starts with medication management and patient progress tracking. Most importantly, this stage has the most significant impact on patient engagement. Without an integrated behavioral health EHR, tracking patient progress or ensuring timely follow-ups can become chaotic.
4. Discharge: Ensuring Continuity Beyond the Clinic
Finally, the discharge process summarizes outcomes, provides referrals, and ensures that care continues even after the patient leaves the facility. Unfortunately, many practices still handle this phase manually, leading to lost notes, incomplete summaries, or poor referral tracking.
A connected behavioral health care coordination system ensures that discharge summaries, continuity plans, and post-care referrals flow seamlessly, keeping patients supported long after their sessions end.
Read How an Automated Discharge Planning Prevents Readmissions
Read HereWhere the Journey Breaks: Common Gaps & Inefficiencies
Despite best intentions, most mental health practices struggle to maintain a smooth, connected care journey. Somewhere between intake and discharge, crucial information slips through the cracks, and both patients and providers pay the price.
Here’s where things often go wrong:
1. Disconnected Systems
Most behavioral health practices use multiple tools for scheduling, documentation, and billing, none of which communicate effectively. Intake data is often stored in one platform, while treatment notes are stored in another. This disconnect forces providers to piece together information manually, increasing the risk of errors and care delays.
2. Redundant Documentation
Re-entering the same patient demographics, history, and clinical notes across systems is not just frustrating, it’s time wasting. These redundant documentation loops slow down providers, reduce facetime with patients, and contribute heavily to administrative burnout. It’s a problem that automated mental health documentation workflows can solve instantly.
3. Manual Handoffs
When care teams still rely on paper-based discharge summaries or email attachments, critical details get lost in transition. A missing diagnosis code or incomplete referral can derail post-treatment continuity and even impact reimbursement accuracy. These manual handoffs are a major bottleneck to efficient behavioral health care coordination.
4. Lack of Continuity
Once a patient completes treatment, follow-up often becomes an afterthought. Without structured tracking or automated reminders, relapse prevention and long-term engagement fall through the cracks. True care continuity in behavioral health requires a system that supports ongoing communication and progress monitoring, not just documentation storage.
5. Poor Data Flow
Perhaps the biggest issue is that clinicians rarely get a unified view of the full patient history. Jumping between tabs, platforms, or paper files leads to fragmented insight and reactive decision-making. Without a consolidated data flow, personalization and proactive care become nearly impossible.
Above all else, these gaps don’t just slow down operations but also impact the final outcome tremendously. When mental health workflows are broken, the care continuity is affected, along with care quality, patient trust, and compliance.
The Cost of a Broken Journey
When data does not seamlessly flow across the whole mental health patient journey, it becomes more than just an inconvenience. It costs money, time, and care quality. Let’s understand the costs of these gaps in mental health care:
1. Lost Revenue & Efficiency
Most of the mental health practices use generic systems that are not connected seamlessly and not aligned with behavioral health workflows. This leads to clinicians constantly jumping between screens, losing time for patient care, and declining productivity. With this, the billable hours are also lost, along with the opportunity to earn more revenue.
2. Lower Patient Satisfaction & Engagement
When the EHR is not designed for documenting mental health details, patients have to repeat themselves in almost every visit. This breaks the trust and creates inconsistencies in communication. Furthermore, these inefficiencies lower patient engagement in mental health programs and increase dropout rates, directly impacting clinical outcomes and reimbursements.
3. Reduced Treatment Effectiveness
Disconnected systems mean that data remains siloed in multiple systems, scattering it. This means that providers lack a holistic view of patient profiles and, without a central record of therapy notes, medications, and assessments, designing an effective care plan is nearly impossible. It can also endanger patient safety, especially in complex or severe behavioral health cases.
4. Staff Burnout & Turnover
Another impact of a fragmented mental health patient journey is staff burnout. These systems force clinicians to record manually, increasing the already heavy workload. Because of this, clinicians spend more time on screen than with patients, contributing to burnout. Over time, it builds up, leading to turnover, costing clinicians more with recruiting and onboarding expenses while also breaking care continuity.
In short, a seamless mental health patient journey is essential for better patient outcomes. If it’s broken, clinicians have a hard time delivering effective care, and patients lose trust, dropping out of the ongoing care. So, clinicians need custom behavioral health EHRs tailored for improving mental health EHR workflows for better outcomes.
Fixing the Journey: How EHRs Should Support Every Step
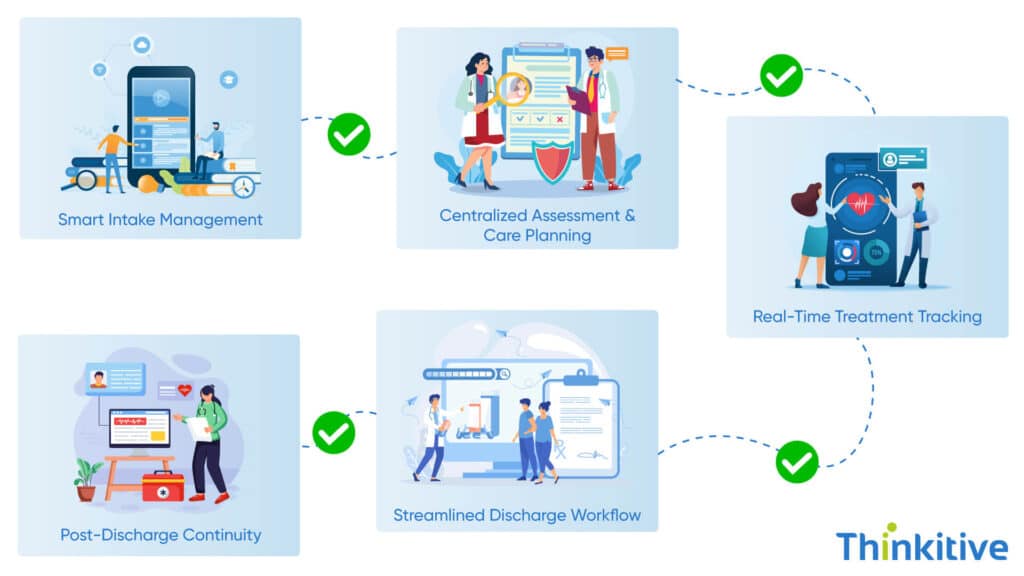
While for many mental health practices, broken mental health workflows have become the norm, it doesn’t have to be. A right behavioral health EHR can easily transform the intake to discharge process from chaotic to a more connected and continuous journey. Here’s how the EHR solves all the issues and fills the gaps:
1. Smart Intake Management
The journey begins with intake, and first impressions matter. Modern EHRs should offer:
- Digital intake forms that automatically sync with patient records, eliminating duplicate entries.
- Integrated pre-screening assessments like PHQ-9 or GAD-7 to capture baseline mental health metrics from day one.
This not only saves time but ensures clinicians have the right context for personalized care planning.
2. Centralized Assessment & Care Planning
Assessments should be structured, standardized, and seamlessly connected:
- Templates for psychiatric and psychological evaluations that guide clinicians through consistent documentation.
- Auto-population of patient data from intake to reduce redundancy and prevent errors.
Centralized care planning ensures that treatment goals and progress tracking are always based on complete, accurate data.
3. Real-Time Treatment Tracking
During treatment, information needs to flow effortlessly:
- Automated progress notes and measurement-based care tracking help clinicians monitor improvement over time.
- Dashboards provide quick visibility into patient status, compliance, and outcomes.
- Integration with teletherapy and group therapy scheduling tools keeps all sessions and communications in one unified system.
4. Streamlined Discharge Workflow
Discharge shouldn’t mean losing visibility over the patient:
- Auto-generated discharge summaries capture key treatment insights.
- Follow-up dates and referrals are flagged automatically, reducing the risk of missed care opportunities.
- Outcome reports are exportable for payers or audits, ensuring compliance and simplifying reporting.
5. Post-Discharge Continuity
True care doesn’t stop at the clinic door:
- Automated follow-up reminders and patient engagement portals keep patients connected after discharge.
- Remote monitoring tools allow clinicians to proactively detect relapse risks and intervene earlier, supporting sustained recovery.
By leveraging all these features, mental health clinics can easily streamline the mental health patient journey. Moreover, behavioral health EHRs eliminate silos, streamline mental health documentation workflow using mental health workflow automation, and improve both outcomes and patient satisfaction.
How to Streamline Intake to Discharge in Mental Health Practices
Find Out HereThe Role of Data in Building a Continuous Care Loop
In healthcare, data is what makes care effective and keeps it continuous. Without enough data, it’s nearly impossible and risky to provide care. That’s why, for practices, it is important to have tools such as EHR dashboards, analytics, and outcome reports to turn raw data into actionable insights.
Here is a table that shows how each of these tools helps in behavioral health EHR support continuous care loop, improve patient engagement in mental health, and ensure care continuity from intake to discharge:
| Data & Tool | Purpose / Insight | Impact on Care |
| EHR Dashboards | Visualize therapy progress, medication adherence, session attendance | Clinicians can quickly spot trends, intervene proactively, and adjust care plans |
| Analytics on Drop-offs | Identify points where patients miss sessions, skip assessments, or disengage | Helps reduce attrition and strengthens patient engagement |
| Outcome Tracking Reports | Aggregate clinical outcomes, PHQ-9/GAD-7 trends, and goal achievement | Enables data-driven decision-making and more personalized care plans |
| Predictive Analytics | Forecast relapse risk or non-compliance | Facilitates early intervention, improving continuity of care |
| Patient Engagement Metrics | Track portal logins, message response rates, and follow-up completion | Informs targeted engagement strategies and improves overall treatment effectiveness |
Learn How Data Keeps the Mental Health Patient Journey Seamless & Continuous
Discover MoreBuilding a Future-Ready Patient Journey

The future of behavioral health care is not just digital, it’s intelligent. By combining AI-driven insights with behavioral health-specific EHRs, practices can move beyond reactive care to proactive, personalized treatment.
1. AI for Predictive Care and Relapse Prevention
Modern AI tools can analyze patient data to forecast potential relapse risks, missed appointments, or symptom escalation. By identifying these early, clinicians can intervene before small issues become major setbacks, strengthening care continuity in behavioral health and boosting patient engagement.
2. Smart EHRs that Adapt to Provider Workflows
Next-generation behavioral health EHRs don’t force clinicians into rigid workflows. Instead, they adapt to each provider’s specialty and practice style, automatically prioritizing relevant assessments, therapy notes, or medication tracking. This flexibility ensures smoother documentation, reduces redundancy, and allows providers to focus on care, not clerical tasks.
3. Continuous Learning from Patient Data
Every interaction, assessment, and treatment outcome becomes a learning opportunity. AI-driven analytics can surface trends across patient populations, optimize care plans, and refine therapy protocols over time. Practices that leverage this continuous learning see better outcomes, smarter care delivery, and a truly patient-centered approach.
By integrating predictive AI, adaptive EHR workflows, and continuous data-driven learning, practices can transform the mental health patient journey from fragmented and reactive to seamless, proactive, and future-ready.
Conclusion
In a nutshell, mental health workflows are broken, and they significantly impact the mental health patient journey. In addition, generic EHRs exacerbate this issue further while making the intake-to-discharge process much more disconnected and chaotic.
That’s why adopting a custom behavioral health EHR is the right choice, as it has all the necessary features for fixing the broken behavioral health patient workflow. With intelligent automation and effective discharge planning, these systems create a more patient-centered journey, saving time, ensuring continuous and consistent care.
Want to explore how Thinkitive’s mental health EHR automates your patient journey end-to-end? Click here to book your free demo and see for yourself.
Frequently Asked Questions
In the mental health patient journey, there are multiple providers, therapy types, and ongoing evaluations; data often gets scattered across systems. This makes it too complex for generic EHRs to manage and capture this patient data, leading to disjointed workflows, manual coordination, and broken care continuity.
EHRs centralize patient information intake forms, assessments, therapy notes, and discharge summaries into one connected workflow. This ensures clinicians access real-time data, maintain consistent communication, and provide seamless, coordinated care across every stage of the patient journey.
Absolutely, a custom behavioral health EHR workflows automate repetitive documentation, auto-fills previously available patient data, and streamlines scheduling. This minimizes manual errors, reduces administrative burden, and allows clinicians to focus more on patient interaction and less on paperwork.
Measurement-based care uses standardized tools like PHQ-9 or GAD-7 to track progress objectively. Integrated within EHR dashboards, it helps clinicians adjust treatment plans in real time, enhancing engagement, accountability, and overall treatment effectiveness.
Automation and AI simplify discharge by generating summaries, setting reminders, and tracking referrals automatically. They also power predictive follow-ups, flagging relapse risks or missed appointments to ensure continuous post-care engagement and better long-term outcomes.




