Mental Health CPT Codes Your Generic EHR Doesn’t Support
What can be the single line between an approved or rejected claim? The answer is simple: medical coding, or more precisely, CPT (Current Procedural Codes) codes.
If you enter them accurately at the right place, then you can smoothly claim the reimbursements. However, if you make a single mistake and the claim gets denied or delayed and you lose revenue. This is because CPT codes prove that you provided the care and services, and act as a way to standardize billing.
While coding for physical care is complex, the complexity of mental health CPT coding is on another level. In mental health, there are multiple sessions from individual to group, with their own unique codes. This often confuses clinicians, leading to errors and costing clinics thousands of dollars.
Although there are tools, and many EHRs handle basic CPT code documentation processes, they fall short for more complex behavioral health CPT coding. However, the reality is that most behavioral health practices rely on these generic EHRs for medical billing, facing frequent denials.
That’s why upgrading to a specialized software through custom mental health EHR development, which is developed with a complete CPT code library and documentation tailored for behavioral health, is essential.
In this blog, we will explore how generic EHRs fail behavioral health CPT coding and the difference a best EHR for behavioral health billing and coding can make.
Let’s dive in!
The Role of CPT Codes in Mental Health Billing
Without accurate mental health CPT coding, clinics can’t have successful medical claims. These codes ensure that all submissions are standardized and that your practice is compliant with both insurance and regulatory requirements.
To put it simply, CPT codes are the proof that care was delivered and documented correctly. However, in mental health, the services come in multiple forms, and each has its own coding requirements. Common categories include:
- Diagnostic evaluation: Initial psychiatric assessments and intake evaluations.
- Psychotherapy sessions: Individual, group, or family therapy, often differentiated by session length.
- Crisis intervention: Emergency mental health care for urgent situations.
- Medication management: Prescribing or monitoring psychiatric medications.
For physical care billing documentation, it’s enough to have the session time and details of services provided. However, for behavioral health documentation, the clinicians need to capture details such as session time, patient response, and treatment notes to file the correct CPT code.
This complexity makes behavioral health CPT coding more challenging, and generic EHRs are not designed to handle this complexity. So, the role of CPT codes is quite essential in medical billing, and understanding this is the first step towards preventing claim denials, streamlining workflows, and ensuring compliance.
Where Generic EHRs Fail
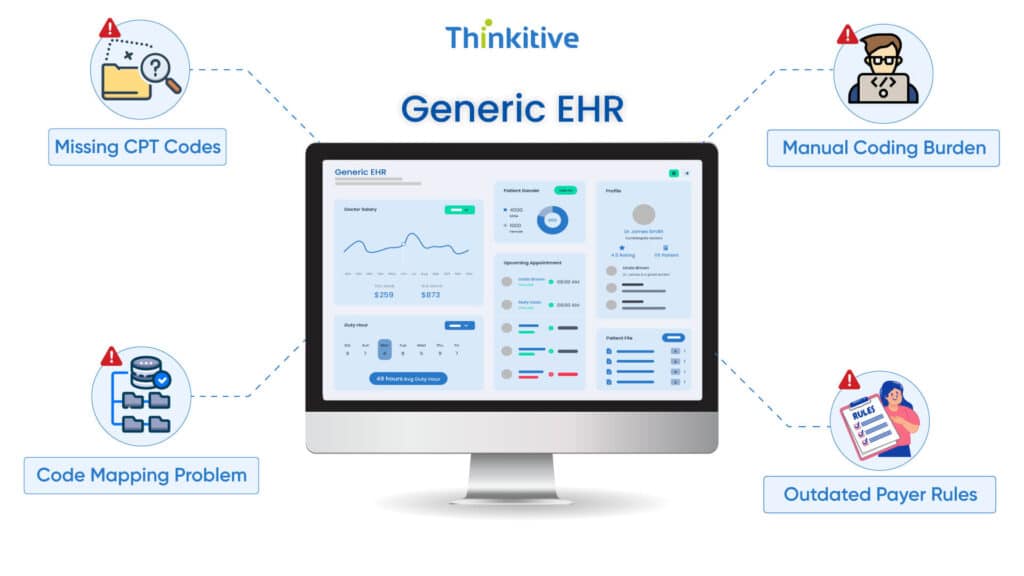
Although many generic EHRs can handle the most common CPT codes used in mental health therapy. But when it comes to more complex and detailed behavioral health CPT coding, they often fall short. So, the root cause of denials is not clinicians but the systems they use. Here are the gaps that fail the generic EHRs:
- Lack of Behavioral Health-Specific Code Libraries:
When it comes to coding, it’s not easy to remember every one of them, so a CPT code library is crucial, but generic EHRs lack a behavioral health-specific code library. This means it only includes common codes such as 90791 (Psychiatric Diagnostic Evaluation) or 90837 (60-minute Psychotherapy). Without having more critical codes built in, clinicians have to enter these codes manually, increasing the chances of errors and claim denials.
- Improper Code Mapping
Another issue is that generic EHRs don’t have the code mapping specific to therapy sessions, and they default to general medical procedure codes. This mismatch between clinical documentation and billing codes leads to coding compliance issues and delayed reimbursements.
- Manual Coding Burden
In the generic EHR, there is no automation for EHR coding for therapy sessions, which leads to clinicians entering codes manually. With the task added to their already existing workload, not only is productivity impacted, but the chances of CPT code documentation errors also increase.
- No Integration with Payer Rules
In healthcare, the payer requirements and CPT codes change constantly; however, generic EHRs don’t sync with the latest billing rules. As a result, providers end up using outdated or mismatched codes, leading to rejected claims and unnecessary revenue loss.
In short, generic EHRs built for generic medicine billing cannot manage the complexity of behavioral health billing. This means that without specialized features like a complete CPT code library, automated mapping, and payer integration, accurate coding is nearly impossible.
The Financial Impact of Missing Codes
Every missed or incorrect CPT code isn’t just an administrative error; it’s lost revenue. When a claim gets denied or delayed, it directly affects a clinic’s cash flow, causing unnecessary administrative strain.
For instance, if your practice faces even a 10% claim denial rate, that could translate to $5,000–$10,000 in lost revenue every month. And the worst part? Most of it stems from simple coding errors or outdated CPT entries that could easily be prevented with the right system.
But the financial impact doesn’t stop there. Each denied claim means more back-and-forth with payers, rework for your billing team, and delayed payments for clinicians. Over time, this not only leads to financial instability but also fuels clinician burnout. When providers spend hours resolving billing issues instead of focusing on patient care, frustration builds—and so does the pressure to cut corners.
In short, missing or incorrect CPT codes can quietly drain both your revenue and morale. The solution lies in smarter systems that don’t just record codes but understand the nuances of behavioral health billing.
Behavioral Health CPT Codes that Generic EHRs Commonly Miss or Mishandle
When it comes to behavioral health CPT codes, even the most advanced generic EHRs fall short. The reason is that their design is around medical procedures and not mental health sessions, crisis care, or group therapies.
That’s why many critical CPT codes are not supported by these systems and are misclassified, leading to misalignment with insurance documentation. Here’s a quick list of the CPT codes that are mishandled by generic EHRs:
| Category | CPT Code | Description | Common Issue in Generic EHRs |
| Diagnostic Evaluation | 90791 / 90792 | Psychiatric evaluation with or without medical services | Not available or mislabeled under physical exams |
| Psychotherapy | 90832 / 90834 / 90837 | 30-, 45-, and 60-minute sessions | Incorrect time mapping or documentation mismatch |
| Family & Group Therapy | 90846 / 90847 / 90853 | Family or group psychotherapy sessions | Not supported for multiple participants |
| Crisis Intervention | 90839 / 90840 | Crisis sessions (first hour and each additional 30 minutes) | Missing or inadequate time-tracking fields |
| Add-on Codes | 90785 | Interactive complexity or combined psychotherapy codes | Missing or incompatible with base codes |
So, when your EHR fails to recognize or correctly map those codes, the risks are greater than just billing delays; you lose visibility in the provided care. That’s where a custom mental health EHR steps in. Let’s understand how it handles CPT codes while preventing claim denials through accurate EHR coding.
How Custom Mental Health EHRs Solve the Coding Gap
Till now, you should have understood that generic EHRs were never designed for behavioral health billing. So, what the clinics need is a specialized EHR that understands how billing works in mental health and has all the needed tools to handle it properly.
That’s where a custom mental health EHR comes in. It has the most important feature that makes billing much simpler, and that feature is the built-in behavioral health CPT code library. This library has all the updated and complete CPT codes for psychiatric evaluation and psychotherapy, and automatically syncs with any new updates, keeping the clinic compliant.
Another feature that streamlines the billing procedures is automated payer-specific validation before the claims are submitted. With this, clinicians can verify whether or not each code is according to the insurer’s requirements, reducing the chances of denials.
Most importantly, the custom EHR solutions can suggest correct CPT codes based on the time spent in each session. It tracks the time and ensures that the right code is placed for a 45-minute Psychotherapy session, eliminating instances of incorrect code placements.
Finally, the best feature of the custom behavioral health EHR is real-time claim scrubbing. With this feature, checking the claims before they are submitted and pointing out the errors saves the time of fixing claims every time they are rejected.
In short, a custom mental health EHR fills out every gap left by a generic EHR and brings more features to the table, improving claims accuracy and acceptance rate.
Conclusion
For mental health billing, missing or incorrect mental health CPT codes are more than just an administrative blunder; they are financial drains. Moreover, generic EHRs make this already complex process more complicated and time-consuming
They don’t have the right CPT code library and only support basic codes, creating a situation where EHR creates more gaps than it fixes. So, the clinics need to change the EHR and adopt custom mental health EHRs to ensure accurate coding, documentation, and clean claim submission.
Ready to discover how custom EHRs manage this? Click here to talk to our experts and see how these systems maximize reimbursement and simplify mental health coding.
Frequently Asked Questions
Common mental health CPT codes include 90791/90792 for psychiatric evaluations, 90832/90834/90837 for psychotherapy sessions, 90846/90847/90853 for family or group therapy, and 90839/90840 for crisis interventions. These codes cover most therapy, assessment, and emergency care scenarios.
Generic EHRs are designed for general medical billing, not mental health workflows. They often lack specialized code libraries, fail to map therapy sessions correctly, and don’t account for session lengths or multi-participant therapies, causing behavioral health CPT coding gaps and higher claim denials.
Check your EHR’s documentation or vendor release notes for automatic CPT update support. Verify if it includes behavioral health codes, session durations, and payer-specific validations. Regularly auditing your behavioral health billing software against the current CPT code set ensures coding compliance and minimizes rejected claims.
Psychiatric evaluation codes (90791/90792) cover initial assessments or diagnostic evaluations, often including medical services. Psychotherapy codes (90832/90834/90837) are for ongoing therapy sessions, differentiated by duration. Accurate distinction ensures proper billing, compliance, and correct reimbursement for each type of service.
Yes. Automated claim scrubbing reviews codes, modifiers, and documentation against payer rules before submission. This reduces human error, prevents outdated or mismatched codes, and improves claim approval rates, saving administrative time and avoiding lost revenue from coding mistakes.
A custom behavioral health EHR provides preloaded CPT code libraries, automated session coding, payer-specific validation, and claim scrubbing. It reduces errors, prevents denials, saves clinician time, ensures coding compliance in mental health practices, and maximizes reimbursement, making billing workflows efficient and reliable for behavioral health practices.




